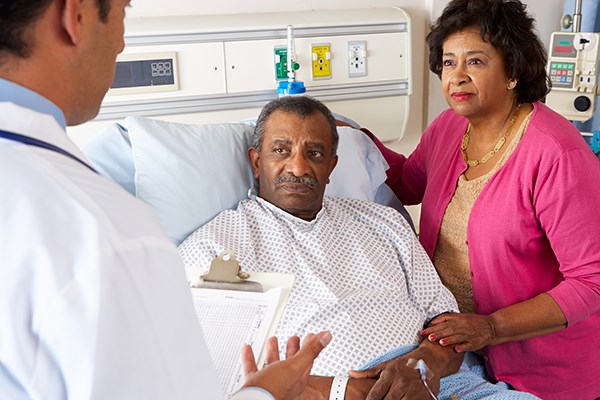
If your care saves the patient but leaves their mind wounded, have you fully cared for the patient? Adopting a practice of premeditated compassion would allow us to offer our patients empathy even as we develop the tunnel vision common to acute care situations.
My second shift as an intern was a long haul. Swamped with tasks, the learning curve I was on felt more like a wall.
So it was with relief that I noticed I was 20 minutes away from the time at which I wouldn’t pick up any new patients. Two people were still in my care and I would likely not be signing out anyone to the next shift.
Then, looking at the board once more, I saw the little red box pop up: a new patient. The conflict ate at me. I wanted to cross the finish line that was just 20 minutes away. I also wanted to be the intern who never let a patient sit on the board. I saw my co-residents fighting the same battle as they hovered their mouses over the “Assign Me” button.
My patients happened to be more tidied up at that point, so I took the plunge, picked up the patient, and went to meet the EMS squad. They waited in a hallway tucked between the main patient care areas. This hallway was where cramped rooms begged for simple encounters and quick dispositions. The stretcher clogged the space, making me squeeze between it and the linen basket to get to the foot of the bed. That squeeze reminded me of what I had been feeling the entire shift: simple things being complicated by unrelated demands. Finally, I found my mark and I asked the paramedic for the story.
“Doc, we got a call because he all of a sudden felt weak in both of his legs and couldn't move them.”
As the monologue progressed the patient was whirled into the room and hooked up to the monitor. I heard the nurse say, “When did you have that aortic sleeve placed?” That question pulled me into the room. Entering it felt like the start of a simulation case. The diaphoretic man before me was groaning in pain, yelling for us to do something. The vitals on the monitor were ominous.
Fast-twitch decisions started to happen. I had rehearsed these. EKG ordered. Access obtained. My fourth-year resident brought the ultrasound to the bedside.
“Doc, just put me down already. I can’t take this pain!”
The melodrama of it shook me. I remember freezing for a moment and thinking “Is this a simulation?” As in any simulation, we continued to act quickly. Attending to the bedside. No pulses on Doppler. CT angiography of the chest, abdomen, and pelvis with runoff. STAT read requested. Vascular Surgery paged.
CT Read: “Complete occlusion of the aortobifemoral bypass graft due to occlusion at its proximal end with poor renal enhancement and no distal flow”
The patient was handed off to the resident covering the Shock Resuscitation Unit and I finished my night.
Reflection and Review
Running back the “tape” of my first critically-ill patient felt like those painful moments when I watched the recordings of standardized patient encounters as a medical student. I saw myself standing in the radiology room as the patient was transferred to the scanner. I was saying, “We need CTA with runoff to the toes. He has an aortic graft and it looks like there are no pulses in his feet.” The patient's hands were secured above his head. He lay there naked, while I talked loudly with the radiology technician about the protocol. The tech now knew more about my patient’s condition than the patient. My sense of urgency had led to disregard; I had failed to inform my patient what was going on.
In replaying this scenario, I realized that I almost never spoke to the patient, explained what was happening, or addressed what we were doing. He was a mannequin sitting on a stretcher with mechanical pupils and there was an attending behind the glass screen telling me how bad his pain was. The lack of consideration I showed my patient was counterbalanced only by my ability to manage the encounter clinically.
Simulation Plus
After this case, I would never question the value of training with simulation. This case forced my mind to move down clinical pathways that have been worn deeply into my brain via simulated cases. What became clear is that committing to a clinical pathway is not sufficient to treat our future patients; we also must engage with them compassionately. In this case, it is clear, my medical decision-making outpaced my ability to care for this patient with compassion.
This subordination of compassion to medical decision-making does not surprise me. Saving a life is more important than tripping over words. Yet, I can’t help but wonder: if my care saves the patient but leaves their mind wounded, have I fully cared for them? The tension between compassion and critical care arises because the former requires complex cognition that is nearly impossible to muster when every neuron is being utilized to manage a situation clinically. This is why our training for compassionate care should not be reserved for controlled conversations about how to deliver cancer diagnoses; it must include acute care situations. Our patients need this, as the compassion we show in critical moments is directly related to the number of patients leaving our care with PTSD.1
If I could go back to that evening, the compassionate care that I wish I had offered would be premeditated; not robotic, contrived, or fabricated compassion, but deliberately practiced. Maybe then I would have used the 30 second trip to the CT scanner to tell my patient about what was happening to him.
Take-Away
We all desire to show our patients compassion. Adopting a practice of premeditated compassion would allow us to do so reflexively even as we develop the tunnel vision common to acute care situations. Working through this deliberate practice shows the value we give to others as we sacrifice time to prepare for their worst days.
Reference
- Moss J, Roberts MB, Shea L, et al. Healthcare provider compassion is associated with lower PTSD symptoms among patients with life-threatening medical emergencies: a prospective cohort study. Intensive Care Med. 2019;45(6):815-822.