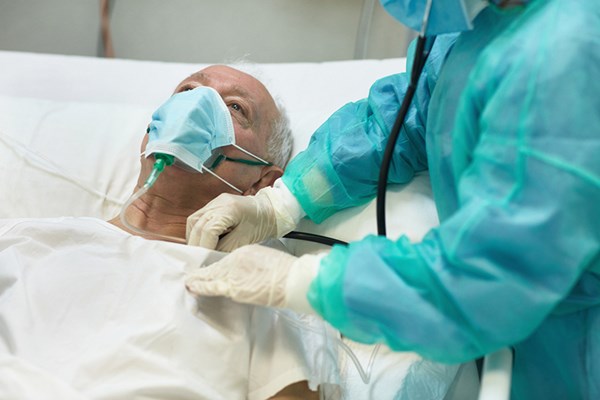
I know you hate the oxygen mask. Do you know how much I wish you didn't need it?
The first day, I tried reasoning with you.
Please keep your mask on. I know your mouth is dry, but as soon as you take the mask off, your oxygen level drops to 68%. In seconds. I know you don't feel it. But it does.
Day 2, I tried the firm approach.
Stop taking your mask off. STOP IT. It's the only thing keeping you alive.
Finally, on the third day, I was mean.
Sir, if you keep taking that off, you will die. Is that what you want? You want to die?
Then, back to pleading, like with a child who doesn't want to go to bed yet or a grandparent who has suddenly forgotten how to chew their food. I was pleading with you because I knew whatever was making you take the mask off wasn’t logical. You were thirsty; I saw your cracked, dry lips and your stunned expression as the oxygen blew forcefully into your face with each breath.
But the last time someone snuck you some orange juice, you choked on it and threw up into your mask. You remember? You couldn't even swallow it because of how out-of-breath you were. Remember that? And I'd yelled at them. I yelled at the nurse who gave you the juice because the choking noises made me panic. She couldn't bear to keep listening to you beg for juice or water or something, anything, but after three days of 12-hour shifts with my computer close to your bed, 8R, I grew attached to you. So when I looked up and saw you choking, spluttering, your face wet and gagging, your oxygen dipping, I panicked, I yelled, and I was mean.
Then I tried all approaches at once. Finally, I taped the mask to your face. Just regular silk tape. It probably hurt a little bit. I said matter-of-factly, If you take this mask off, I will have to put a tube down your throat to help you breathe and you will probably die on the ventilator. If I don’t find you in time to put a tube down your throat, you will die anyway. Please stop taking your mask off. Then I walked away.
At one point that last day, we grabbed the airway cart and I got ready to intubate you. You were hypoxic and confused and begging not to be intubated. We’d had conversations just earlier that day where, in a much clearer state of mind, you had firmly established you wanted to be intubated if need be, so I knew it was the right thing to do. But still, I felt a great weight in my chest as I continued preparing for the intubation around you, pretending I couldn't hear your desperate pleas. I was trying to stay focused, checking and double-checking that I had everything I needed right next to me, watching your oxygen saturation ebb lower and lower. But, at the last minute, someone else must have died because we were able to find a real BiPAP machine (not the "McGuyver'd" version of a CPAP mask that I had made) and your oxygen climbed back up to 96%. For the first time in days, you looked comfortable. You relaxed. When I walked by your bed to check on you, you gave me a thumbs up.
But then a bed finally opened up for you on the floors, a semi-private room you got to share with just one other person. Those rooms upstairs have bright windows, wider beds, TVs – they are practically spas compared to the beeping, grunting turmoil of the ED. Fewer people walking in and out looking for supplies; there’s less movement, less noise, a lower sense of urgency in general.
I imagine you felt a little more freedom now that you knew I wasn't there to yell at you, and you took off your mask.