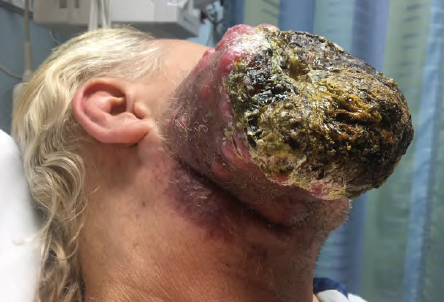
Challenges with health care literacy, lack of insurance, and simple human fear can sometimes lead patients to delay seeking help - or even deny a problem exists. Tread lightly to offer the best care in these cases.
A 56-year-old male with a past medical history of active tobacco use and remote intravenous heroin use presents to the ED complaining of a 2-month history of a rapidly enlarging mass on his right cheek. He states the lesion began as a “small pimple” and rapidly expanded. Exam reveals a 10 cm by 10 cm exophytic and indurated mass protruding from the right face, extending from the preauricular area and zygoma to his proximal neck with a necrotic and purulent central region. CT imaging shows a necrotic infiltrative malignant mass of the right cheek with extensive right neck neovascularity and adenopathy at all cervical levels.
Tumor neglect is a maladaptive response to grossly evident cancers that are disfiguring and life-threatening. The phenomenon, uncommon and largely unstudied, involves patients ignoring tumors in order to “cope with the obvious, outward and clearly visible signs of cancer.”1 Denial is a common coping mechanism that grants individuals time to come to terms with stressful situations. However, it has the potential to become pathological, particularly when one’s own health is at stake.
Little research is available on this phenomenon, with only a few isolated case studies. The incidence is unknown. Cancers that appear to be most commonly associated with tumor neglect include those that are visible to the patient, larger than 1 cm, and especially malignancies of the skin and breast, though cases of testicular and some solid organ cancers have been reported. It is estimated that a third of women with symptoms of breast cancer will delay seeking professional care by > 3 months.1 A 2018 report details a case of a 37-year-old woman with a growing breast lump for 4 months who presented to the ED with pain at the site.2 Imaging confirmed the 16 cm by 13 cm fungating mass had metastasized to the lung and liver. Shortly after admission, the patient developed spontaneous tumor lysis syndrome and died of multiorgan failure.
Several case studies describe individuals ignoring their tumors for months or even decades, resisting the efforts of family and friends to persuade them to seek medical care.2 Such neglect can lead to unchecked tumor growth, disfigurement, metastasis, and death.2 Management of such advanced cases depends on several factors and often requires a multidisciplinary team that may include surgeons for resection and reconstruction in particularly challenging cases.1
The reasons for this unusual phenomenon are multifactorial: distrust of the health care system, poor medical literacy, low socioeconomic status, psychosocial stressors, and the tendency to overlook the hazard of slow-growing tumors. A patient’s fear of a formal cancer diagnosis and its potential financial burden may also be contributing factors. Patients seek to maintain control and independence as their deteriorating health threatens the status quo.3 Those suffering from tumor neglect do not see their behavior as a form of denial and can feel suspicious of and threatened by the perceived interference of family and medical personnel who seek to help. Understandably, patients with tumor neglect can inadvertently become alienated by their behavior and the presence of a visible malignancy.
Emergency physicians are uniquely positioned to offer support, as potentially the first point of contact when a patient seeks help. Often, the most meaningful impact relates less to immediate management than referral to a specialist. Establish rapport, try to overcome the patient’s distrust of physicians, and eliminate barriers to health care when possible. Preserve the patient’s autonomy by seeking their input on key decisions in their care, while providing an informed perspective on their condition.
Case Resolution
Our patient was admitted with oncology and otolaryngology consults. Biopsies revealed HPV-negative, poorly differentiated squamous cell carcinoma of the face. A PET scan demonstrated significant metastases to the spine, liver, and lungs. Three weeks later, the patient underwent resection of the facial mass with modified radical neck dissection and pectoralis flap placement. Three months later, he was transitioned to hospice care and died under unclear circumstances.
Take-Home Points
- Cancers most commonly associated with tumor neglect include malignancies of the skin and breast.
- Tumor neglect is usually multifactorial in etiology, with a significant role for emotional distress, fear of death, financial difficulties, lack of health care literacy, and distrust of physicians.
- Respecting the patient’s autonomy and self-determination is paramount.
- EM physicians should identify and ensure immediate referral for high-risk populations or for concerning lesions.
References
- Block LM, Jee YM, Baskaya MK, Bentz ML, Poore SO. Denying the Obvious. Plast Reconstr Surg Glob Open. 2015;3(11):e571.
- Cordrey EO, Dienhart JA, Wang J. Spontaneous tumor lysis syndrome in a giant neglected breast cancer. J Molec Oncol Res. 2018;2(2).
- Day MR, Leahy-Warren P, Mccarthy G. Self-Neglect: Ethical Considerations. Ann Rev Nurs Res. 2016;34(1):89-107.