Case
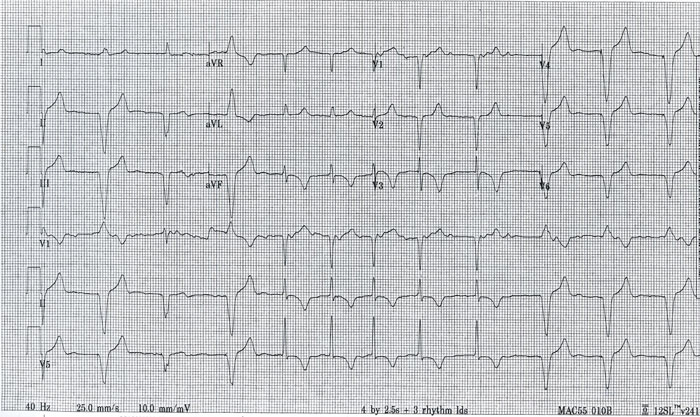
A 76-year-old female with dementia and unknown cardiac history presents with chest pain and palpitations for 4 hours.
Answer
Atrial fibrillation preceded and followed by paced beats.
Let’s take this piece by piece. First, there are 2 distinct rhythms and 3 distinct QRS morphologies. In the middle of this ECG you can clearly see atrial fibrillation in which there is no clear and regular p-wave and the beats follow an irregularly irregular pattern. As there are no other conduction abnormalities, the QRS complex in this segment is narrow. At the beginning and end of this ECG there are wide-complex QRS complexes preceded by very subtle pacer spikes. The rate is also slower at approximately 60 beats per minute (bpm). The most likely explanation is that there was a string of atrial fibrillation and the ventricular pacemaker kicked in once the rate slowed below 60 bpm. There is a third distinct wave-form morphology seen in this ECG which is the third beat in this ECG. In this beat, which is a fusion beat, depolarization in the ventricle is initiated from both the pacemaker and the AV node. Another important aspect of this ECG is the diffuse inverted T waves seen in the non-paced beats. This could be secondary to ischemic changes (suspicion should be based on the clinical scenario) or due to T-wave memory. T-wave memory is a phenomenon in which permanent T-wave changes resulting from long-term ventricular pacemaker use can be seen in non-paced beats.
Learning Points
- Be suspicious of atrial fibrillation in any ECG without clear p-waves and beats that occur at irregularly irregular intervals.
- T-wave changes in a patient with a longstanding pacemaker may result in permanent T-wave changes in non-paced beats.



