Appendicitis is the most common pediatric abdominal surgical emergency, with a lifetime risk of 7 percent.
Ultrasound is the primary imaging modality in children to avoid the harmful effects of radiation.1 The estimated lifetime risk of developing cancer after one abdominal computed tomography (CT) scan in a 1-year-old child is increased by 0.18 percent.2
Driven by pediatric emergency medicine physicians, recent trends in CT utilization in children have been reduced over the past 10 years, but use of the technique in children remains common. It was found that non-pediatric hospitals used CT for appendicitis in >70 percent of cases, compared with 25 percent of cases at children’s hospitals.3 However, most pediatric appendicitis cases will present to non-pediatric hospitals.4 It was estimated that 57 percent of graduating EM residents will go on to practice community medicine, and thus require training to assist their patients outside of pediatric hospitals.5
Appendix point-of-care ultrasound (POCUS) has a sensitivity of 92 percent when evaluating for secondary signs of appendicitis (appendicolith, peri-appendiceal free fluid).6 Imaging and management modalities can shift drastically based on the time of day (radiology ultrasound availability), practice location (freestanding or critical access ED, community vs. academic/pediatric hospital), EM faculty experience with POCUS, as well as surgeon preference. EM ultrasound education is continuously evolving with academic leaders re-examining what constitutes core content for POCUS.7
Our purpose is to increase the momentum behind adding appendiceal ultrasound to core EM training competencies.
Explanation
We surmise that with more focused pediatric abdominal ultrasound training in residency, a foundation of comfort and knowledge would eventually lead to a trickle-down effect to future generations of EM learners.
A second-year EM resident interested in pediatric emergency medicine POCUS spent a one-month advanced ultrasound elective focused on pediatric ultrasound. This elective included dedicated didactics focusing on pediatric sonography, simulation, and hands-on experience. The resident was required to submit >25 percent of the 150 scans required for the rotation on pediatric patients for quality assurance. Additionally, weekly POCUS rounds in the pediatric intensive care unit provided an opportunity for increased comfort and familiarity with scanning the pediatric patient and also supplanted times when ED pediatric volumes provided less opportunity.
Description
In 2012, the Council of Emergency Medicine Residency Directors (CORD) and the American Institute of Ultrasound in Medicine (AIUM) recognized appendix ultrasound as an advanced POCUS application.8 This resident learner felt increasing confidence and familiarity not only with pediatric appendicitis but with a general approach to scanning children. She endorsed that patients’ families were overall pleased to have these educational scans performed on their children. This resident was encouraged by the added value she brought to her patients and training program with this innovation.
As she progressed to a third-year resident, she had many cases of accurately diagnosed appendicitis by POCUS. This is an example of a perforated appendicitis diagnosed by this resident (Figure 1). The patient was a previously healthy 9-year-old male presenting to the ED with a chief complaint of sharp non-radiating right lower quadrant abdominal pain for three days. His mother endorsed multiple episodes of emesis. Physical exam showed a febrile male with right lower quadrant abdominal tenderness with accompanying rebound tenderness. Laboratory results revealed a leukocytosis of 24,000. The patient was seen by general surgery and taken directly to the operating room based on the resident’s POCUS scan.
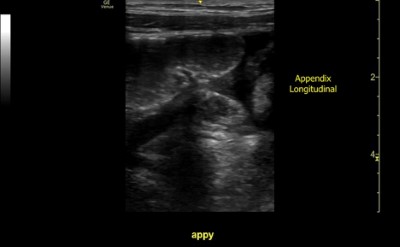
Figure 1. This is an example of a perforated appendicitis diagnosed by this resident. The patient was a previously healthy 9-year-old male presenting to the ED with a chief complaint of sharp non-radiating right lower quadrant abdominal pain for three days. His mother endorsed multiple episodes of emesis. Physical exam showed a febrile male with right lower quadrant abdominal tenderness with accompanying rebound tenderness. Laboratory results revealed a leukocytosis of 24,000. This patient was seen by general surgery and taken directly to the operating room based on the resident’s POCUS scan.
By using the aforementioned educational model, resident learners were able to accurately diagnose appendicitis by POCUS prior to obtaining comprehensive ultrasound, thereby expediting patient care.9–11 Ideally, training would reflect a balance of both pathologic and non-pathologic scans, as well as a required percentage of all educational ultrasounds to be performed on pediatric patients. In times of reduced pediatric volumes or in adult only EDs, rounding in a pediatric unit may present more opportunity for exposure.
If pediatric abdominal ultrasound is routinely and deliberately taught to EM residents, a cultural shift away from obtaining abdominal CTs in children would be the desired outcome.
Disclaimer: This research was supported (in whole or in part) by HCA Healthcare and/or an HCA Healthcare affiliated entity. The views expressed in this publication represent those of the author(s) and do not necessarily represent the official views of HCA Healthcare or any of its affiliated entities.
References
- Petroianu A. Diagnosis of acute appendicitis. Int J Surg. 2012;10(3):115-119.
- Brenner D, Elliston C, Hall E, Berdon W. Estimated risks of radiation-induced fatal cancer from pediatric CT. AJR Am J Roentgenol. 2001;176(2):289-296.
- Anderson KT, Bartz-Kurycki MA, Austin MT, et al. Hospital type predicts computed tomography use for pediatric appendicitis. J Pediatr Surg. 2019;54(4):723-727.
- Hodges MM, Burlew CC, Acker SN, et al. Pediatric appendicitis: Is referral to a regional pediatric center necessary? J Trauma Acute Care Surg. 2018;84(4):636-641.
- Burkhardt J, Kowalenko T, Meurer W. Academic career selection in American emergency medicine residents. Acad Emerg Med. 2011;18(10 Suppl. 2):48-53.
- Khan U, Kitar M, Krichen I, et al. To determine validity of ultrasound in predicting acute appendicitis among children keeping histopathology as gold standard. Ann Med Surg. 2019;38:22-27.
- American College of Emergency Physicians. Ultrasound Guidelines: Emergency, Point-of-care, and Clinical Ultrasound Guidelines in Medicine. ACEP Policy Statement. 2016.
- Lewiss RE, Pearl M, Nomura JT, et al. CORD-AEUS: Consensus document for the emergency ultrasound milestone project. Acad Emerg Med. 2013;20(7):740-745.
- Dadeh A-A, Phunyanantakorn P. Factors Affecting Length of Stay in the Emergency Department in Patients Who Presented with Abdominal Pain. Emerg Med Int. 2020;2020:5406516.
- Seyedhosseini J, Fadavi A, Vahidi E, Saeedi M, Momeni M. Impact of point-of-care ultrasound on disposition time of patients presenting with lower extremity deep vein thrombosis, done by emergency physicians. Turkish J Emerg Med. 2018;18(1):20-24.
- Zare MA, Bahmani A, Fathi M, Arefi M, Hossein Sarbazi A, Teimoori M. Role of point-of-care ultrasound study in early disposition of patients with undifferentiated acute dyspnea in emergency department: a multi-center prospective study. J Ultrasound. Published online May 29, 2021.
- Nah SA, Ong SS, Lim WX, Amuddhu SK, Tang PH, Low Y. Clinical Relevance of the Nonvisualized Appendix on Ultrasonography of the Abdomen in Children. J Pediatr. 2017;182:164-169.e1.