Treating a rash that follows no pattern and appears after a vacation? Check for cutaneous larva migrans.
Case
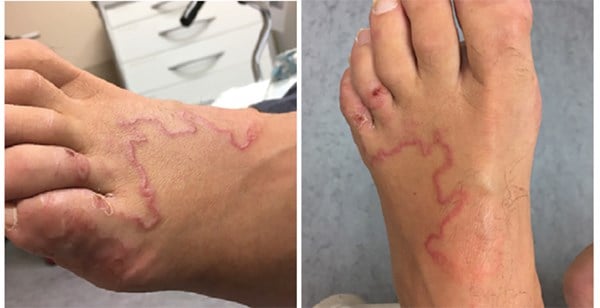
A 59-year-old male without any past medical issues presented to our ED with a pruritic rash for 2 weeks. He was initially seen by his family doctor after it had not responded to a course of over-the-counter athlete's foot cream. He was referred to the ED for IV antibiotics by his family doctor due to concerns of a worsening infection spreading up his foot. The serpiginous erythematous rash did not follow the course of any of the superficial veins on his foot. In addition, the patient had a macerated rash that extended beneath the 5th toe, and scabs were present on the dorsum of 4th and 5th toes.
The visual diagnosis was clinched by an experienced clinician with one question: Where did you vacation recently?
DISCUSSION
Cutaneous larva migrans (CLM) or Erythema Larva Migrans is a dermatitis caused by the migration of parasitic nematode larvae of hookworms within the epidermis.1 Hookworm-related cutaneous larva migrans (HrCLM) has been another suggested name.2 Humans are accidental hosts who often acquire this infestation while walking barefoot on sand that contains feces of cats or dogs that contain eggs of the infectious form of the larvae.2-4 A skin scab on the lower extremities typically marks point of entry and precedesthe characteristic serpiginous rash that later appears1. The rash itself develops over days to months with a mean time to onset of 5-15 days. Incubation period of the larva ranges from 7 days up to 7 months.1, 2, 5 Typical symptoms include rash, pruritis, and a secondary bacterial infection due to frequent itching. Humans are not natural hosts and the larvae die within several weeks to several months (rarely taking up to one year) as they are unable to penetrate the host’s dermis and migrate to deeper layers to complete their life cycle.5 Human intestinal hookworms like Ancylostoma duodenale and Necator americanus can cause a similar skin eruptions however the rash associated with these infections are shorter-lived as the parasite is able to penetrate the dermis to complete its life cycle.5, 6 Another rarer condition with similar symptoms is Cutaneous Pili Migrans that is caused by larvae migrating via hair follicles through the dermis.7
The most common hookworms species that cause CLM are Ancylostoma carinum (dog hookworm) and Ancylostoma braziliensis (cat hookworm), and are seen commonly in the southern United States (US), Central and South America and the Caribbean. Other hookworm species known to cause CLM are Cinaria stenocephala, Ascaris species, Necator americanus, and Bunostomum phlebotomum.2, 5, 6 The hookworm life cycle begins when an adult worm lays eggs in the intestine of their natural hosts, most commonly cats or dogs. The eggs follow their natural cycle forming first the noninfectious rhabditiform larvae, which then molts into the infectious filariform larvae in about 1 week.6 Humans are often infected after walking barefoot on sand contaminated with dog or cat feces that contains excreted larvae. They may also latch onto clothes and then burrow through the skin.2, 5
Without treatment the rash and pruritus resolves 2 weeks after onset but has been reported to last up to 1 year in rare instances.2, 5 Rarely non-human hookworm larvae can penetrate deeper, past the dermis, and can cause a peripheral eosinophilia and eosinophilic pulmonary infiltrates.2, 8 The most common sites of entry are the feet and buttock; however, cases can also be seen in the areas between fingers and toes and on the abdomen. Diagnosis is generally made clinically and microscopy can be used to help identify larvae. Skin biopsy is generally not recommended as it may cause worsening local reaction and has not been shown to consistently show the presence of larvae.
TREATMENT
First line therapy is with oral ivermectin 200 mcg/kg daily for 1-2 days. Albendazole and mebendazole are second-line agents (Table 1). Cure rates with ivermectin are between 94-100%.3, 8, 9 Albendazole 400 mg once daily with a fatty meal (for better absorption) for 3 days can also be prescribed (Table 1).3, 8, 9 Associated cutaneous folliculitis will require up to 5-7 days of therapy at the same dosage.2 Topical agents such as albendazole 10% cream and thiobendazole 15% cream (not currently available in the U.S.) are less effective7. Antihistamines may be considered for symptomatic relief.
Differential diagnoses to consider in any returned traveler with a primary cutaneous presentation include other infestations such as scabies, lichenoid eruptions like phyto-photodermatitis, zoster, jellyfish stings, arthropod bites, and other superficial skin and soft tissue bacterial and fungal infections.1,4
CONCLUSION
Our patient had vacationed in the Caribbean about 6 weeks prior to presentation. He recalls frequently walking barefoot on the beaches. He initially thought his rash was caused by athlete’s foot, and his family doctor had also considered thrombophlebitis or a cellulitis. Further history provided in the ED revealed that the rash started about one week after returning from his vacation and had slowly progressed over the following days. A relative who was with him on the vacation had similar lesions. He was prescribed albendazole 400 mg once daily for a 3-day course.
Table 1: Recommended treatment for Cutaneous Larva Migrans.
|
ANTIHELMINTH AGENT |
PEDIATRIC DOSAGE |
ADULT DOSAGE |
COMMON SIDE EFFECTS |
|
Ivermectin
Dispensed as 3mg tablet
|
Age >15 yrs only 200 mcg/kg PO once daily for 1-2 days |
200 mcg/kg PO once daily for 1-2 days |
Mazzotti reaction (Urticaria, facial swelling, fevers, tachycardia, tender lymphadenitis), nausea/vomiting/diarrhea, anorexia |
|
Albendazole |
-Weight <10 kg 200 mg PO once daily for 3 days -Weight > 10 kg 400 mg PO once daily for 3 days |
400 mg PO once daily for 3 days |
Headache, increased liver enzymes |
|
Mebendazole |
Age >2yr 100mg PO twice daily for 3 days or 500mg as a single dose |
100mg PO twice daily for 3 days or 500mg as a single dose |
Mostly GI – Abdominal pain, nausea, anorexia, flatulence, hepatitis. |
TAKE-HOME POINTS
- Skin eruptions are common in returned travelers and the differential is broad ranging from bites, stings, infestations, and infections. CLM is one of the leading causes of dermatologic disorders observed in returned travelers.10
- Visual diagnosis is important in any skin rash. This particular rash does not follow the veins and has a characteristic serpiginous appearance and is commonly seen on the lower extremities and buttock.
- Consider CLM in travelers that have walked barefoot on beaches located in tropical climates in South America, the Caribbean, and Africa.
- The mean time to onset of rash is 5-15 days with incubation period ranging from a week to 7 months.
- Eradication is most effective with ivermectin (94-100% resolution). Albendazole/mebendazole are other oral alternatives depending on medication availability and patient’s age.
References
-
- CDC - DPDx - Zoonotic Hookworm. Cdc.gov. https://www.cdc.gov/dpdx/zoonotichookworm/index.html. Published 2019. Accessed June 16, 2020.
- Hochedez P, Caumes E. Hookworm-related cutaneous larva migrans. Oxford Academic; 2007. p. 326-333.
- Bouchaud O, Houzé S, Schiemann R, et al. Cutaneous Larva Migrans in Travelers: A Prospective Study, with Assessment of Therapy. Vol. 31. 2000:493-498. 202013:10:05.
- Freedman DO, Weld LH, Kozarsky PE, et al. Spectrum of disease and relation to place of exposure among ill returned travelers. N Engl J Med. 2006;354(2):119-130.
- Edelglass JW, Douglass MC, Stiefler R, Tessler M. Cutaneous larva migrans in northern climates: A souvenir of your dream vacation. Vol. 7. 1982:353-358.
- CDC - Hookworm - Biology. https://www.cdc.gov/parasites/hookworm/biology.html. Published 2019. Accessed June 16, 2020.
- Luo DQ, Liu JH, Huang YB, He DY, Zhang HY. Cutaneous pili migrans: A case report and review of the literature. Vol. 48. 2009:947-950.
- Weller P, Leder K. Hookworm Related Cutaneous Larva Migrans. Uptodate.com. https://www.uptodate.com/contents/hookworm-related-cutaneous-larva-migrans. Published 2019. Accessed June 16, 2020.
- Sherman SC, Radford N. Severe infestation of cutaneous larva migrans. J Emerg Med. 2004;26(3):347-349.
- Hochede P, Caumes, E. Hookworm‐Related Cutaneous Larva Migrans. J Travel Med. 2007; 14(5):326-33.