Spontaneous iliopsoas injury, most commonly associated with athletes, is a rare cause of atraumatic hip pain - yet it should remain on your differential when evaluating hip or low back pain among the elderly, especially when the patient is unable to ambulate.
Spontaneous iliopsoas muscle or tendon injury is a rare cause of atraumatic hip pain. Given its mechanism, injuries tend to be found in athletes who suffer trauma during flexion activities. Nonetheless, spontaneous rupture with subsequent hematoma formation should be on the differential for acute, atraumatic hip or low back pain in the elderly, especially when the patient is unable to ambulate.
Case Report
A 91-year-old Caucasian female presented to the ED for right hip pain that started 7 hours prior to arrival. She stated she was attempting to put her right foot up onto a footstool when she felt a sudden pain in her right groin and hip. She had been previously able to walk on her own but has not been able to ambulate since the pain started. She had a catheter in place for chronic urinary retention, but denied any paresthesias in her groin, changes in her bowels, or pain radiating into her legs. She denied any recent traumas or falls. She described the pain as sharp, non-radiating, worse with attempting ambulation, and better at rest. She did not take anything at home for this pain. Her past medical history was significant for osteoarthritis, hypertension, hyperlipidemia, vocal cord dysfunction, and GERD.
Physical exam revealed a well-appearing elderly female in no acute distress. Her abdomen was soft. She had 5/5 strength with dorsiflexion and plantarflexion in the lower extremities bilaterally. Hip flexion was 2/5 in the right lower extremity and 5/5 in the left lower extremity. Sensation was intact throughout. Patellar reflexes 2/4 bilaterally. When the patient attempted ambulation, she was unable to bear weight on the right leg.
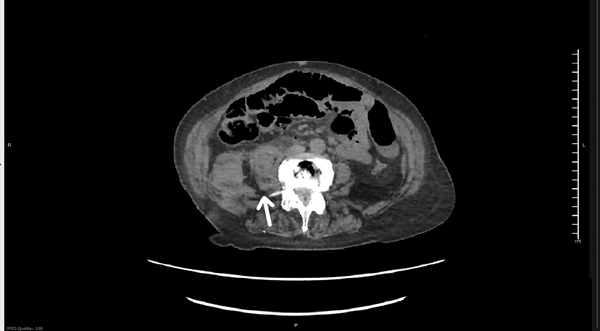
Plain films of the right hip and pelvis showed arthritic changes in all joints, with some soft tissue swelling overlying the right hip. US duplex of the right leg showed no evidence of DVT. Basic labs, including CBC and BMP, were within normal limits. Non-contrast CT of the pelvis and lumbar spine showed a moderate sized right iliopsoas hematoma and a small amount of retroperitoneal bleeding, consistent with iliopsoas muscle rupture. Orthopedic surgery recommended admission and a type and screen and PT/INR, which was within normal limits.
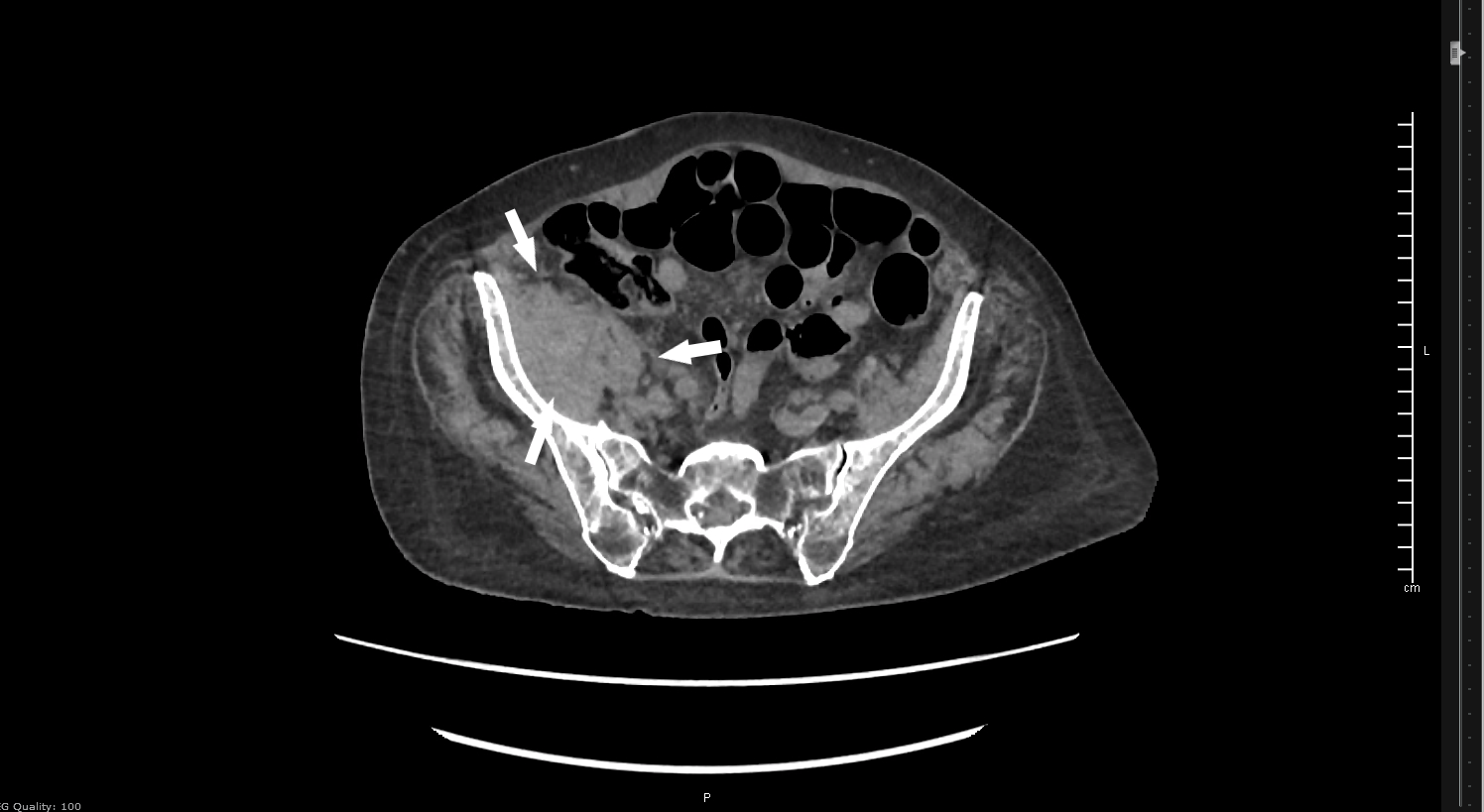
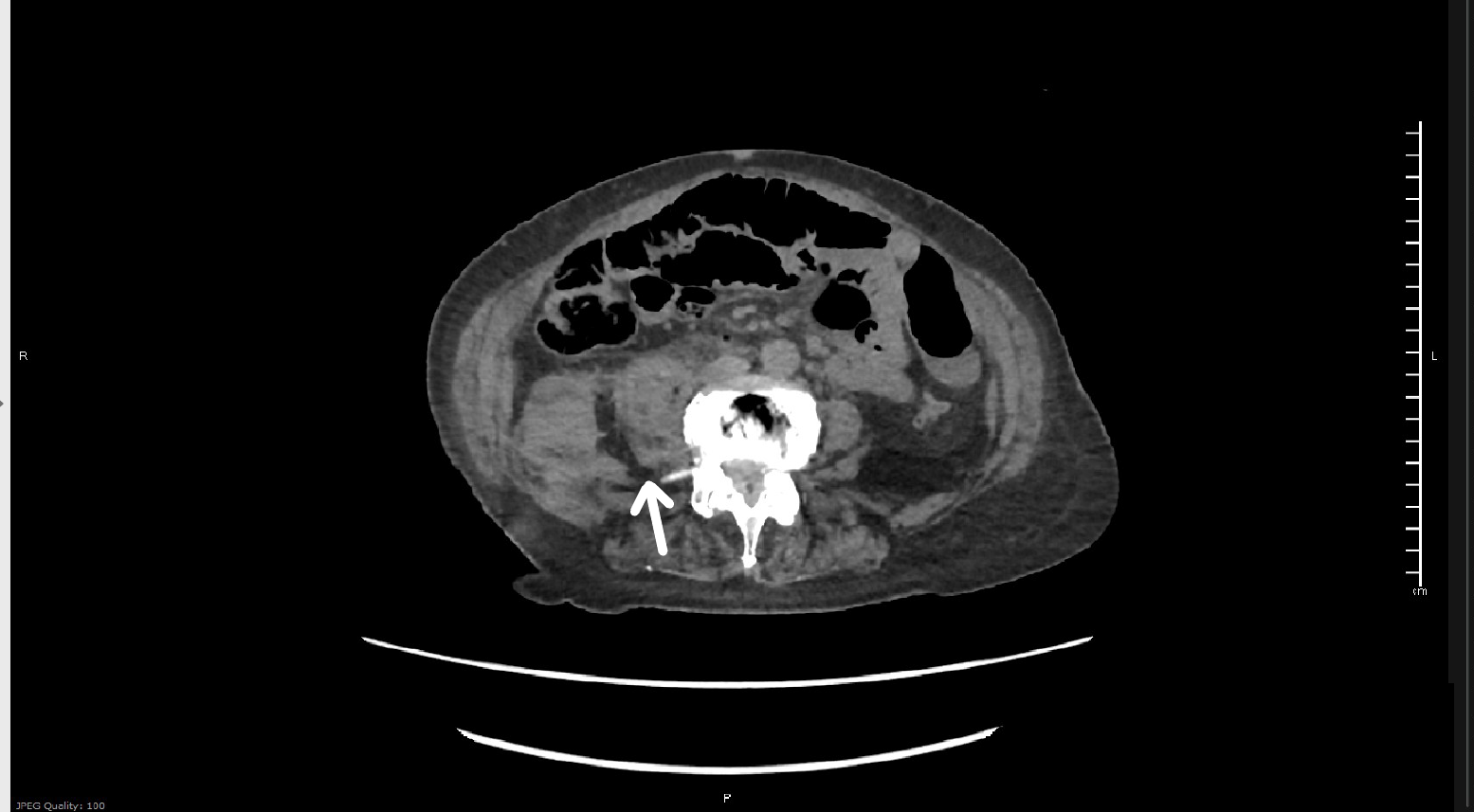
Image 1. Hematoma and retroperitoneal bleed. Image 2. Iliopsoas with edema
After admission, the patient was evaluated for surgical intervention. With pain control, she was able to ambulate, so surgery was deferred. Hemoglobin dropped from 11.3 to 9.9 but stabilized at that point. The patient received physical and occupational therapy and was discharged 2 days later.
Discussion
Spontaneous iliopsoas rupture is an extremely rare cause of atraumatic hip pain seen in the elderly. Iliopsoas injury is usually seen in the setting of athletic trauma. The prevalence of atraumatic and traumatic iliopsoas tendon injury is 0.66%. The most common risk factors for atraumatic tendon injury are age, female sex, chronic steroid use, osteopenia, fluoroquinolone use, metastatic cancer, and chronic inflammatory diseases.1 Risk factors for rupture and hematoma formation include uncontrolled hypertension, underlying bleeding disorder, or anticoagulant use.2,3,4,5
Iliopsoas tendon injuries can be complete or incomplete tears. Complete tears tend to be more painful and present with greater disability, depending on the patient's baseline functional status and concomitant injuries. Decision to admit mostly relies on ability to ambulate and pain control. It would not be unreasonable to discharge an ambulatory patient with pain medication and follow up to primary care for physical therapy or orthopedic surgery referral. Activity restrictions would include weight lifting and fast movements. Most patients will likely be best served with admission, pain control, and orthopedic surgery consult.
CT is often used to diagnose rupture or hematoma. The most sensitive imaging is MRI; however, it is not routinely done because of cost and the lack of added value in management.6 The management is usually conservative, including physical rehabilitation and pain management, though more invasive procedure might be necessary in the setting of continued bleeding or expanding hematoma compressing on vital structures.
Overall, prognosis is quite good, though life-threatening anemia and hypovolemic shock can arise. Anticoagulants should be reversed, and underlying bleeding disorders should be treated as otherwise appropriate.7
References
1. Rubio M, Rodriguez M, Patnaik S, Wang P. Spontaneous Iliopsoas Tendon Tear: A Rare Cause of Hip Pain in the Elderly. Geriatr Orthop Surg Rehabil. 2016;7(1):30–32.
2. Tsai J, Yang P, Lin H, Chang C. Spontaneous Iliopsoas Hematoma. J Emerg Med. 2016;51(3):e53-e54.
3. Yogarajah M, Sivasambu B, Jaffe E. Spontaneous iliopsoas haematoma: a complication of hypertensive urgency. Case Reports. 2015;2015: bcr2014207517.
4. Türkkan, E., Atay, D. Y., Ocak, S., & Ozdemir, G. N. Iliopsoas Hemorrhage in Pediatric Patients with Hemophilia, Experience from One Centre. Blood. 2015;126(23), 4571.
5. James SL, Davies AM. Atraumatic avulsion of the lesser trochan-ter as an indicator of tumour infiltration. Eur Radiol. 2006;16(2):512-514.
6. Petchprapa C, Bencardino J. Tendon Injuries of the Hip. Magn Reson Imaging Clin N Am. 2013;21(1):75-96.
7. Rock J, Basheer A, Jain R, Anton T. Bilateral iliopsoas hematoma: Case report and literature review. Surg Neurol Int. 2013;4(1):121.