Although high-pressure injection injuries may only leave small superficial wounds, they can create widespread multilayer soft tissue injuries, deep-space infections, and lead to compartment syndrome. What's your first move?
Pressure washer injuries are rarely seen in the emergency department but have major consequences if underlying injury or extent of the injury is missed or overlooked. Although underlying trauma is normally examined and ruled out by CT scans, initial x-rays can help effectively triage and diagnose deeper soft tissue damage. In this case, initial x-rays in the emergency department were able to demonstrate significant soft tissue trauma, thus enabling the patient’s treating physicians to quickly initiate appropriate antibiotics and analgesics and begin trauma consultation and admission.
Introduction
We present a patient with extensive underlying tissue damage diagnosed on initial x-rays after sustaining a pressure washer injury. We report here how a high-pressure injection injury with only superficial physical exam findings can have significant damage that extends beyond the wound or injury itself secondary to shearing forces and energy dispersion after the initial insult. Diagnosis of underlying trauma in the emergency department is usually completed by CT scans, however, we demonstrate that initial use of x-rays can be an efficient way to triage and begin appropriate treatment for high-pressure injection injuries and to effectively diagnose underlying trauma. This is important in the emergency department since major complications of these types of injuries include acute extremity compartment syndrome, infection and can lead to limb amputation.
Case
A 32-year-old male presented to the emergency department with a chief complaint of right forearm pain. The patient, who is left-handed, was using a pressure washer at work, about 20 minutes prior to emergency department arrival, when it slipped and hit the volar aspect of his right forearm. On arrival, the patient complained of severe pain in the volar aspect of his arm extending through his wrist and elbow, which was made worse with the slightest extension movement. He held his wrist in a flexed position secondary to pain. The patient noted that he was otherwise healthy and denied any other medical problems. On further questioning he did not know if his tetanus was up to date.
On inspection, the patient endorsed pain from his right elbow down to his hand. He had a 1-2 cm circular superficial injection wound on the distal third of this volar forearm without surrounding erythema or edema. He had full range of motion of his fingers, wrist, and elbow. His sensation and motor strength were intact. Due to suspicion for extensive subcutaneous injury at bedside, x-rays of the patient’s right arm were ordered immediately after initial evaluation. Examination of the images showed extensive subcutaneous air dissecting through multiple tissue planes extending from the initial injection wound location both distally to his wrist and proximally down his forearm. This can be a common finding after high-pressure injection injuries. The patient was then started on intravenous antibiotics, unasyn and gentamicin, analgesia, and trauma surgery was consulted. The trauma team examined the patient at bedside and he was admitted for further monitoring with frequent neurologic checks and pain control. Ultimately, the patient received a fasciotomy and wash-out secondary to worsening compartment pressures and concern for underlying infection. Several days later he was discharged with a fully intact neurologic function and outpatient follow-up.
Image 1: Right forearm lateral x-ray showing extensive subcutaneous air beyond superficial wound location outlined by the white circle.
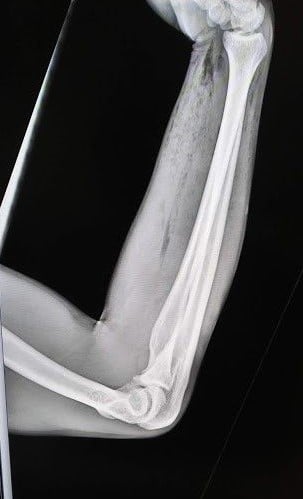
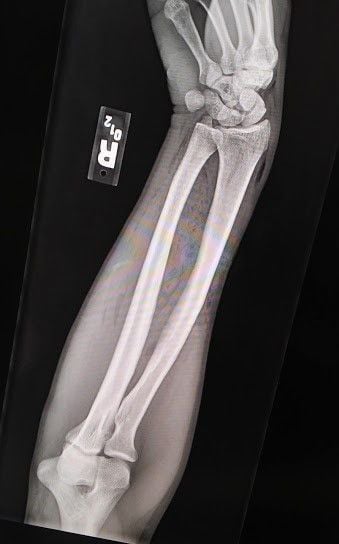
Image 2: Right forearm anterior-posterior x-ray showing subcutaneous air into the wrist and hand
Discussion
High-pressure injection injuries most often occur on the patient’s non-dominant hand or arm.1 The degree of underlying damage has a high risk of being underestimated on presentation secondary to small or superficial surface wounds. Up to 30% of pressure injuries eventually require amputation and expert surgical opinions in case reports even recommend that all high-pressure injection injuries receive a fasciotomy within six hours from injury onset in order to decrease amputation risk.2 Pressure washer injuries, like other high-pressure injection injuries (including paint, gas, air, and grease), can inject gas or liquid into the surrounding and underlying soft tissues increasing risk for infection.3 The foreign material dissects quickly through tissue planes, increasing pressure within the muscle compartments and restricting blood flow due to extraluminal pressure on blood vessels. Additionally, the disseminated foreign material can seed bacteria throughout the affected areas, creating a risk for deep space infections and worsening inflammation. Several case reports throughout the United States and Europe illustrate worse outcomes for those with high-solute and non-organic solvent injections as these exposures require larger debridements and serial washouts to remove foreign material.4 For these reasons, patients should be admitted to the hospital for continuous monitoring and serial physical and neurologic exams even if initial imaging does not reveal any significant underlying damage.5,6 Consensus statements from both trauma and plastic surgeons recommend broad spectrum antibiotics as well as updating tetanus status.7 After admission, physicians may have difficulty controlling severe pain from these injuries; however, digital and other nerve blocks should be avoided as they can mask worsening pain or loss of sensation which are often the first signs of compartment syndrome.
Conclusion
Although high-pressure injection injuries may only leave small superficial wounds, they can create widespread multilayer soft tissue injuries, deep-space infections, and lead to compartment syndrome. Even if x-ray and CT scans are negative, it is highly recommended that these injuries receive urgent consultation, admission, antibiotics, and analgesia.
TAKE-HOME POINTS
- If a pressure washer or other high-pressure injection injury is suspected, consider initial screening x-rays instead of CT scans to detect deeper, underlying damage.
- However, always maintain a high degree of suspicion for high-pressure injection injuries regardless of imaging findings. Early fasciotomy may lead to improved outcomes.
- All high-pressure injection injuries require an updated tetanus status, broad-spectrum antibiotics and effective analgesia. Nerve blocks should be avoided a they may cloud serial neurovascular and compartment checks.
- Remember, even if initial imaging does not show signs of underlying damage, it is important to still consider deeper injuries in these patients as they will require admission for close monitoring and IV antibiotics.
References
- Sirio CA, Smith JS Jr, Graham WP 3rd. High-pressure injection injuries of the hand. A review. Am Surg 1989;55:714-718.
- Hogan CJ, Ruland RT. High-pressure injection injuries to the upper extremity: a review of the literature. J Orthop Trauma 2006;20:503.
- Giladi AM, Chung KC. Fasciotomy for compartment syndrome of the hand and forearm. Operative Techniques: Hand and Wrist Surg 2017;13.
- Bekler H, Gokce A, Beyzadeoglu T, Parmaksizoglu F. The surgical treatment and outcomes of high-pressure injection injuries of the hand. J Hand Surg Eur Vol. 2007;32(4):394-399.
- Dailiana HZ, Kotsaki D, Varitimidis S, et al. Injection injuries: seemingly minor injuries with major consequences. Hippokratia 2008;12(1):33-36.
- Scott AR. Occupational high-pressure injection injuries: pathogenesis and prevention. J Soc Occup Med. 1983;33(2):56-59.
- Amsdell SL, Hammert WC. High-pressure injection injuries in the hand: current treatment concepts. Plast Reconstr Surg. 2013;132(4):586e-591e.



