A 57-year-old female is brought in to the emergency department after sustaining a gunshot wound to the right face. Initial assessment reveals facial swelling and large amounts of blood in the oropharynx, though she is initially stable on a non-rebreather. Her GCS is 12 (E4 V2 M6). Given the extent and nature of her injury, there is concern for impending airway compromise, and it is decided to take the patient to the OR for emergent tracheotomy.
For every ED physician the trauma resuscitation starts with the ABCs: airway, breathing, and circulation. The case scenario presented here may represent one of the more challenging airways you might ever encounter. The neck is the location of many vital structures. If a neck injury is missed during the initial stages of a polytrauma evaluation, it can result in increased morbidity and mortality. Penetrating neck injuries account for up to 5%-10% of all traumatic injuries.1 Mortality, particularly for vascular injuries, approaches 50%.2 Appropriate and timely management of neck injuries is a critical skill for the emergency physician.
Who Needs Immediate Airway Attention?
A fundamental principle of airway management is that earlier airways are generally easier airways. In traumatic neck injuries, an earlier intubation usually means an easier intubation because there is less time for airway distortion, swelling, and patient deterioration. The criteria for emergent airway management in penetrating neck trauma are outlined in Table 1.
Table 1. Criteria for Emergent Airway Management in Penetrating Neck Trauma3
| Stridor |
| Respiratory distress |
| Shock |
| Rapidly expanding hematoma |
The ideal approach for securing the airway is controversial. Options include rapid sequence intubation, oral intubation with sedation or local airway anesthesia only, blind nasotracheal intubation, direct fiberoptic intubation, retrograde guidewire intubation, cricothyrotomy, and placement of an endotracheal tube through an open wound in the neck (should one be available). Special caution is warranted for the patient with suspected blunt laryngeal injury, as orotracheal intubation may be impossible. Paralysis should be avoided in these patients, and a cricothyrotomy should be considered, with the appropriate tray and tools at hand. If there is a hematoma overlying the cricothyroid membrane, performing a cricothyrotomy is contraindicated. If time permits, tracheostomy would be the best approach.
Despite the multiple serious confounders, the familiarity of the emergency physician with RSI makes it the preferred technique in the majority of penetrating neck traumas (with appropriate scrupulous use of paralytics). Mandavia, et al, reporting on 58 patients with critical airway compromise in neck trauma, found that two-thirds of the airways were managed successfully with standard RSI. In this study, primary management of the airway via fiberoptic intubation by ENT specialists was attempted in 12 patients. Of these attempts, 3 failed this management, but then were successfully intubated using RSI.4
How Do I Manage an Open Wound in the Neck?
Open wounds in the neck require special attention. The first question is whether it violates the platysma muscle. If not, then primary repair and ED discharge can be arranged as long as there is no concern for blunt trauma to the adjacent structures in the neck.
On the other hand, if there is violation of the platysma, further evaluation is necessary. Avoid probing through the wound, as this may disrupt a clot. Do not blindly attempt to clamp vessels, as this also may cause further injury.
Direct compression can be attempted to control bleeding of an open neck wound. If that fails, consider placing a Foley catheter to tamponade the bleeding. Zone 1 injuries (below the cricoid cartilage) may involve the subclavian vessels; bleeding here is notoriously difficult to control. These patients may require emergent thoracotomy for hemorrhage management.5
Back to the Case
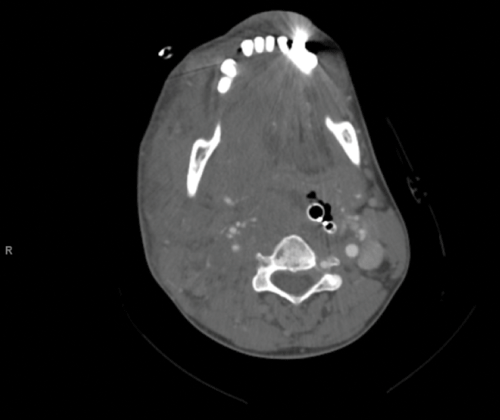
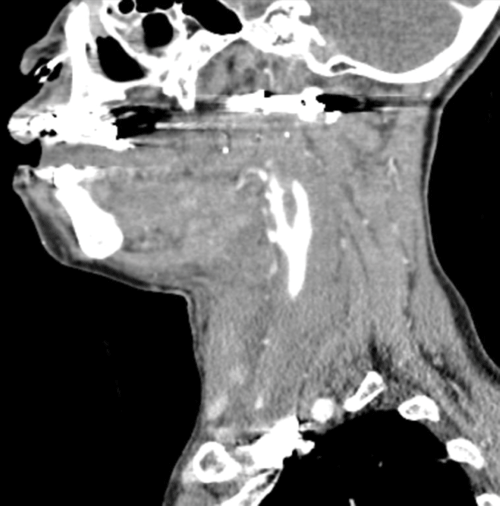
Prior to tracheotomy in the OR, an attempt at blind nasotracheal intubation is made and is successful. She is then taken for CT angiography of the neck and found to have complete occlusion of the right internal carotid artery, with possible transection (Image 1). The bullet is lodged in the right lateral mass of C1. The right neck structures are distended, displaced, and swollen due to edema and extravasation (Image 2). Contrasted CT head shows an acute small right MCA infarct with likely dissection. She is taken for endovascular repair and then transferred to the surgical ICU.
Approaching Vascular Neck Injuries
Table 2 demonstrates some of the classically taught “hard” and “soft” signs of penetrating neck trauma. If the patient presents with hard signs then s/he should go to the operating room as soon as possible. However, patients presenting with soft signs can still have serious injury and will always require further diagnostic testing.
Table 2. The “Hard” and “Soft” Signs in Penetrating Neck Trauma
| Soft signs |
| Non-expanding hematoma |
| 7th cranial nerve palsy |
| Hoarseness |
| Dysphasia |
| Subcutaneous emphysema |
| Hard signs |
| Hypotension in the ED |
| Thrill/bruit |
| Neurologic deficit |
| Uncontrolled bleeding |
| Expanding hematoma |
Modern CT scanners make helical CT angiography 90%-100% sensitive. This has overtaken conventional angiography as the diagnostic test of choice for penetrating neck trauma. A level II EAST (Eastern Association for the Surgery of Trauma) recommendation suggests that CT angiography or duplex ultrasound can be used in lieu of arteriography to rule out an arterial injury in penetrating injuries to zone 2 of the neck (between the cricoid cartilage and the angle of the mandible).6
When Should I be Concerned for Tracheoesophageal Injury?
Esophageal injuries often are clinically silent but carry a high morbidity because of mediastinitis. If repaired within the first 24 hours, the survival rate is greater than 90%. When surgery is performed after 24 hours the prognosis drastically worsens, with a survival rate of approximately 65%.7 EAST guidelines state that either contrast esophagography or esophagoscopy be used to rule out an esophageal perforation that requires operative repair. This diagnostic workup should be expeditious because morbidity increases if repair is delayed.
What About Cerebrovascular Injuries?
Biffl, et al, found four risk factors that independently conveyed a 41% chance of blunt carotid arterial injury. These were a GCS <6, presence of a petrous bone fracture, diffuse axonal injury, and either a LeFort II or III fracture (maxillary bone fractures). In the presence of all four of the independent factors for carotid injury, the risk of blunt carotid injury increases to 93%. Additionally, certain cervical spine fractures conveyed a 39% chance of vertebral vascular injury (Table 3).8
Table 3. Evidence and risk factors for traumatic cerebrovascular injury
| Signs and symptoms of blunt cerebrovascular injury |
| Arterial bleeding |
| Bruit |
| Expanding hematoma |
| Focal deficit |
| Ischemic stroke on secondary CT scan |
| Risk factors for blunt cerebrovascular injury |
| LeFort II or III fractures |
| C-spine fracture (C1-C3, or extending into the transverse foremen) |
| Diffuse axonal injury with GCS 6 |
| Basilar skull fracture with carotid canal involvement |
The criteria in Table 4 were developed to guide therapy according to the EAST guidelines. Injury grades I-II should be treated with either anti platelet or no-bolus heparinization (level II recommendation). Invasive therapy should be considered for injuries greater than grade II, as they rarely resolve with observation and heparinization (level II recommendation).
Table 4. Grading cerebrovascular injuries
| Grade I | Vessel irregularity <25% of luminal diameter |
| Grade II | Intimal flap, intraluminal hematoma with >25% narrowing |
| Grade III | Pseudoaneurysm |
| Grade IV | Vessel occlusion |
| Grade V | Vessel transection |
Case Resolution
The patient survives her injury and is discharged after a prolonged ICU stay, though with residual left-sided hemiparesis resulting from her arterial injury.
Learning Points
”” Avoid paralytics if you suspect laryngeal edema.
”” Avoid probing an open neck wound, as this may disrupt a clot.
”” Acute surgical management of penetrating neck trauma is dependent on the hard and soft signs.
”” Suspect tracheoesophageal injury, even in the asymptomatic patient.
”” Vascular injuries are more common than injuries to other structures.
”” CT angiography is a good starting point for stable penetrating injuries to all neck zones.
”” Don”™t forget the ABCs; always stabilize prior to imaging studies.
References
- Asensio JA, Valenziano CP, Falcone RE, et al. Management of penetrating neck injuries. The controversy surrounding zone 2 injuries. Surg Clin North Am 1991 Apr;71(2):267-296.
- Bladergroen M, Brockman R, Luna G, et al. A twelve-year survey of cervicothoracic vascular injuries. Am J Surg. 1989;157:483-486.
- Eggen JT, Jorden RC. Airway management, penetrating neck trauma. J Emerg Med 1993 Jul-Aug;11(4):381-385.
- Mandavia DP, Qualls S, Rokos I. Emergency airway management in penetrating neck injury. Ann Emerg Med 2000.
- Carducci B, Lowe RA, Dalsey W. Penetrating neck trauma: consensus and controversies. Ann Emerg Med 1986 Feb;15(2):208-215.
- Inaba K, Munera F, McKenney M, et al. Prospective evaluation of screening multislice helical computed tomographic angiography in the initial evaluation of penetrating neck injuries. J Trauma. 2006;61:144-1.
- Demla V, Shah K. Neck Trauma: Current Guidelines for Emergency Clinicians. EM Practice Guidelines Update. 2012;4(3):1-7.
- Biffl WL, Moore EE, Offner PJ, et al. Optimizing screening for blunt cerebrovascular injuries. Am J Surg. 1999;178:517”“522.