A 53-year-old man presents to the ED for worsening pain associated with a longstanding whole-body rash. He states that 2 years ago a small blemish started on his chest, and it spread to involve predominantly his forearms, chest, and legs. He has previously been to the ED for the same symptoms and was discharged with cream for eczema.
The patient states his skin has been dry, flaky, with pink-red scales and plaques. The pain is alleviated by applying lotion, but as soon as the lotion dries the pain returns.
Physical exam is unremarkable except for the findings exhibited in these photographs. What is your assessment of this condition?
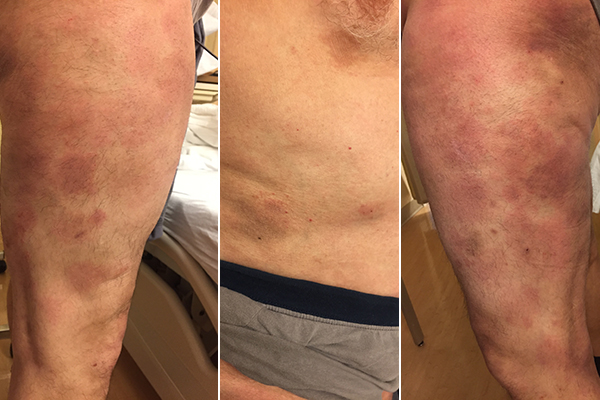
Mycosis Fungoides
Mycosis fungoides is a T-cell lymphoma commonly misdiagnosed as eczema or other dermatological issue. Because of this, it is often mistreated and can be frustrating to the patient for many years. Proper diagnosis and treatment is often multifaceted, based on extent of disease.
Definition
• T-cell lymphoma in which neoplastic lymphocytes infiltrate the epidermis and form plaques, nodules, and ulcers
Diagnosis
• Skin biopsy Epidemiology
• Middle age and older adults
Etiology
• Unknown
• Possible virus or bacterial Ag
Clinical
• Early-patch
— Flat, scaly lesions more than 5 cm in photo-protected sites
— Round, ovoid, or digitate dermatosis (finger-shaped)
— Referred to as "plaque parapsoriasis"
— Poikiloderma vasculare atrophicans: history of regressing to wrinkled macules of hypo- and hyperpigmentation with telangiectasia
• Plaque
— Same location and size as patches, but lesions are thicker, varying shades of red-brown with induration and elevation
— Occasionally ulcerate
• Tumor
— Solid nodule at least 1 cm that arises within or adjacent to pre-existing patches and plaques
— Frequently ulcerate
• Sézary syndrome
— Leukemic form of mycosis fungoides
Management
• Hematology consultation
• Topical or intralesional corticosteroids (1st line)
• Bexarotene
• UVA or UVB phototherapy
• Apheresis
• Total Skin Electron Beam (TSEB)



