The most important mantra in the ED is: Perform resuscitative efforts to reverse threats to “life, limb, or eye.”
As it pertains to supratherapeutic INR reversal in the setting of anticoagulation, emergency physicians are most familiar with reversing anticoagulation due to warfarin in the setting of life-threatening trauma or intracranial hemorrhage.5,6There are, however, less documented reports of atraumatic ophthalmologic hemorrhage due to excessive anticoagulation.
The incidence of clinically insignificant subconjunctival hemorrhage in warfarin use is approximately 1 percent.2,4 To date, we have found only one case of spontaneous subconjunctival hemorrhage (SCH) requiring emergent anticoagulation reversal with intravenous vitamin K.3 More recently, in June 2021, there was a report of warfarin-associated SCH without supratherapeutic INR.1
This case appears to be the first documented case of supratherapeutic INR causing SCH and anterior segment ophthalmologic hemorrhage requiring emergent anticoagulation reversal with vitamin K and prothrombin complex concentrate. Thus, this report adds to the literature of diagnostic consideration that may require aggressive management when presented with atraumatic, frank ophthalmologic hemorrhage.
Case Report
A 96-year-old woman with a past medical history of deep venous thrombosis and pulmonary embolism on warfarin presented to our ED with a spontaneous left eye bleed. A family member reported the bleeding began two days prior and was associated with decreased vision. The patient, who was living independently, refused to seek care until her family member visited her on the day of her presentation and determined the frank bleeding required immediate care. The patient reported she took her medications as prescribed. She denied dizziness, lightheadedness, and syncope.
Vital signs were remarkable for a blood pressure of 89/53 mmHg with a normal heart rate. Left periorbital ecchymosis was noted. The patient refused to fully cooperate with visual acuity (VA) assessment in the right eye but was able to count fingers. Left-eye VA was to hand motion. Extraocular movements were intact in both eyes. Pupils constricted bilaterally, but there was a relative afferent pupillary defect in the left eye. Mild chemosis, as well as severe subconjunctival hemorrhage of the inferior aspect on the left, was noted. There was no proptosis. Bedside ocular sonography did not reveal a vitreous hemorrhage or retinal detachment.
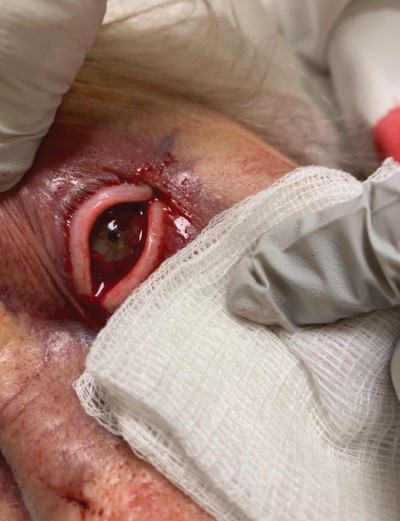
Image 1: Left eye with mild chemosis and subconjunctival hemorrhage over the inferior aspect without proptosis
Pertinent initial diagnostic studies included a complete blood count (CBC), coagulation profile, and immediate computed tomography (CT) scans with and without contrast of the orbit. An emergent ophthalmologic consultation was placed. The initial hemoglobin was 8.3, a three-point drop since the last in-house hemoglobin, which was about two years prior. Initial PT was over the threshold of detection (150), and thus the INR could not be calculated. Ophthalmology was consulted, and the patient was diagnosed with a severe left anterior segment hemorrhage, which may have required surgical exploration. Her pressure was repeated without crystalloid or colloid administration and found to be 127/56 mmHg.
Repeat coagulation profile after administration of vitamin K revealed PT 145, just under the threshold of detection, and calculated INR of 12.6. The patient continued to have extravasation of blood from the eye that was temporized with manual pressure. She maintained a normal heart rate and blood pressure.
Prothrombin complex concentrate (PCC) was given. Repeat studies showed PT 16.6 and INR 1.43. Transfer to a nearby tertiary center for further ophthalmologic monitoring and assessment was arranged. Within one hour of administration of PCC, the ophthalmologic hemorrhage ceased. The patient transfer was uneventful.
Discussion
Warfarin-induced SCH has been identified in the literature, and clinical judgment should guide emergent reversal of potentially sight-threatening ophthalmologic hemorrhage due to anticoagulation with PCC. Our patient’s vision was at baseline after anticoagulation reversal. It was also unclear whether the three-point decrease in hemoglobin was due to the acute hemorrhage or had been a more chronic process since the prior measurement observed during chart review was taken years prior. Ultimately, warfarin reversal was sufficient to reverse ophthalmologic bleeding, and no further surgical exploration or intervention was necessary. The patient also did not suffer from prothrombotic consequences of the reversal.
References
- Philip, A. M., Fry, M. V., Hermanson, M. E. & Kelly, L. D. Massive spontaneous subconjunctival hemorrhage in a patient on therapeutic warfarin: A case report. American Journal of Ophthalmology Case Reports (2021). https://www.sciencedirect.com/science/article/pii/S2451993621000402#bib8.
- Superstein, R. & Gomolin, J. E. S. Prevalence of ocular hemorrhage in patients receiving warfarin therapy. Canadian Journal of Ophthalmology (2000). https://www.scopus.com/record/display.uri?eid=2-s2.0-0022011065&origin=recordpage.
- Kleis, W., Hernandez-Denton, G. & Hernandez-Morales, F. An unusual complication of anticoagulant therapy: bloody tears. Boletin de la Asociacion Medica de Puerto Rico (1989). https://www.scopus.com/record/display.uri?eid=2-s2.0-0022011065&origin=recordpage.
- Leiker, L., Mehta, B. H., Pruchnicki, M. C. & Rodis, J. L. Risk factors and complications of subconjunctival hemorrhages in patients taking warfarin. Optometry (2009). https://pubmed.ncbi.nlm.nih.gov/19410227/.
- Alrajhi, K. N., Perry, J. J. & Forster, A. J. Intracranial bleeds after minor and minimal head injury in patients on warfarin. Journal of Emergency Medicine (2015). https://pubmed.ncbi.nlm.nih.gov/25440860/.
- Aguilar, M., Hart, R. G. & Kase, C. S. Treatment of warfarin-associated intracerebral hemorrhage: Literature review and expert opinion. Mayo Clinic Proceedings (2007). https://pubmed.ncbi.nlm.nih.gov/17285789/.



