Septic arthritis is a rheumatologic emergency.
Annually, there are 20,000 cases of septic arthritis in the United States.3 In some cases the diagnosis can be confounded by multiple factors in the patient's history.
Case
A 40-year-old male with no significant past medical history presented to the ED complaining of erythema, pain, and edema of the left wrist for 2 weeks along with pain and edema of the right knee for 1 week. The patient stated he had been weeding on a recently purchased outdoor property in rural Pennsylvania. The patient's fiancée noticed a small, target-like lesion on his back a few weeks prior and thought it was a fungal infection. The patient began using an antifungal cream, which seemed to have resolved the rash. Upon further questioning, the patient stated he was having pain and swelling in multiple joints over the past 5 months but decided to come to the ED now because of worsening symptoms, particularly in his right knee. The patient reported a family history of rheumatoid arthritis in his father. He endorsed chills but denied fevers, vision changes, shortness of breath, chest pain, abdominal pain, vomiting, diarrhea, penile discharge, pain with urination, or genital lesions He did not have a history of gout, skin lacerations, trauma to any of the joints, or intravenous drug use. Both the patient and his fiancée confirmed a monogamous relationship and at present were not concerned for any sexually transmitted infections (STIs); however, the patient did report a remote history of chlamydia. He was questioned about his sexual history without his fiancée in the room, and he again reported only having sexual relations with his fiancée.
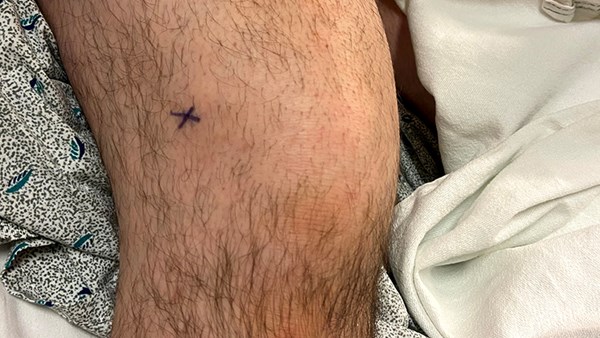
Upon arrival, the patient was found to be febrile 100.5°F and tachycardic 105 BPM. Otherwise, the patient was hemodynamically stable but in obvious distress secondary to pain. On physical examination, the left wrist was mildly erythematous and edematous without tenderness to palpation or pain with passive or active range of motion. The right knee was grossly edematous with mild erythema and severe pain during active and passive range of motion.
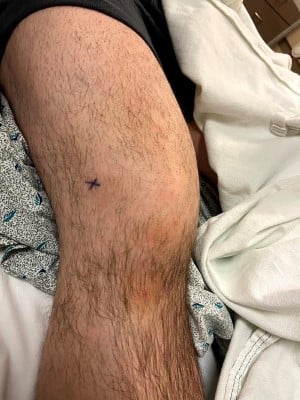
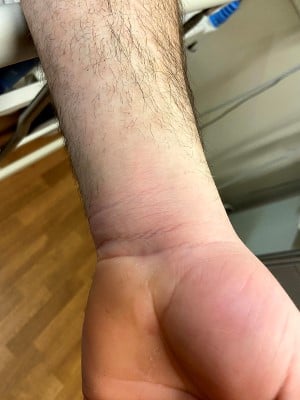
X-ray of the left wrist was negative for fracture or effusion. X-ray of the right knee was significant for a large suprapatellar effusion but no fracture. Chest X-ray was unremarkable. CBC was significant for a white blood cell count of 14.6. The BMP was unremarkable, and lactate was 1.3. Inflammatory markers included CRP 19 and ESR >100. Uric acid was 2.6.
A knee arthrocentesis was performed which revealed a cloudy yellow aspirate with WBC 95,300, RBC 110,000, segmented neutrophils 88%, lymphocytes 4%, monocytes 8%, and no crystals.
The ED team consulted orthopedic surgery, who was not entirely convinced the patient’s symptoms were consistent with septic arthritis based on involvement of multiple joints and 5-month duration of symptoms. However, they agreed the patient needed IV antibiotics and surgical intervention. The patient was admitted for presumed septic arthritis, and orthopedic surgery completed a washout of the right knee the following morning.
Discussion
Septic arthritis is a rheumatologic emergency, which may lead to permanent joint damage and a mortality rate of 10-15%.1,2 Annually, there are 20,000 cases of septic arthritis in the United States.3 Gonococcus was the leading cause of septic arthritis in young adults in the past, but it now makes up less than 1% of septic arthritis cases.4 Joint infection can occur via direct inoculation, hematogenous spread, or spread from contiguous infection. Large joints are more often affected, and the most common joint involved is the knee.5 If left untreated, non-gonococcal septic arthritis can destroy articular cartilage, causing permanent joint damage.1
The essentials for diagnosis of septic arthritis include fever, painful joint, joint effusion, and arthrocentesis findings.6 The pain is acute or subacute with associated erythema, swelling, and limitation of motion in the affected joint. Definitive diagnosis is established by identification of an organism in the synovial fluid. Blood cultures often can be positive even when joint cultures are negative. The joint fluid analysis typically demonstrates high leukocyte counts, usually over 50,000, but you should maintain clinical suspicion for inflammatory or infectious process when the count is above 7500. The higher the white cell count in the joint fluid the more likely for it to be of bacterial or fungal origin. Smear and cultures should be obtained from the synovial fluid sample to determine the causative organism.
In gonococcal arthritis, Gram stain smears and bacterial cultures are negative in 50-75% of cases. Treatment for disseminated gonococcal infection (DGI) is ceftriaxone 1 g IV every 24 hours plus azithromycin 1 g orally as a single one-time dose (preferred initial regimen). Alternative regimens include IV cefotaxime or ceftazidime 1 g every 8 hrs with a one-time dose (2 g) of azithromycin.
This case had a multitude of confounding factors that could have explained the patient's migratory polyarthralgias. The patient had a recent history of weeding in Pennsylvania, a family history of rheumatoid arthritis, and a remote history of chlamydia. In the ED, while it may not be pertinent to determine the causative organism in an inflamed joint, it is important to have a high index of suspicion for septic arthritis in order to complete the proper tests and procedures, consult orthopedics early, and admit for IV antibiotics and further treatment.
Septic arthritis should be considered in all individuals with non-traumatic joint pain. It may be difficult to diagnose DGI during the initial ED evaluation because many patients will not report high-risk behaviors such as multiple partners, men having sex with men, or history of prior STI. Individuals with suspected DGI should undergo testing for other STIs such as HIV, chlamydia trachomatis, and syphilis.
Case Conclusion
Upon admission, the patient had an extensive workup to determine the etiology of his migratory polyarthralgia. His Lyme titer was negative. Cyclic citrullinated peptide AB <16 (normal). Rheumatoid factor screen negative. HLA-B27 Negative. RPR reactive. FTA-ABS reactive. HIV non-reactive. The key lab result was the culture of the right knee aspirate which grew Neisseria gonorrhoeae. Finally, the patient’s echocardiogram was negative for endocarditis. Unfortunately, despite clinical improvement after being started on appropriate antibiotic coverage, the patient signed out Against Medical Advice on day 4 of his hospital stay.
Take-Home Points
- When assessing a painful swollen joint, it is important to:
- Obtain a thorough history
- Review vitals for signs of sepsis
- Complete a comprehensive physical exam
- Establish a broad differential diagnosis
- Perform an arthrocentesis when applicable
- Consult orthopedic surgery early and admit the patient for IV antibiotics
- It is imperative to establish a non-judgmental environment and open rapport with the patient as it may be difficult to obtain the information required when questioning about STIs.
References
- Kaandorp CJ, Krijnen P, Moens HJ, Habbema JD, van Schaardenburg D. The outcome of bacterial arthritis: a prospective community-based study. Arthritis and rheumatism. 1997;40(5):884-892.
- Weston VC, Jones AC, Bradbury N, Fawthrop F, Doherty M. Clinical features and outcome of septic arthritis in a single UK Health District 1982-1991. Annals of the rheumatic diseases. 1999;58(4):214-219.
- Goldenberg DL, Cohen AS. Acute infectious arthritis. A review of patients with nongonococcal joint infections (with emphasis on therapy and prognosis). The American journal of medicine. 1976;60(3):369-377.
- Ross JJ. Septic Arthritis of Native Joints. Infectious disease clinics of North America. 2017;31(2):203-218.
- Kaandorp CJ, Dinant HJ, van de Laar MA, Moens HJ, Prins AP, Dijkmans BA. Incidence and sources of native and prosthetic joint infection: a community based prospective survey. Annals of the rheumatic diseases. 1997;56(8):470-475.
- Belcher C, Dawson M. Infectious Disease Emergencies. In: Stone CK, Humphries RL, eds. CURRENT Diagnosis & Treatment: Emergency Medicine, 8e. New York, NY: McGraw-Hill Education; 2017.