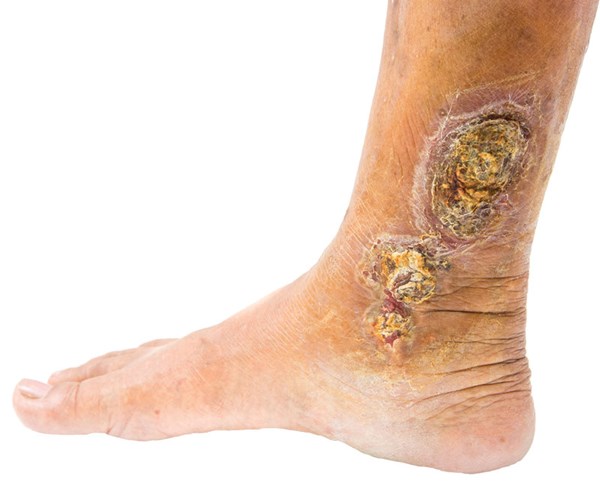
A 54-year-old male with a history of hypertension and morbid obesity presents to the emergency department (ED) with bilateral foot, ankle, and calf pain for the past 3 months. These symptoms are worse throughout the day and improve when he lies down at night. His exam is remarkable for symmetric swelling to the distal lower extremities with associated erythema and tenderness to palpation. A 4 cm shallow, irregularly shaped wound is noted in the left pretibial area with marked serous drainage. Pulses are palpable and equal in the lower extremities. How would you approach this patient?
Nonhealing wounds are often a physical manifestation of chronic illness and are defined by their unresponsiveness to initial therapy or persistence despite continued care.1 The majority of nonhealing wounds affect the lower extremities and are associated with vascular disease.2 Failure to recognize and initiate treatment for nonhealing wounds in the emergency department may increase morbidity and mortality as well as health care expenses for patients.3
Pathophysiology
Normal wound healing begins with an acute injury that damages the blood vessels, initiating the clotting cascade and platelet aggregation, which releases growth factors that draw neutrophils and macrophages into the injured area in order to destroy bacteria. The activation of macrophages also results in the release of growth factors and pro-inflammatory cytokines, which start the wound healing process.
In a chronic wound, the neutrophils and macrophages continue to secrete inflammatory cytokines that destroy the wound matrix and impair connective tissue deposition. This chronic inflammatory state may be exacerbated by repetitive trauma, local tissue ischemia, necrotic tissue, and a heavy bacterial burden, which is self-sustaining and prevents wound healing.
Approach to Evaluation
A thorough history and physical exam will help differentiate between venous or arterial insufficiency and diabetic neuropathy. When interviewing a patient, it is important to ask how long the wound has been present, whether the wound is changing in any way, how painful the wound is, and what therapy has been tried already, if any at all.3,4
Look
The examination of the lower extremity should begin with the general appearance of the legs.
- Evaluate the location, length, depth, and shape of the wound. Wound characteristics vary by etiology, but nonhealing wounds typically have a rounded edge and calloused appearance.
- Proximity to or involvement of underlying tendons, nerves or arteries should be assessed, as well as the presence of foreign bodies.
- Enlarged palpable veins (varicose veins), as well as dark red or purple discoloration can be characteristic of venous insufficiency.
- Hemosiderin staining (dark red or brown) is a cardinal sign of venous insufficiency in contrast to cellulitis, which is typically bright red.
- Thin, shiny, pale skin with an absence of hair growth, and thickened and/or brittle nails can be a sign of arterial insufficiency or diabetic neuropathy.
- Autonomic dysfunction associated with diabetes leads to decreased secretions and results in dry, cracked, and calloused skin.3
- A nonhealing wound represents a chronic inflammatory state, and mild surrounding erythema is expected. Cellulitis should be considered only if the inflammation or erythema is noted >1 cm from the edge of the wound. Other clues to infection include drainage, foul odor, worsening pain, and rapid progression.4
Feel
- Dead tissue may need debridement for accurate assessment of the wound base.
- Hypothermic skin suggests arterial insufficiency, normothermic skin is common with venous insufficiency, and hyperthermic skin is typical of cellulitis.
- Edema may be pitting or non-pitting and is typically symmetric.
- If pulses are not palpable, they should be identified and marked via Doppler ultrasound.
- Delayed capillary return may indicate arterial insufficiency, whereas rapid return may be seen in cellulitis.
- Neurologic examination should include light and sharp sensation, 2-point discrimination, and proprioception.
Special Examination Techniques
- Ankle Brachial Index (ABI): The ABI is the ratio of lower extremity to upper extremity systolic blood pressure. ABIs should be performed on patients with leg ulcers, as clinical examination findings are not independently sufficient to include or exclude arterial disease. 5,6 (See Table 1)
- Probing: The depth of the wound should be assessed by inserting a sterile (ideally metal) instrument into the wound. If the probe reaches bone, osteomyelitis should be strongly suspected.
- Elevation: Simple elevation of the lower extremity can provide valuable information.
- Pain related to venous insufficiency is worsened in the dependent position and lessened with elevation.
- Pain related to arterial insufficiency is lessened in the dependent position and worsened with elevation.
- Erythema from dependent rubor may fade with elevation, as opposed to cellulitis in which the erythema persists despite elevation.
Table 1. Ankle Brachial Index (ABI)
| Normal | >0.96 |
| Mild Obstruction | 0.71-0.96 |
| Moderate Obstruction | 0.31-0.71 |
| Severe Obstruction | <0.31 |
Diagnostic Workup
The diagnosis of a nonhealing wound is largely clinical. Diagnostic studies should be tailored to determine the underlying etiology. Once the diagnosis of a nonhealing wound is made, the provider needs to determine if the wound is infected, and to what extent.
For suspected infection, consider:
- Wound biopsy for culture analysis is the reference standard for the diagnosis of infected tissue and should be obtained when able, especially if topical or systemic antibiotics will be initiated. Avoid swab cultures.
- A normal erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) in a low risk patient population provides reassurance; however, osteomyelitis cannot be ruled out with normal results.7
- The white blood count is not helpful in the evaluation of osteomyelitis.7
- An abnormal plain radiograph in the correct clinical setting increases the likelihood of osteomyelitis but cannot definitively rule-in or rule-out the diagnosis.8
- Magnetic Resonance Image (MRI) is the test of choice for evaluation of osteomyelitis.8-9
Treatment and Disposition
Most patients with chronic lower extremity wounds can be discharged and managed on an outpatient basis. Long-term management requires lifestyle modification, optimization of comorbidities, weight loss, tobacco cessation, glucose control, improved nutrition, and adherence to multidisciplinary wound care team recommendations.10-13
Compression increases wound healing rates and is the mainstay of pain management for venous ulcers.5 Note that compression should be avoided if an ischemic ulcer is suspected! Topical steroid cream may reduce itching and irritation if there is surrounding eczema or stasis dermatitis. Otherwise, additional pain control can be accomplished with topical analgesics, NSAIDs, gabapentin, and/or opioids.14 All wounds should be kept warm and protected from injury using padding, thick socks, and hard shoes.
There is some evidence to suggest that topical antibiotics such as cadexomer iodine, mupirocin, and bacitracin promote wound healing, particularly in venous leg ulcers.15 Empiric antibiotics, on the other hand, have not been shown to improve wound healing and should therefore only be used only in cases of suspected infection.
Case Discussion
The case described a typical presentation of a venous insufficiency ulcer. This patient”™s risk factors included hypertension and obesity. Other clues included worsening pain throughout the day and relief with elevation as the patient lies down at night. There were no signs of infection, so management consisted of absorptive dressings, compression, and outpatient follow-up.
Conclusion
Nonhealing wounds are the byproduct of prolonged and complex disease processes. Though chronic in nature, they can pose acute threats to life and limb. Differentiating the signs and symptoms of acute illness from the expected course of a chronic nonhealing wound within the emergency department can be critical to achieving improved outcomes and quality of life.
References
- Greer N, Foman NA, MacDonald R, et al. Advanced wound care therapies for nonhealing diabetic, venous, and arterial ulcers: a systematic review. Annals Intern Med. 2013;159(8):532-542.
- Forster R, Pagnamenta F. Dressings and topical agents for arterial leg ulcers. Cochrane Database Syst Rev. 2015;6:Cd001836.
- Hartoch RS, McManus JG, Knapp S, Buettner MF. Emergency management of chronic wounds. Emerg Med Clin North America. 2007;25(1):203-221.
- Gardner SE, Frantz RA, Doebbeling BN. The validity of the clinical signs and symptoms used to identify localized chronic wound infection. Wound Repair Regen. 2001;9(3):178-186.
- O'Meara S, Cullum N, Nelson EA, Dumville JC. Compression for venous leg ulcers. Cochrane Database Syst Rev. 2012;11:Cd000265.
- Khan NA, Rahim SA, Anand SS, Simel DL, Panju A. Does the clinical examination predict lower extremity peripheral arterial disease? JAMA. 2006;295(5):536-546.
- Harris JC, Caesar DH, Davison C, Phibbs R, Than MP. How useful are laboratory investigations in the emergency department evaluation of possible osteomyelitis? Emerg Med Australas. 2011;23(3):317-330.
- Kapoor A, Page S, Lavalley M, Gale DR, Felson DT. Magnetic resonance imaging for diagnosing foot osteomyelitis: a meta-analysis. Arch Intern Med. 2007;167(2):125-132.
- Butalia S, Palda VA, Sargeant RJ, Detsky AS, Mourad O. Does this patient with diabetes have osteomyelitis of the lower extremity? JAMA. 2008;299(7):806-813.
- Freiman A, Bird G, Metelitsa AI, Barankin B, Lauzon GJ. Cutaneous effects of smoking. J Cutan Med Surg. 2004;8(6):415-423.
- Health Quality Ontario. Management of chronic pressure ulcers: an evidence-based analysis. Ont Health Technol Assess Ser. 2009;9(3):1-203.
- Vander Straten M, Carrasco D, Paterson MS, McCrary ML, Meyer DJ, Tyring SK. Tobacco use and skin disease. Southern Med J. 2001;94(6):621-634.
- Wilcox JR, Carter MJ, Covington S. Frequency of debridements and time to heal: a retrospective cohort study of 312 744 wounds. JAMA Derm. 2013;149(9):1050-1058.
- Briggs M, Nelson EA, Martyn-St James M. Topical agents or dressings for pain in venous leg ulcers. Cochrane Database Syst Rev. 2012;11:Cd001177.
- O'Meara S, Al-Kurdi D, Ologun Y, Ovington LG, Martyn-St James M, Richardson R. Antibiotics and antiseptics for venous leg ulcers. Cochrane Database Syst Rev. 2013;12:Cd003557.