The Patient
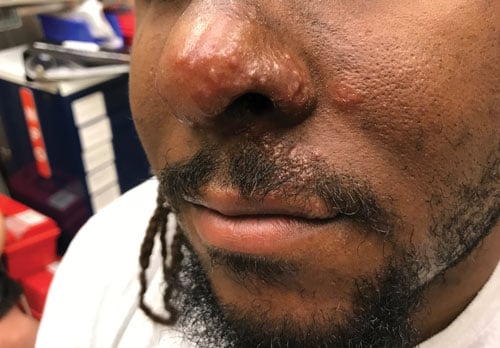
30-year-old male with no significant past medical history presents with 2 days of gradually worsening rash over the left nare, left upper lip, and inferior medial epicanthus. It is pruritic and mildly relieved with application of hydrogen peroxide and rubbing alcohol. Patient denies fever, eye pain or discharge, otalgia, headache, or blurry vision. He also denies exposure to any new hygiene, household cleaning products, or insects. He is up to date on his vaccinations and had an episode of heat exhaustion at work one week ago.
What is the diagnosis?
What is the treatment?
The Diagnosis
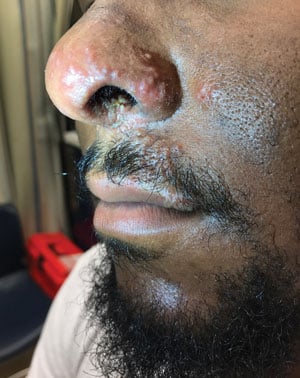
Herpes zoster is caused by reactivation of a latent infection of the varicella zoster virus (VZV), a member of the herpes virus family. During initial infection, VZV establishes a lifelong latency within the dorsal root ganglion of sensory neurons. Reactivation can occur due to many causes, such as immunosuppression, stress, or local trauma. The incidence also increases with age.1
In this patient, reactivation was most likely due to the recent episode of heat exhaustion at work. During reactivation, the virus travels down the sensory nerve in the cutaneous distribution to produce the characteristic pruritus, paresthesias, burning, and rash. Pain can appear 48-72 hours prior to onset of rash, which is vesicular, unilateral, and limited to dermatomal patterns.1-2
Ramsay Hunt syndrome (herpes zoster oticus) is a major otologic complication of reactivation within the V2 and V3 branches of the trigeminal ganglion (CN V), which may also lead to involvement of cranial nerves VII and VIII.3 The typical triad of symptoms includes ipsilateral facial paralysis, ear pain, and vesicles visible in the auditory canal or on the auricle.2 Patients can also develop taste perception dysfunction on the anterior 2/3 of the tongue, tinnitus, hyperacusis, and lacrimation. If not treated, facial paralysis and hearing loss may become permanent.3 Treatment of herpes zoster oticus consists of a combination of antivirals (valacyclovir or acyclovir) and prednisone (5 days, without a taper).
The goals of therapy are to limit the extent, duration, and severity of pain in the primary dermatome; prevent disease dissemination; and prevent post-herpetic neuralgia. Treatment of herpes zoster in immunocompetent patients should begin within 72 hours of onset of rash and should only be considered after that time frame if the patient is developing new lesions.4
This patient had a single vesicle inferior to the medial epicanthus. Evaluation of the auditory canal revealed no lesions, and the patient did not have facial paralysis. A fluorescein stain of the eye was also performed and was negative for herpes keratitis. The patient was treated as an outpatient with acyclovir 800mg 5 times a day for 7 days with close primary follow up.
References
- Schmader KE, Oxman MN. Chapter 194. Varicella and Herpes Zoster. In: Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, Wolff K. eds. Fitzpatrick’s Dermatology in General Medicine, 8e New York, NY: McGraw-Hill; 2012.
- Whitley RJ. Varicella-Zoster Virus Infections. In: Kasper D, Fauci A, Hauser S, Longo D, Jameson J, Loscalzo J. eds. Harrison’s Principles of Internal Medicine, 19e New York, NY: McGraw-Hill; 2014.
- Andrus P, Guthrie J. Acute Peripheral Neurologic Disorders. In: Tintinalli JE, Stapczynski J, Ma O, Yealy DM, Meckler GD, Cline DM. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e New York, NY: McGraw-Hill; 2016.
- Takhar SS, Moran GJ. Serious Viral Infections. In: Tintinalli JE, Stapczynski J, Ma O, Yealy DM, Meckler GD, Cline DM. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e New York, NY: McGraw-Hill; 2016.



