A 77-year-old male with a history of atrial fibrillation (not on anticoagulation), heart failure with reduced ejection fraction, hyperlipidemia, hypertension, gout, and prostate cancer (status post transurethral resection of the prostate in 2014) presents to the emergency department with right-sided flank pain for 2 days.
The pain radiates to his back and right lower abdomen and is described as constantly aching, dull, and 8/10 in severity. He has been taking 800mg of naproxen every 6 hours with only mild relief. Earlier in the day, he had one episode of emesis.
In the ED, the patient is afebrile, blood pressure 192/90 mmHg, 100/min and irregular, and respiratory rate 18/min and non-labored. Pulse oximetry is 100% on room air. Labs are notable for a creatinine of 1.53 with eGFR 50. Although he denies hematuria or dysuria, urinalysis shows moderate blood.
The initial differential includes urolithiasis, pyelonephritis, and renal artery or vein thrombosis. Since the patient is not on anticoagulation for his atrial fibrillation, suspicion for infarction is high, and a CT abdomen and pelvis with IV contrast is ordered. The CT shows a subtotal infarct of the right kidney secondary to a proximal right renal artery thrombus (Image 1). Vascular surgery does not recommend any surgical intervention, and a heparin drip is started.
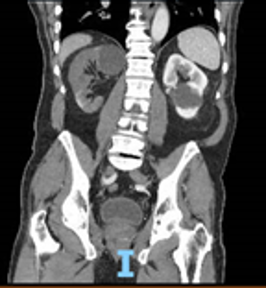
Image 1: CT abdomen pelvis with IV contrast showing subtotal infarction of the right kidney due to a proximal right renal artery thrombus.
Discussion
There are two kinds of hematuria: (1) macroscopic hematuria, which is gross blood in the urine, and (2) microscopic hematuria, which is blood in the urine visualized only under the microscope.1
Macroscopic hematuria can be caused by as little as 1mL of blood in 1 liter of urine and can be due to arterial or venous blood, though myoglobinuria from rhabdomyolysis and hemoglobinuria from hemolysis can also turn urine a red color.
The definition of microscopic hematuria can vary but is generally thought of as 3 or more red blood cells per high-powered field.1-4 A false negative result on urine dipstick for hematuria can occur from low urine pH, high urine specific gravity, or high dietary vitamin C.1,2 Certain medicines and foods, including rifampin and beets, can cause urine to appear red grossly but will be negative for hematuria on dipstick or urinalysis.2 Though the true causes of hematuria can be extensive, this review will focus on the most common and emergent causes.
When working up a patient with hematuria, the clinician must consider the larger context in which the patient is presenting. For a patient with colicky flank pain, costovertebral angle tenderness, and hematuria, a non-contrast CT abdomen and pelvis is an excellent first imaging modality choice, but what does the clinician do when that CT comes back negative for renal stones? Additionally, what about the patient presenting with atypical flank pain? Gross hematuria without any flank pain? These patients may warrant broadening the differential and further investigation with additional imaging in the ED.
Urolithiasis
A common cause of hematuria is urolithiasis, although 10-20% of patients with urolithiasis will present without hematuria. Microscopic hematuria on urinalysis has a 69-84% sensitivity for urolithiasis. One study by Mefford et al found that more severe obstructive uropathy correlated with a lower incidence of hematuria, although the reasons for this are unclear.5 Non-contrast CTs are currently the best imaging modality for diagnosing kidney stones, with a sensitivity of 97–100% and specificity of 94–96%. Stones larger than 5mm are more likely to cause severe hydronephrosis and obstruction and are more likely to require urology consultation.5
Urinary Tract Infection
Urinary tract infections cause up to 20% of microscopic hematuria cases and less commonly may also present with macroscopic hematuria.3 On urinalysis, positive nitrites, leukocyte esterase, WBCs, and bacteria may all be indicative of a urinary tract infection.2-4 Left untreated, a urinary tract infection could turn into pyelonephritis. However, in the setting of a patient with fever and colicky flank pain, an infected obstructive kidney stone must be considered.5 If the hematuria does not resolve after the infection has been appropriately treated, further investigation into alternative causes of hematuria should be initiated.3
Malignancy
Asymptomatic hematuria ranges from 2-31% in the general population and does not necessarily portend pathology.1,3However, 20-40% of patients with macroscopic hematuria have an underlying urological malignancy, usually bladder cancer. Up to 90% of patients with urologic malignancy initially will present with hematuria. Even a single episode of macroscopic hematuria — even in patients on anticoagulation — should prompt further testing for malignancy.2,6
Renal Artery Thrombosis
Renal infarction presents similarly to renal stones; this can lead to delayed diagnosis.7 The patient will have flank or abdominal pain, nausea, and vomiting, with labs showing leukocytosis and elevated lactate dehydrogenase.7 Renal infarction is more commonly caused by renal artery thrombosis, either by chronically forming cholesterol-based clots in patients with hyperlipidemia or acute dislodgement of a blood clot from the left atrium in patients with atrial fibrillation. Endocarditis, trauma, and other pathology may also precipitate an embolic event.7,8,9 As patients present with similar symptoms as those with urolithiasis (i.e., flank pain and hematuria), the clinician must have a high index of suspicion for this often-missed diagnosis.
The imaging modality of choice is a CT angiogram of the abdomen, which has 100% specificity for renal artery thrombosis.7,8 A CT with or without contrast may still diagnose the infarction, but it is much less specific. Sending these patients home without the correct diagnosis can be life-threatening. These patients need to be admitted, as the decreased perfusion to the kidney causes kidney injury and potentially irreversible kidney failure if not treated with heparin or local thrombolysis from interventional radiology.8,9
Patients on anticoagulation therapy may still present with renal infarction, either due to failure of anticoagulation therapy or medicine non-adherence. However, anticoagulation medications can also cause gross hematuria from conditions that, without anticoagulation medications, may not have caused as much or any hematuria. In addition, studies have shown an association of higher complications of hematuria (including hospitalizations and urologic procedures for hemorrhage control) for patients on antithrombotic medication.10
Ruptured Abdominal Aortic Aneurysm
As abdominal aortic aneurysms (AAAs) are often asymptomatic, a patient’s first presentation for AAA will often be for AAA rupture, a dangerous complication that has up to a 75% mortality.11,12 Aneurysms considered at risk for rupture and requiring preemptive surgical intervention include those over 5.5 cm in size or those increasing 0.5 cm or more in size over 6 months.11,12
The textbook presentation of ruptured AAA is a pulsatile abdominal mass with a bruit and high output cardiac failure. Several studies have shown, however, that while these findings are only present in some patients (around 50%), hematuria will be present in upwards of 87% of patients.13,14 As this is an unusual cause of hematuria, it may delay the diagnosis, though further data is needed to investigate the impacts of hematuria as the chief complaint on ruptured AAA mortality.13 The diagnosis can be confirmed by ultrasound or CT angiography, and definitive management is by open or endovascular repair.11,12
Tuberculosis
Classically, tuberculosis will present with pulmonary symptoms, night sweats, and weight loss, but when tuberculosis invades extra-pulmonary systems, its presentation can be strange and unexpected. There have been multiple case reports of genitourinary tuberculosis presenting as hematuria with or without dysuria.15,16 Diagnosis may be elusive, as less than 5% of these patients have active pulmonary tuberculosis.15,16 It is often only recognized in the late and chronic stage, by which time it may have caused renal parenchymal destruction, ureteral strictures, or end-stage renal disease.15,16 Though biopsy may be necessary, urine culture and PCR testing are key to diagnosis, and treatment is similar to that for pulmonary tuberculosis.15,16
Nephropathy
From familial diseases such as Alport syndrome to the acquired diseases of post-streptococcal glomerulonephritis or IgA nephropathy, there are multiple other causes of hematuria to consider.2,6 These are less common and usually present within the setting of other signs and symptoms to clue the physician in. If the patient is stable and otherwise doing well, outpatient nephrology follow-up may be appropriate after the initial ED workup.
Conclusion
Hematuria in the setting of flank pain is a common presentation to the ED. As kidney stones affect up to 15% of the population, it is often standard to order a non-contrast CT abdomen and pelvis in these patients to search for a stone.5However, in the setting of a negative non-contrast CT scan and especially in patients with risk factors for renal infarction, the next step should be a CT angiogram to rule out renal vein or artery thrombosis. Other unusual causes of hematuria to keep in mind are ruptured abdominal aortic aneurysm and tuberculosis, as these can be life-threatening if not recognized.
References
- Bolenz C, Schröppel B, Eisenhardt A, Schmitz-Dräger BJ, Grimm MO. The Investigation of Hematuria. Dtsch Arztebl Int. 2018;115(48):801-807.
- Goller T, Klemencic S, Sheng A, Koyfman A, Long B. Evaluation and Management of Hematuria in the Emergency Department. emDOCS.net. 2021 March.
- Sharp VJ, Barnes KT, Erickson BA. Assessment of asymptomatic microscopic hematuria in adults. Am Fam Physician. 2013;88(11):747-754.
- Saleem MO, Hamawy K. Hematuria. [Updated 2021 Aug 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan.
- Mefford JM, Tungate RM, Amini L, et al. A Comparison of Urolithiasis in the Presence and Absence of Microscopic Hematuria in the Emergency Department. West J Emerg Med. 2017;18(4):775-779.
- Hicks D, Li CY. Management of macroscopic haematuria in the emergency department. Emerg Med J. 2007;24(6):385-390.
- Antopolsky M, Simanovsky N, Stalnikowicz R, Salameh S, Hiller N. Renal infarction in the ED: 10-year experience and review of the literature. Am J Emerg Med. 2012;30(7):1055-1060.
- Lopez VM, Glauser J. A case of renal artery thrombosis with renal infarction. J Emerg Trauma Shock. 2010;3(3):302.
- Sauerberg N, Khan YS. Renal Artery Thrombosis. [Updated 2021 Oct 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan.
- Wallis CJD, Juvet T, Lee Y, et al. Association Between Use of Antithrombotic Medication and Hematuria-Related Complications. JAMA. 2017;318(13):1260-1271.
- Jeanmonod D, Yelamanchili VS, Jeanmonod R. Abdominal Aortic Aneurysm Rupture. [Updated 2021 Aug 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan.
- Aggarwal S, Qamar A, Sharma V, Sharma A. Abdominal aortic aneurysm: A comprehensive review. Exp Clin Cardiol. 2011;16(1):11-15.
- Pomper SR, Fiorillo MA, Anderson CW, Kopatsis A. Hematuria associated with ruptured abdominal aortic aneurysms. Int Surg. 1995;80(3):261-263.
- Salo JA, Verkkala KA, Ala-Kulju KV, Heikkinen LO, Luosto RV. Hematuria is an indication of rupture of an abdominal aortic aneurysm into the vena cava. J Vasc Surg. 1990;12(1):41-44.
- Bae EH, Heo S, Kim YH, et al. Gross hematuria associated with genitourinary tuberculosis. Chonnam Med J. 2013;49(1):48-49.
- Muneer A, Macrae B, Krishnamoorthy S, et al. Urogenital tuberculosis — epidemiology, pathogenesis and clinical features. Nat Rev Urol. 2019;16:573–598.



