A 55-year-old female with a history of paroxysmal atrial fibrillation with multiple failed ablations, hypertension, chronic back pain, and a 100-pack-year smoking history presented to the ED via Mobile Stroke Unit (MSU) with a chief complaint of “blurry vision.”
The patient reported discontinuing her anticoagulation regimen (aspirin 81 mg daily) because she was receiving epidural injections for musculoskeletal neck pain. The patient reported experiencing left-sided chest pain which radiated to her left arm during an argument with her daughter 36 hours previously. The morning after, she awoke to circumferential left-arm numbness from her shoulder to her fingers accompanied by painless “blurry” vision that improved when she closed her left eye. These symptoms persisted for 24 hours, at which point she presented to the ED.
Physical examination upon her arrival was notable for a normal right eye, and a left eye with 20/70 visual acuity and an inferior nasal quadrantanopia. She also reported paresthesias in the V1, V2, and V3 branches of the left trigeminal nerve. Intraocular pressures were normal bilaterally.
An ECG showed a normal sinus rhythm. Computed tomography (CT) and CT angiography of the brain and intracranial vessels were negative for acute bleeding, aneurysm, or large vessel occlusion. A bedside ultrasound of the left eye was performed and was also normal. An MRI of the brain was subsequently performed and was also negative for acute pathology.
A dilated eye exam revealed findings concerning for branch retinal artery occlusion (BRAO). It is suspected that this finding was due to cryptogenic stroke in the setting of paroxysmal atrial fibrillation while the patient was not on anticoagulation.
The differential diagnosis of acute, painless vision loss necessarily mandates consideration of both intracranial and intraocular etiologies. BRAO often causes superior or inferior quadrantanopia, which can also be associated with damage to Meyer’s loop within the temporal horns of the brain, whereas central retinal artery occlusion (CRAO) is associated with damage to Baum’s loop within the parietal lobe.
CRAO may also present with amaurosis fugax, a common presentation of multiple sclerosis. Retinal hemorrhage and detachment may also present similarly, and giant cell arteritis must also be considered in patients older than 50.
Loss of partial or whole perfusion of the retina from either BRAO or CRAO mandates quick recognition in order to prevent permanent vision loss. CRAO can compromise the entire arterial supply of the retina, whereas BRAO is more localized. Causes include thrombotic and embolic events as well as impaired venous drainage and external ocular trauma. Severity of visual loss depends upon the area affected, and permanent vision loss can occur in as few as 90 minutes.
Emboli associated with CRAO and BRAO are generally caused by embolized cholesterol fragments (Hollenhorst plaques), which appear as a yellow, fuzzy spot within the artery. Emboli can also originate from cholesterol thrombi found on native or mechanical heart valves, which appear white on fundoscopic exam. Obstruction of the central artery in CRAO often results in the appearance of diffuse retinal pallor and edema associated with a “cherry red spot” at the macula, whereas a wedge-shaped area of retinal pallor is pathognomonic for BRAO. As shown in Figure 1, a portion of the patient’s superotemporal arcade was obstructed, causing an inferonasal visual field defect.
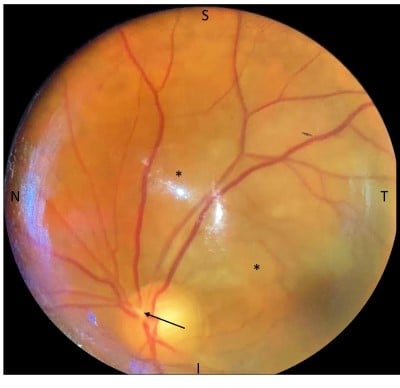
Figure 1. The patient’s left eye as seen on the fundoscopic exam, with nasal (N), temporal (T), superior (S), and inferior (I) orientation. It exhibits a cup-to-disc ratio of 0.4, normal optic disc nerve appearance without disc edema, plaque at proximal superotemporal arterial arcade (arrow) with corresponding area of wedge-shaped retinal edema (*), normal vessels, and normal periphery.
CRAO and BRAO are ocular emergencies mandating rapid diagnosis and management to prevent permanent loss of vision. Treatment options include ocular massage to attempt to relocate a lesion to a more peripheral area, and acetazolamide to reduce intraocular pressure via decreased aqueous humor production. Hyperbaric oxygen therapy has also shown promising results. While catheter-directed thrombolysis may be effective for CRAO, the smaller size and peripheral location of most BRAOs makes them less amenable to this therapy.
Our patient, unfortunately, presented on the third day of her visual symptoms, which limited treatment options. The patient was admitted to the cardiology service, with neurology making recommendations. During her admission, she noted symptomatic improvement in her vision. Serial troponins were negative; she remained in sinus rhythm. She was discharged on apixaban for paroxysmal atrial fibrillation. She declined placement of an internal loop recorder but agreed to have an MCOT cardiac monitor. At her four-week follow-up appointment, she continued to be in normal sinus rhythm while taking aspirin, statin, and apixaban. Unfortunately, she was unable to afford carvedilol, as she was spending $500 per month on prescriptions while waiting for insurance.