Thalidomide’s Resurgence and its Contemporary Uses
Katelynn Baska, OMSIII, Jonathan Meadows, DO, and Peter Mattson, MSIV
You are a third-year resident working in the ED one night when the following patient arrives: a 65-year-old man with a five-year history of type 2 diabetes mellitus and a less than one-year history of multiple myeloma presenting with a complaint of left lower extremity pain and paresthesias in his hands and feet. He reports that the numbness and tingling began two days ago but the onset of leg pain wasn’t until early this afternoon. His wife is present at the bedside and relays that he has also had a few episodes of confusion throughout the day, for example, mixing up the sugar and salt on the table and forgetting that their cat died, an event that occurred two years prior. The patient reports that he has never experienced these symptoms before but was diagnosed with multiple myeloma seven months ago. His current medications include metformin 500 mg BID, dexamethasone 40 mg, and thalidomide 250 mg qHS. When asked about his social history, he reports that he “drinks a few beers” every day but denies tobacco or illicit drug use.
Your initial differential diagnosis includes: deep vein thrombosis, diabetic peripheral neuropathy, cellulitis, superficial thrombophlebitis, vitamin deficiencies (i.e. B6, B12), lumbar radiculopathy, disc herniation, syphilis, medication toxicity, and Wernicke-Korsakoff Syndrome. On physical exam, his left leg is erythematous and edematous, and he has decreased sensitivity to sensory stimuli in all four extremities. He has a negative straight leg raise and mild paraspinal hypertonicity but no pain or bony asymmetry. His CBC shows mild leukopenia and his CMP is positive for hypercalcemia - consistent with the diagnosis of multiple myeloma. BUN and creatinine are within normal limits and his HbA1C is 6.7%. RPR is negative and his serum vitamin B12, B6, and B1 levels are within normal limits. Ultrasound of the left lower extremity reveals a clot in the peroneal vein. What next steps do you take in the care of this patient? What is your current working diagnosis? Did you consider thalidomide toxicity as a possible etiology?
Created in the 1950s by German pharmaceutical company, Chemie-Grunenthal, thalidomide was initially marketed as a non-addictive, nonbarbiturate sedative. It was later prescribed as an antiemetic during pregnancy in the late 1950s and 1960s and gained notoriety as in utero exposure was linked to an upsurge of infants born with phocomelia (congenital malformation of the arms and legs). Throughout the world, more than 10,000 children were affected by the use of thalidomide, and it prompted the establishment of more stringent methods of drug testing and screening, including the incorporation of multiple species in clinical trials due to the realization that differences in species sensitivity impact outcomes. Thalidomide was taken off the market worldwide in 1962.1,2,3
When you think of thalidomide, however, it would be erroneous to think only of its use as a historical cautionary tale; thalidomide is, in fact, still used as an effective component of treatment today. Its anti-angiogenic properties make it a useful therapy for those suffering from multiple myeloma. In addition, it has been found to successfully treat complications of leprosy, systemic lupus erythematosus (SLE), Behcet’s syndrome, Langerhans cell histiocytosis, and graft vs. host disease, due to its potent anti-inflammatory properties.3 Though it was banned from use in pregnant women, publications demonstrating its utility as a treatment for erythema nodosum leprosum began to crop up in the mid-1990s and research on the drug has since exploded - especially within the past ten years.3 The resurgence in the use and interest in thalidomide has brought about new information, precautions, and side effects of which medical providers should be aware.
One such example is the creation of the prescriber safety program or S.T.E.P.S. (System for Thalidomide and Prescribing Safety) program. This program has three major goals:
1) to control access to the drug;
2) to educate prescribers, pharmacists, and patients; and
3) to monitor compliance.
Certain S.T.E.P.S. criteria and procedures must be followed. For example, prescribers and pharmacists must be registered in the S.T.E.P.S. registry, and patients are counseled on the importance of not becoming pregnant while being treated.4 Female patients of childbearing age must undergo pregnancy testing and agree to take two forms of contraception while undergoing therapy. Men taking thalidomide must agree to use a condom during sexual intercourse and refrain from donating semen as the drug has been found to be present in semen.5 Despite these precautions, there has been a recent spike in thalidomide-induced fetal malformations in Brazil due to the prevalence of leprosy in the country and the practice of medication sharing, exposing people who have not been properly educated on its use and teratogenicity.
Those who have properly followed the procedures of the S.T.E.P.S. program are not completely out of the woods when it comes to dealing with the effects of thalidomide toxicity. As illustrated in the case above, thalidomide (and analogs of thalidomide) can lead to fairly benign side effects such as sedation, constipation, and fatigue. However, increased doses (>200mg/day) and longer treatment duration (>6 months) can elicit symptoms such as peripheral neuropathy, thromboembolic events, confusion, and edema. Toxicity also tends to occur more frequently when thalidomide is combined with dexamethasone or other chemotherapeutic drugs.6 According to the National Cancer Institute Common Toxicity Criteria, Grade 1-2 peripheral neuropathy can occur in greater than 80% of patients, while more severe neuropathy (Grades 3-4) occurs in roughly 3-5% of patients.6 Typically, reduction of thalidomide dosing or temporary withholding of treatment results in resolution of these symptoms. However, higher-grade neuropathy should be treated with complete discontinuation of thalidomide therapy. Coagulopathies, such as DVTs and PEs, occur in about 1-3% of patients taking thalidomide, but co-administration of dexamethasone increases the incidence to 10-12%.6 Additionally, concurrent use with chemotherapeutics such as doxorubicin increases the incidence of coagulopathy to greater than 25%.6 To avoid these consequences, prophylactic anticoagulants (i.e. warfarin, low molecular weight heparin, or aspirin) should be utilized for patients on combination therapies. Should a patient present with DVT or PE who is taking a combination treatment regimen, treatment should be discontinued immediately and the coagulopathy should be treated.6 With the increased use of thalidomide over recent years and an aging U.S. population, it is important to be cognizant of the necessary precautions for patients taking thalidomide and the symptoms of toxicity when you encounter patients in the ED who fall within this particular population.
References
-
Vargesson N. 2015. Thalidomide-induced teratogenesis: history and mechanisms. Birth defects research. Part C, Embryo Today: Reviews. 105(2): 140-156.
-
Botting, J. 2002. The History of Thalidomide. Drug News Perpective. 15(9): 604-611.
-
Kim, James H., Scialli, Anthony R. 2011. Thalidomide: The Tragedy of Birth Defects and Effective Treatment of Disease. Toxicological Sciences. 122 (1): 1-6.
-
Zeldis, JB, Williams, BA, Thomas, SD, Elsayed, ME. 1999. S.T.E.P.S.: A Comprehensive program for Controlling and Monitoring Access to Thalidomide. Clinical Therapy. 21 (2): 319-30.
-
Li, Y, Wang, X., Liu, L., Reyes, J., Palmisano, M., Zhou, S. 2018. Distribution of pomalidomide into semen of healthy male subjects after multiple doses. Clinical Pharmacology. 10: 53-62.
-
Ghobrial, Irene, Rajkumar, S. Vincent. 2003. Management of thalidomide toxicity. J Support Oncology. 1(3): 194-205.
Related Content


May 02, 2023
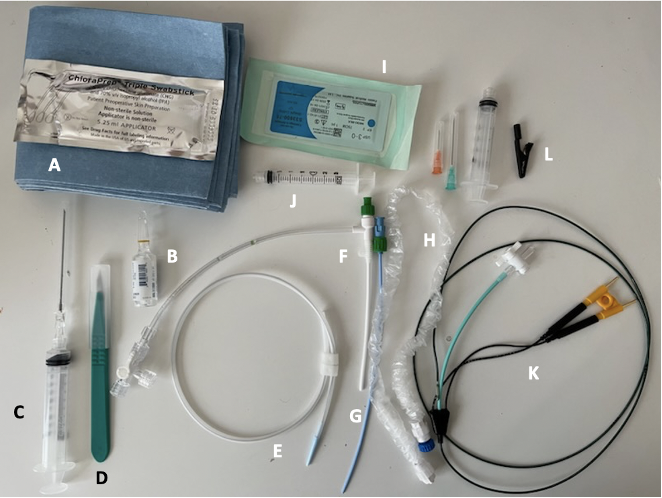
Critical Care Device Series: Transvenous Pacemaker
Temporary transvenous pacing (TTVP) utilizes central venous access to pass an electrode into the right ventricle. TTVPs are one of the most infrequently performed procedures by emergency physicians; however, it is essential for those working in any setting with critically ill patients to be well-equipped to perform this procedure emergently.




