Back pain is one of the most common chief complaints in the emergency department. It is estimated that between 2002 and 2016, back pain was the primary complaint of 4.4% of all ED visits.
Additionally, 84% of all adults will have lower back pain at some point of their lives that can be acute (less than four weeks’ duration), subacute (four to 12 weeks’ duration), and chronic (greater than 12 weeks’ duration). More than 85% of these patients will have nonspecific musculoskeletal pain that can be treated with conservative management and multimodal analgesia.
However, not all back pain is simple lumbago, and as emergency physicians, it is crucial to be aware of more insidious causes of back pain and to be able to recognize red flag characteristics that, if overlooked, can lead to dire consequences.
Red flag historical features include pain greater than 6 weeks, history of trauma or intravenous drug use, and pain at night. Concerning symptoms include urinary retention, fecal incontinence, and saddle anesthesia. Frequently discussed “can’t-miss diagnoses” include cauda equina syndrome, conus medullaris, malignancy, and spinal epidural abscesses.However, in the evaluation of an undifferentiated patient in the ED, we must keep a wide differential.
Our case highlights a rare presentation of acute back pain.
Case
An 80-year-old female with a past medical history of multinodular goiter status post partial thyroidectomy, hypothyroidism, obesity, hypertension, hyperlipidemia, coronary artery disease, and supraventricular tachycardiapresented to the ED for evaluation of back pain onset one hour prior to arrival. Earlier that morning, she was bending down to feed her cat and as she was getting up, she developed paresthesias originating in her lower back radiating down to her bilateral lower extremities that was worse with movement. She also reported associated numbness. Recent outpatient workup for chronic lower back pain with MRI demonstrated findings significant for a synovial cyst localized at the L5 vertebral body.
On review of systems, the patient denied intravenous drug use, weight loss, recent trauma, saddle anesthesia, fecal incontinence, urinary retention, fevers, chills, headaches, chest pain, dyspnea, abdominal pain, nausea, vomiting, constipation, diarrhea, dysuria, hematuria, seizure-like activity, recent sick contacts, or recent travel.
On initial presentation, the patient’s vitals were blood pressure of 164/94 mmHg, pulse of 91 bpm, respiratory rate of 18, temperature of 37.1°C, and oxygen saturation of 96% on room air. The patient was laying on her right side, writhing in pain, and complaining of severe pain in her lower back and leg. On exam, the patient had exquisite tenderness to palpation localized to her lower back and lower extremities and decreased tactile sensation localized to her entire right leg as compared to the left leg. Lower extremities were cool to the touch and bilateral pedal pulses were absent on palpation and on Doppler.
A decision was made to administer 8 mg of morphine, which led to minimal relief of her symptoms. Due to the clinical concern for vascular or neurological etiologies, likely requiring emergent surgical intervention, presurgical labs were drawn including troponin, PT/INR, and type and screen. All lab results were unremarkable, except the initial high sensitivity troponin result significant for a value of 682.7. However, the patient had no ischemic changes on her ECG.
Given the patient’s sudden onset of back pain, past medical history significant for extensive cardiovascular comorbidities, cool extremities, and absent pedal pulses on physical exam, there was considerable concern for significant vascular compromise including aortic dissection, abdominal aortic aneurysm, and lower extremity ischemia. Point-of-care ultrasound study of the abdominal aorta showed absent flow in bilateral common femoral arteries, but no dissection flap or aneurysm (Figure 1).
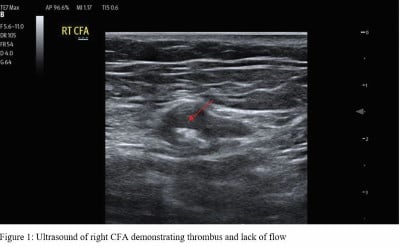
Due to concern for impending limb ischemia, the patient underwent emergent CT angiography studies of the chest, abdomen, and pelvis, which was significant for atherosclerosis and abdominal aortic occlusion extending into the bilateral common iliac arteries (Figures 2 and 3).
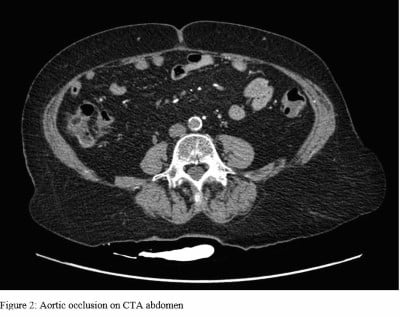
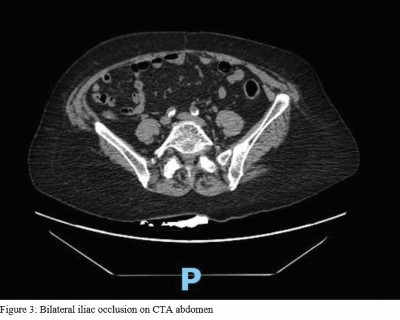
Vascular surgery was emergently consulted given the finding of an acute aortic occlusion and recommended anticoagulation with heparin with plan for emergent surgical intervention. After a long discussion about risks and benefits of surgical intervention, the patient consented for emergency surgery. The patient received left axillary to bifemoral bypass using polytetrafluoroethylene graft, which was well tolerated with minimal complications. She was subsequently admitted to SICU for hemodynamic monitoring and hourly neurologic checks.
Discussion
Back pain is a common chief complaint in the emergency department, and this case illustrates the importance of always having a wide differential. In this case, the patient’s lower back pain was a result of complete aortic occlusion extending into both lower extremities.
Complete aortic occlusion is an extremely rare condition but is potentially catastrophic if missed, as it can lead to loss of limb or life. This condition can be extremely difficult to diagnose as collateral circulation can allow for just enough perfusion to conceal acute ischemia for extended periods of time. Lumbar, intercostal, epigastric, circumflex iliac vessels, and visceral-systemic pathways of the celiac, superior, and inferior mesenteric arteries over time form extensive collateral networks that can perfuse the abdomen and pelvis.3
Acute occlusion of the aorta carries a mortality rate of 31-52%.4 The early mortality rate of acute occlusion of the aorta tends to be high, as it can initially be mistaken for cerebrovascular accident or a primary central nervous systemlesion, leading to a delay in diagnosis. This delay in diagnosis can lead to critical gastrointestinal malperfusion, renal infarction, and even paralysis resulting from malperfusion of the spinal cord, thereby increasing morbidity and mortality.5
Acute aortic occlusion can be caused by large saddle embolic occlusion of aortic bifurcation, acute in situ thrombosis of the atherosclerotic abdominal aorta, or acute occlusion of an abdominal aortic aneurysm.5 About 75-80% of cases of aortic occlusion present in the setting of extensive aorto-iliac occlusive disease.4 In their 2015 article, “A modern series of acute aortic occlusion,” Crawford et al.5 identified that 76% of cases of acute aortic occlusion were secondary to acute thrombosis, 7% secondary to embolic etiology, and 17% had indeterminate etiology.
Ischemic manifestations of aortic occlusion in patients with severe atherosclerosis can be precipitated by low flow states or dehydration. Common presenting features of acute aortic occlusion include acute claudication and uncontrolled hypertension. Acute claudication is characterized by cramping of buttocks, hips, and thighs that is reproducible with exercise and improves with rest.6
Moreover, acute aortic occlusion can also present with ischemic rest pain. Ischemic rest pain is a result of severe malperfusion of the lower limbs causing diffuse pedal ischemia. This type of pain is mainly localized to forefoot or toes but can present more proximally; the pain is worsened by elevation of the lower extremity and periods of recumbency, and does not improve with analgesia.6,7
It is highly likely that our patient was experiencing ischemic limb pain given the fact that her pain did not improve after administration of an appropriate weight-based dose of morphine. Aortoiliac occlusive disease is more prevalent in males, but its exact incidence and prevalence is unknown given that a majority of cases of peripheral artery disease are asymptomatic.6 Leriche syndrome characterized by claudication, impotence and sexual dysfunction, and absence of femoral pulses may be present in patients with severe aortoiliac occlusive disease.3 Of note, if identified appropriately, aortic occlusion can be diagnosed through sonographic means. Duplex scanning of the aorta, iliac, and common femoral arteries have a sensitivity of 91% and a specificity of 93% in the diagnosis of acute aortic occlusion.4
Surgical intervention is indicated in patients with debilitating claudication, pain at rest, and loss of tissue. The gold standard of surgical intervention for aortoiliac disease has been open repair, with patency rates as high as 72-90% at 10 years for aortobifemoral grafting. Open surgical options include aortobifemoral artery bypass grafting, aortoiliac endarterectomy, and extra-anatomic bypass.3 Aortobifemoral artery bypass grafting is the most common approach given its long-term patency rate. Also, it is a good option if legions spare the common femoral artery as it prevents introduction into the groin, reducing infections rates. Alternatively, aortic endarterectomy is rarely used and generally is reserved for focal stenosis of the distal aorta or proximal iliac arteries.3
Conclusion
In our case, the patient’s chronic atherosclerotic disease for the aortoiliac vessels eventually led to an acute occlusive episode, which manifested itself as severe lower back pain, paresthesias, numbness of the lower extremities, and absence of pulses on palpable and on Doppler. Ultrasound and angiography studies played a significant role in the eventual diagnosis, but clinical acumen and suspicion for vascular compromise steered us in the right direction with respect to making this life-saving diagnosis. Fortunately, our patient was discharged several days after her emergent surgical intervention with excellent functional status. Ultimately, this case presents a rare and life-threatening diagnosis for a common emergency department chief complaint and reminds us that thorough history and physical and broad differentials are of vital importance in our fast-paced work environment.
References
- Galliker G, Scherer DE, Trippolini MA, Rasmussen-Barr E, LoMartire R, Wertli MM. (2019, July 3). Low Back Pain in the Emergency Department: Prevalence of Serious Spinal Pathologies and Diagnostic Accuracy of Red Flags. The American Journal of Medicine. Retrieved October 4, 2022, from https://www.sciencedirect.com/science/article/abs/pii/S0002934319305406.
- Deyo RA, Weinstein JN. Low Back Pain. The New England Journal of medicine. 2001;344(5):363-370. doi:10.1056/NEJM200102013440508.
- Clair, D. G., & Beach, J. M. (2015, May). Strategies for managing AORTOILIAC occlusions: Access, treatment and outcomes. Expert review of cardiovascular therapy. Retrieved October 10, 2022, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4717320/.
- Efstratiadis, G., Kirmizis, D., Papazoglou, K., Economidou, D., & Memmos, D. (2004, January 1). The walking man with a completey occluded aorta. Academic.oup.com. Retrieved October 10, 2022, from https://academic.oup.com/ndt/article/19/1/227/1813293.
- Crawford, J., Perrone, K., Wong, V., Mitchell, E., Azarbal, A., Liem, T., Landry, G., Moneta, G., (2014, January 3). A modern series of acute aortic occlusion. Journal of Vascular Surgery. Retrieved October 11, 2022, from https://reader.elsevier.com/reader/sd/pii/S0741521413019885?token=11517D2B96F0FFE07A7FAD48673CD47C0A0562C7D1EA5EA9050E8D30ACC2760A5AD4C0E5DF587CD6F711F02D64090CB3&originRegion=us-east-1&originCreation=20221011154853.
- Brown, K. N., Muco, E., & Gonzalez, L. (2022). Leriche syndrome . National Center for Biotechnology Information. Retrieved October 11, 2022, from https://www.ncbi.nlm.nih.gov/books/NBK538248/#:~:text=Leriche%20Syndrome%20also%20commonly%20referred,and%20absence%20of%20femoral%20pulses.
- Santilli, J. D., & Santilli, S. M. (1999, April 1). Chronic critical limb ischemia: Diagnosis, treatment and Prognosis. American Family Physician. Retrieved October 11, 2022, from https://www.aafp.org/pubs/afp/issues/1999/0401/p1899.html.



