Spinal epidural abscesses are a rare condition affecting the spinal column, but if left untreated, they can rapidly become fatal.
The incidence of spinal epidural abscesses are 0.2 to 2.8 cases per 10,000 per year. Peak incidence occurs in patients between 60-70 years old. Often, the abscess is due to Staphylococcus aureus (S. aureus), however, other microbes such as Actinomycosis, Gram-negative bacilli, and fungi can cause spinal epidural abscesses. Overall, S. aureus causes 63% of spinal epidural abscesses, while fungal strains cause roughly 10% of infections.1
Risk factors for spinal epidural abscesses include:
- Spinal trauma
- Spinal procedures or surgery
- IV drug use
- Diabetes mellitus
- Chronic renal failure
- Alcoholism
- AIDS
- Malignancy
Diabetes mellitus is the most common risk factor, with about 33% of the patients diagnosed with a spinal epidural abscess also having a history of diabetes.2,3 Meanwhile, IV drug use and spinal manipulation (such as placement of an epidural catheter) are becoming more prevalent risk factors in recent years with the opioid epidemic and advances in chronic pain medicine, respectively.
The classic triad of symptoms a patient might present with includes back pain, fever, and neurologic deficits secondary to compression from the abscess. However, only about 8% of patients will present with all three. If spinal epidural abscess is on the differential, it is important for the clinician to obtain prompt evaluation to minimize morbidity and mortality. Ultimately, though, preoperative status including age, comorbidities, and time to diagnosis and treatment best predicted morbidity and mortality rates.4,5
Case
A 37-year-old female presented to the emergency department endorsing symptoms of fatigue and frequent sensation of restless legs. She also described having to crawl around for parts of the day, reporting that she felt too weak to use her legs. She had been seen at another facility 3 days prior and had basic labs performed, which were unremarkable. Over the past 24 hours, she continued to grow weaker, now returning to the emergency department for another evaluation. She denied any chest pain, shortness of breath, nausea, vomiting, diarrhea, or skin changes. When asked, she endorsed a past history of IV drug use and hepatitis C.
Exam
Physical exam revealed a disheveled female who appeared older than her stated age. Her vital signs were remarkable for a heart rate of 100 beats per minute. Otherwise she was afebrile, had a normal blood pressure of 115/60, a respiratory rate of 16 breaths per minute, and an oxygen saturation of 100% on room air. Her cardiopulmonary exam was unremarkable. The patient had scabs in different stages of healing over her body with evidence of track marks in the antecubital fossa of her bilateral arms. She had diminished strength, reflexes, and sensation in all four extremities, including inability to feel pinpoint sensation. Jerking movements were noted in the bilateral lower extremities that the patient reported she could not control. No rashes were seen throughout the integumentary examination and she had normal, intact rectal tone.
Pathophysiology
Most spinal epidural abscesses are located at the posterior aspect of the thoracic or lumbar spine. Posterior abscesses are thought to originate from a distant focus, such as the skin or from dental etiology. Anterior abscesses are predominantly due to discitis or vertebral osteomyelitis and can be caused by direct extension from retropharyngeal or retroperitoneal abscesses.1 Vertebral hematomas due to trauma are seen in up to 35% of cases and a nidus of blood serves as a nutrient source for bacteria to breed.
The pathophysiology of spinal epidural abscesses stems from the ability of bacteria to enter the epidural space. Normally, this part of the spinal column is sterile, however, once bacteria are able to enter, they tend to coalesce in a suppurative infection within the confined epidural space. Bacteria have a few ways to enter this space, the most common being via hematogenous spread. Manipulation of the spinal column with epidural catheter placement, spinal surgeries, and via lumbar puncture are also ways for bacteria to enter the central nervous system and spinal column via direct inoculation.
Diagnosis
Diagnosis of a spinal epidural abscess by physical exam alone is often difficult as most patients do not present with the classic triad that was previously mentioned. Pain is one of the most common presenting symptoms, which may be found on palpation of the spinous processes near or overlying the spinal epidural abscess. Another physical exam finding is pain with straight leg raise, which will cause compression of spinal nerve roots. Neurologic deficits can develop as abscesses increase in size, causing symptoms consistent with cauda equina syndrome. These include but are not limited to urinary retention, bowel incontinence, and perianal/saddle anesthesia. Patients may also report weakness with leg movement, paralysis, or numbness.5 Fever is present in 35-60% of patients; however, absence of fever cannot rule out spinal epidural abscess.6
Laboratory evaluation includes complete blood count, blood cultures, coagulation studies, and inflammatory markers. Oftentimes erythrocyte sedimentation rate (ESR) is elevated, but normal levels do not exclude the diagnosis of spinal epidural abscess. ESR sensitivity ranges from 68-100%, however, one case series posited only an ESR above 50mm/hour was considered positive. In a meta-analysis of 915 patients with spinal epidural abscesses, the sensitivity of an ESR was noted to be 94%. C-reactive protein has a similar sensitivity to ESR at 84-100%, but is a more effective marker of early disease as it rises faster than the ESR and is influenced less by other plasma factors. Presence of leukocytosis is extremely variable and does not predict the severity of disease. Given leukocyte count is a nonspecific lab marker, it should not be used to exclude the diagnosis of spinal epidural abscess. For imaging, magnetic resonance imaging is the test of choice. If unavailable, CT with IV contrast is another option, although it is less sensitive.6
Management
Management includes neurosurgical evaluation for any patient with evidence of epidural abscess or with an abnormal neurological examination from mass effect. These patients will often require emergency evacuation to decompress the spinal cord and nerve roots. Endoscopy-assisted surgery and percutaneous drainage have been reported to be successful in some cases. Nonsurgical candidates include those with minimal neurologic deficits or who are poor surgical candidates. Patients who are deemed surgical candidates will need to undergo aspiration, surgical drainage, and antibiotic therapy for 4-6 weeks post-surgery. Repeat MRI should be obtained at 4-6 weeks of therapy or if there is evidence of worsening symptoms or deteriorating clinical examination.
Antibiotic regimens include the following:
- Preferred: vancomycin + a 3rd or 4th generation cephalosporin (cefotaxime, ceftriaxone, ceftazidime, or cefepime)
- Alternative for suspected pseudomonal infection: vancomycin + cefepime
- Alternative for penicillin allergy (non-anaphylaxis): vancomycin + meropenem
- Alternative for severe penicillin allergy: vancomycin + aztreonam
- Alternative for vancomycin allergy: linezolid + secondary antibiotic as indicated above
- Be advised when using linezolid that serotonin syndrome is possible if the patient is on an SSRI or MAOI1
Prompt diagnosis and management is important for patients with an underlying abscess, as delay in diagnosis can result in irreversible neurological damage. Around 4-22% of patients diagnosed with spinal epidural abscess will have irreversible paraplegia. Around 5% of patients will die from sepsis. A prospective evaluation of clinical decision guidelines to diagnose spinal epidural abscesses in patients showed that 75% of patients diagnosed with spinal epidural abscess suffered delays in diagnosis. A permanent neurological deficit was nearly 6 times more likely in those who suffered a delay.7
Case Conclusion
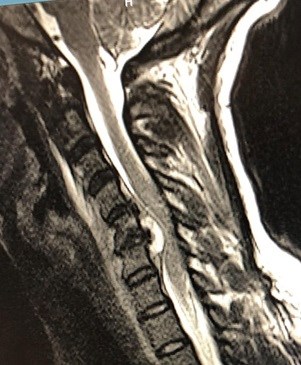
After the physical exam, it was determined the patient had symptoms consistent with a potentially catastrophic neurological process. Laboratory workup revealed a normal white blood cell count of 9.8, a slight anemia with hemoglobin of 10.8 and hematocrit of 36, and a normal platelet count of 390. ESR was elevated at 89 mm/hour and CRP was elevated at 62 mm/hour. Renal function panel revealed a normal BUN and creatinine at 20 mg/dL and 0.70 mg/dL, respectively. Urinalysis showed no evidence of infection. Bedside echocardiogram showed no evidence of vegetative lesions on the valves and showed a normal ejection fraction. The patient had a normal post-void residual bladder volume. CT angiogram of the chest showed no evidence of pulmonary embolism or underlying pneumonia. MRI of the spinal cord showed discitis osteomyelitis with a large epidural abscess at C5-6 compressing the spinal cord. It also noted epidural phlegmon extending from C3-7 with prevertebral phlegmon extending from C2-T1. The patient was given broad spectrum antibiotics including vancomycin and cefepime and was transferred to a tertiary medical center for neurosurgical evaluation.
Take-Home Points
- Spinal epidural abscess is a difficult diagnosis to make. It should be on your differential when evaluating patients with back pain and other neurologic symptoms, especially those patients at increased risk, such as diabetics and IV drug users.
- Antibiotic choice must include Staphylococcus aureus coverage.
- Prompt diagnosis and treatment is important for epidural spinal abscesses to avoid permanent neurologic damage.
References
- Chao D, Nanda A. (2002, April 01). Spinal Epidural Abscess: A Diagnostic Challenge.
- Fotaki A, Anatoliotaki M, Tritou I, Tzagaraki A, Kampitaki M, Vlachaki G. Review and case report demonstrate that spontaneous spinal epidural abscesses are rare but dangerous in childhood. Acta Paediatr. 2019 Jan;108(1):28-36.
- Du JY, Schell AJ, Kim CY, Trivedi NN, Ahn UM, Ahn NU. 30-day Mortality Following Surgery for Spinal Epidural Abscess: Incidence, Risk Factors, Predictive Algorithm, and Associated Complications. Spine. 2019 Apr 15;44(8):E500-E509
- Ameer MA, Knorr TL, Mesfin FB. Spinal Epidural Abscess. [Updated 2020 Mar 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020.
- Darouiche RO, Hamill RJ, Greenberg SB, Weathers SW, Musher DM. Bacterial spinal epidural abscess. Review of 43 cases and literature survey. Medicine (Baltimore). 1992;71(6):369-385.
- Chenoweth CE, Bassin BS, Mack MR, et al. Vertebral Osteomyelitis, Discitis, and Spinal Epidural Abscess in Adults [Internet]. Ann Arbor (MI): Michigan Medicine University of Michigan; 2018 Dec.
- Ghobrial GM, Beygi S, Viereck MJ, et al. Timing in the surgical evacuation of spinal epidural abscesses. Neurosurg Focus. 2014;37(2):E1. doi:10.3171/2014.6.FOCUS14120