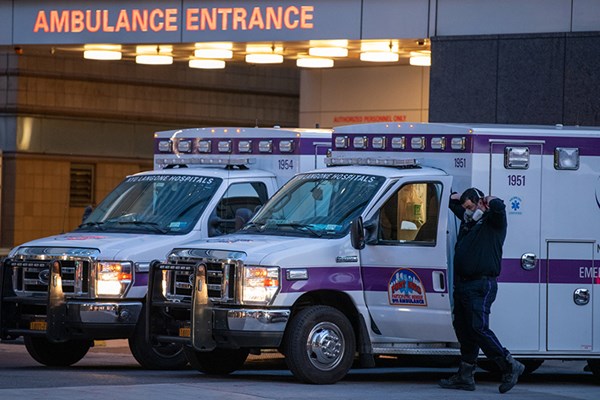
Prehospital personnel are truly on the frontlines of medicine, and they have been dramatically affected by the SARS-CoV-2 pandemic. As protocols shift according to supplies and emerging research, how are we protecting our EMS first responders from COVID-19?
Facing uncertainty at every scene, Emergency Medical Services (EMS) teams must maintain rapid responses, ensure adequate personal protective equipment (PPE), and adhere to frequent changes to protocols.
Services across the country have been dealing with the problem of limited supplies of PPE and many have found creative measures to protect patients and providers. Prior to COVID-19, EMS providers would lace up their tactical boots, slip-on their gloves, and be ready to face most scenes to which they were called. Now, like other healthcare workers, EMS crews have to reuse PPE for multiple patients with the worry of cross-contamination. With the virus’s continued spread, each service has implemented various changes to try to deal with these challenges.
PPE protocols across the country have seen drastic changes since the start of the pandemic. Initially, providers were generally wearing only a surgical or N95 mask to calls that were suspicious for COVID-19 infections. As we have learned more about the viral spread, regulations have evolved to protect the men and women on the frontlines.
Many services are now applying risk stratification based on dispatch information and patient complaints and symptoms. For example, Stonewall Jackson, a service in the suburbs of Washington, DC, stratifies patients by low, moderate, high, and severe acuities.
| LOW ACUITY PATIENTS (not suspected to have had contact with the virus and have no respiratory complaints) |
EMS providers are required to wear gloves alone with these patients |
| MODERATE ACUITY PATIENTS | EMS providers are required gloves, face masks, and goggles and patients wear a mask |
| HIGH ACUITY PATIENTS (possible COVID-19 exposures/symptoms) |
EMS providers wear a gown, mask, goggles, and gloves |
|
SEVERE ACUITY PATIENTS |
EMS providers wear an isolation suit, gloves, P100 respirator, goggles, and a face shield are expected to be worn in these cases |
In Saline County, Missouri, paramedic Scott Raak reports that all providers are to wear gloves, surgical masks, and eye protection for every patient. If a possible or confirmed COVID-19 patient calls, providers are to wear what the service calls the Scott Pro2000. This consists of a full mask air purifier, a rubber body suit, and boots. In Columbus, Ohio, Eric Cortez, MD, and Robert Lowe, MD, medical directors of several Columbus Township agencies and the Columbus Fire Department, respectively, have changed their protocols to require surgical masks on all calls. The Columbus Fire Department has their providers wear yellow turnout jackets to calls as well. When responding to nursing homes, adult care centers, shelters, and extended care facilities, they are requesting the facilities bring patients as close to the entrances as possible to decrease contamination.
Mount Sinai's health system in New York City is avoiding aerosol treatments, like nebulizers, and requiring providers to wear N95 masks on all calls. Seattle and King County, Washington, are doing what they call MEGG (mask, eye protection, gloves, and goggles). Providers there are required to wear a cloth or surgical mask throughout the entire shift and are placing surgical masks on all patients.
Many more services across the country are also following similar protocols and implementing other vital safety procedures. When performing aerosol-generating procedures, Rosie Roantree, DO, EMS medical director of Town of Wallkill Volunteer Ambulance Corps, an ALS agency in Middletown, New York, recommends keeping ambulance doors open and turning on the heating, ventilation, and air conditioning (HVAC) system. In Rochester, Minnesota, EMS medical director Anuradha Luke, MD, FACEP, of the Mayo Clinic, states that their department has EMS physician phone coverage and is starting to make 24/7 telemedicine available for its prehospital providers. This may allow EMS crews to make treatment decisions in the field and therefore reduce the number of patient transports, potentially helping to decrease the spread of the virus.
Departments have become increasingly innovative during this time of great need. Harrison Brookeman, a second-year medical student at the Virginia Tech Carilion School of Medicine and a leader on his COVID-19 team at the Charlottesville Albemarle Rescue Squad, reported that teams have been receiving 3D-printed and laser-cut face shields from the University of Virginia. They are working with the Department of Engineering to design printable face masks for the service.
Paramedic Taylor Mathis of Waynesboro First Aid Crew in Waynesboro, Virginia, shared that his service has a dedicated COVID-19 ambulance. The ambulance is plastic-wrapped and there are no porous surfaces in the back of the ambulance, greatly reducing the chance of contamination. All monitor equipment is separated into plastic bags that can be wiped clean after use. All other equipment such as medications, O2 tanks, and PPE, is located outside of the patient care area. EMRA Prehospital & Disaster Medicine Committee Chair-Elect Sarayna McGuire, MD, of the Mayo Clinic, reported that local EMS have started reprocessing masks using vaporized hydrogen peroxide.
The University of Missouri’s Adam Beckett, DO, made boxes out of plastic and PVC pipe to place over patients. The “Beckett Box” is used as a protective barrier during intubations and aerosolizing procedures. The boxes have openings large enough for the provider to be able to bag the patient or change medications. In Lansing, Michigan, providers have been using a $10 translucent umbrella as a shield during intubations. They cut the umbrella in half and slide the stem under the mattress. With holes on either side, this is an affordable way to incorporate a protective barrier into intubations.
Joshua Schwanke, EMT-B, of Pottawatomie County, Kansas, states that his agency has issued its EMS providers a "PPE kit" containing three N95 masks that are to be reused unless grossly contaminated or used on a COVID-19 patient under investigation (PUI), two gowns, one Tyvek suit, and two pairs of boots covers.
Unfortunately, even with all these innovations, the future availability of life-protecting supplies is still a concern. For many EMS agencies, the outlook on PPE supplies is grim. For example, in Topeka, Kansas, providers receive one surgical mask for their entire shift and one N95 mask to be used for as long as possible. Agencies in New York are low on gowns and have been forced to use the same gown for multiple patients throughout the day.
Betty Yang, MD, an EMS fellow at the University of Washington, and her colleagues found some hope in the midst of the pandemic. In a study of the Seattle Fire Department which is currently awaiting publication, they found a transmission rate of less than one percent for all EMS providers who took care of patients with COVID-19, both with adequate and inadequate PPE usage. This indicates that while more PPE is better, even minimal PPE provides protection.
Protecting our frontline providers will only be possible if the supply of PPE is maintained. The ingenuity of many prehospital systems during the pandemic has been inspirational. Medicine requires critical thinking and these skills have been utilized to tackle the PPE shortage across the country. The EMS community has come together to find ways to protect themselves and still provide high-quality patient care during this crisis.
Acknowledgements
Special thanks to Adam Beckett, DO, Eric Cortez, MD, Robert Lowe, MD, Anuradha Luke, MD, FACEP, Sarayna McGuire, MD, Kevin Mujal, MD, Rosie Roantree, DO, Joshua Stilley, MD, Betty Yang, MD, Harrison Brookeman, Bryce Taylor, Taylor Mathis, NRP, Scott Raak, NRP, Joshua Schwanke, EMT-B, Amanda Parker, Mary Grace Swanson, and to all those who have contributed.