Prepare for trouble - and make it double! DSD Revisited
Prepare for trouble - and make it double!
DSD Revisited
May 1, 2024
EMRA*Cast host Dustin Slagle, MD, and NYU critical care cardiology fellow James Ciancarelli, DO, revisit the topic of a prior episode – dual synchronous defibrillation – to further explore the theory, logistics, evidence, and indications for its use.
Host
Dustin Slagle, MD
NYU Pulmonary & Critical Care Medicine
dustyslags on Instagram
EMRA*Cast Episodes
Guest
Dual synchronous defibrillation is the application of two separate defibrillators and the synchronous or near-synchronous discharge of electricity delivered to a patient to convert an arrhythmia. Here we are specifically talking about shockable cardiac arrest rhythms: ventricular tachycardia and ventricular fibrillation.
DISCUSSION
As mentioned in this paper by former EMRA Critical Care Committee chair, Mark Ramzy, DO, EMT-P, there are three proposed theories for its use:1
1) Power Theory
One of the leading theories behind the success of DED is that the administration of more joules during transthoracic defibrillation allows for the conversion of all the myocytes out of RVF. This approach requires the two electrical currents from both defibrillator devices to be administered at the same time or as close together as possible and is where DED gets one of its more common names: “double simultaneous defibrillation” (DSiD).
2) Setting Up Theory
Another leading theory behind DED suggests that the first transthoracic current lowers the defibrillation threshold, which then increases the second transthoracic current’s success at converting any remaining fibrillating myocytes. This theory requires a deliberate pause when administering the two electrical currents to ensure they are close together but not delivered at exactly the same time; this is where DED gets its most common name of “double sequential defibrillation” (DSD).
3) Multiple Vector Theory
Another hypothesized theory behind DED directly applies to the two proposed theories above and suggests that application of multiple defibrillator pads increases the number of vectors the electrical current can use to reach the myocardium.
Logistically, DSD requires prep time, so it has to be considered early. Refractory ventricular arrhythmias are defined often by resistance to conversion after three shocks and DSD in studies and case reports is then used on subsequent shocks.1 This means the machines have to be ready as early as 5-6 minutes into the arrest.
The DOSE-VF trial studied DSD against a vector change strategy (changing anterior-lateral to anterior-posterior) and against standard of care before the trial in their region (anterior-lateral placement). The trial suggests both mortality and survival with good neurologic outcome for the use of DSD in refractory ventricular arrhythmias.2
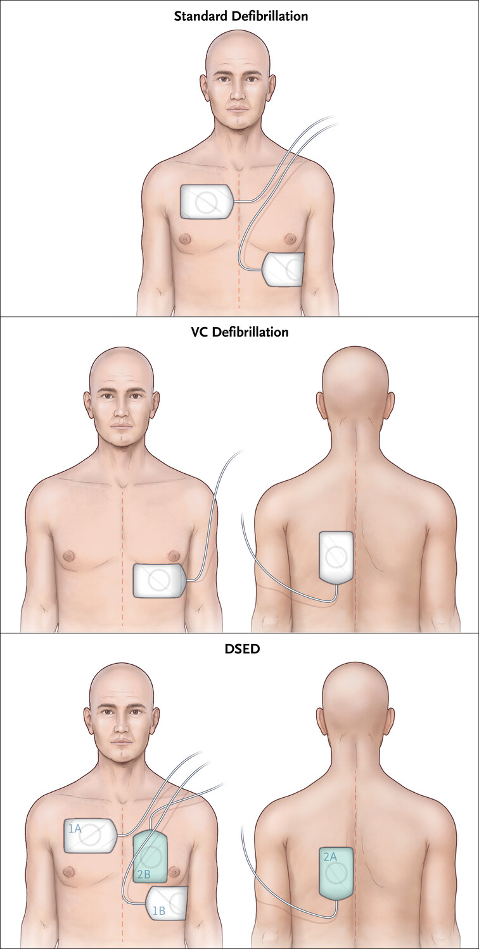
Figure from DOSE-VF trial
Good scientific practice would dictate that confirmatory studies are needed (including studies on ED and inpatient cohorts), but in the meantime in the absence of any known harm, it is reasonable to attempt DSD if your emergency department is capable, your team has prepared for it, and the patient could theoretically benefit from its use.
References
- Ramzy M, Hughes PG. Double Defibrillation. [Updated 2023 Apr 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK544231/
- Cheskes S, Verbeek PR, Drennan IR, et al. Defibrillation Strategies for Refractory Ventricular Fibrillation. N Engl J Med. 2022 Nov 24;387(21):1947-1956. doi: 10.1056/NEJMoa2207304. Epub 2022 Nov 6. PMID: 36342151.





