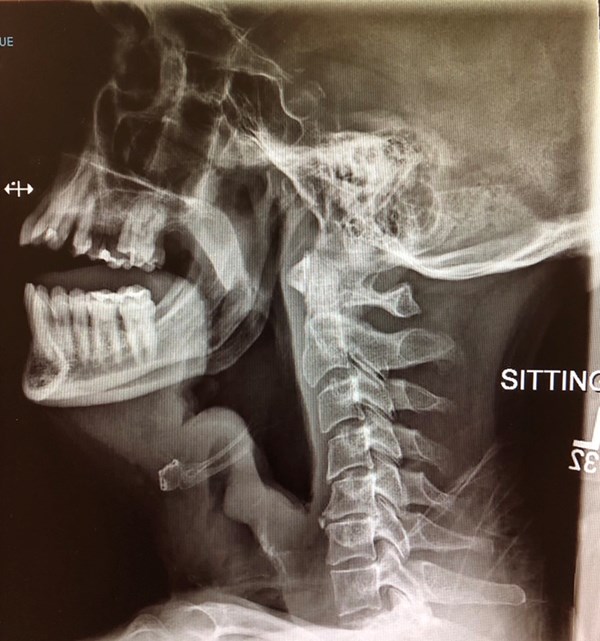
A male in his mid-40s presents with sore throat, difficulty breathing, vocal change, and drooling. He appears anxious and uncomfortable; initial vitals show a febrile, tachycardic patient.
Upon exam he is reluctant to rotate his neck, has difficulty speaking and swallowing, and repeatedly needs to wipe away excess drool. Visual inspection shows a normal-appearing pharynx; pulmonary exam reveals bilateral rhonchi. He reports receiving all regular vaccinations, has no history of severe allergic reactions or angioedema, and has no inciting event. His past medical history reveals nothing significant for difficulty breathing or airway pathology. He does not take any ACE inhibitors or other medications that can cause airway swelling.
What's your diagnosis?
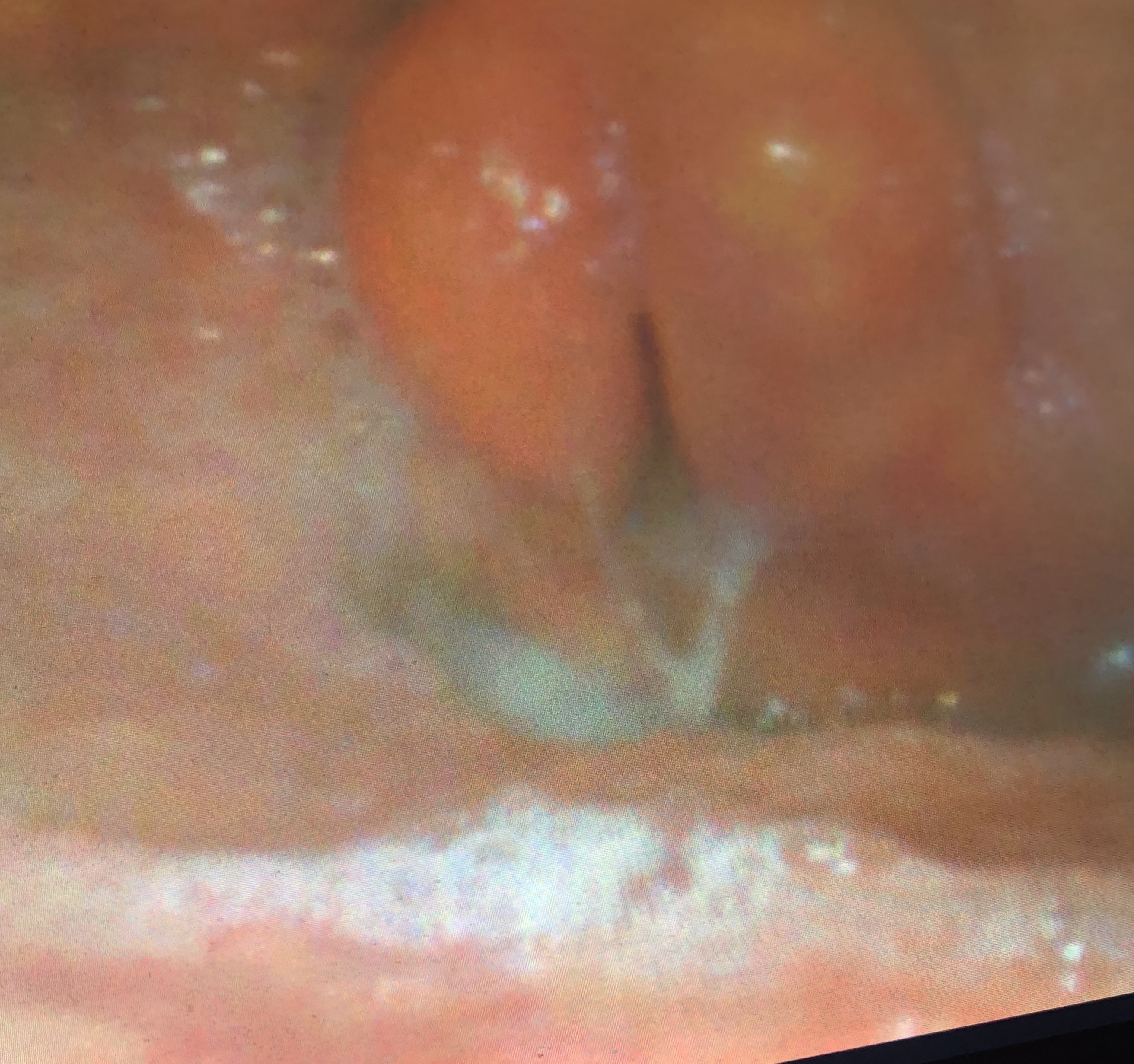
Epiglottitis
Airway edema is always concerning, and epiglottitis was near the top of the differential in this case within seconds of observing the patient. IV steroids, fluids, glycopyrrolate, racemic epinephrine, antibiotics, and radiographs of the chest and neck were all quickly ordered while paging ENT and anesthesia.
Upon visualizing the area around the vallecula with a nasopharyngeal scope, the epiglottis was found to be significantly inflamed and edematous, with no larynx visualized. During exhalation, there was a very thin, black slit being the only space for air to flow. During inhalation, this black slit disappeared.
With the confirmation of epiglottitis, the patient was taken emergently to the OR for an awake fiberoptic nasotracheal intubation. He was discharged days later and achieved full recovery.
Discussion
Epiglottitis is a relatively rare but potentially life-threatening condition associated with infection or injury. It constitutes a true medical emergency and should remain high on your differential when patients present with the hallmark symptoms of difficulty breathing/swallowing/speaking, excessive drooling, sore throat, fever, and slight relief when leaning forward.