Ch. 4 - Finding Your Fit: Learning the Landscape of EM
One of the most exciting things about medicine is there is always more to learn. This is true for the application process as well. Now that you have decided on EM, the next thing you must consider is which type of residency will be best for you.
Factors Important for Residency Selection
While all EM residency programs must meet the ACGME Program Requirements, there is still room for significant variation between programs. Students applying to EM say many factors are important in deciding where they apply and ultimately rank programs, including geographic location, length of training, hospital type(s), clinical duties/experiences, reputation, program culture, and more.1-3 Many of these program attributes have been included as filter options in EMRA Match.
FIGURE 4.1. Common Attributes Students Ranked as Important When Evaluating an EM Residency Program1
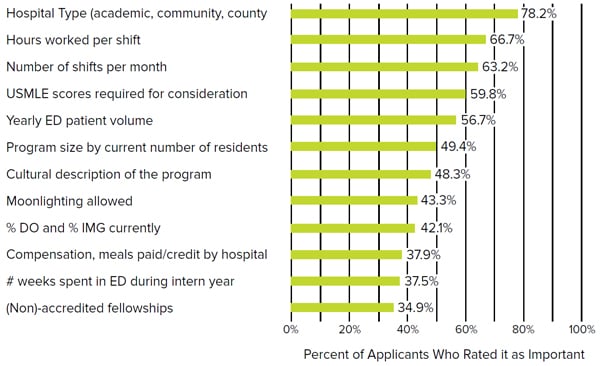
Location, Location, Location
Desired geographic location is typically the most important factor during both the application and ranking process. Some applicants want to be close to family, while others are looking to embark on a new adventure or seek unique social and recreational opportunities to enjoy when not at work. The cultural, racial, and ethnic diversity of the patient population may also vary by location. Residency programs in highly desirable urban areas will likely have a higher cost of living compared to other programs. Applicants with significant others may also need to consider job opportunities that will be available for their partners in each location. Many physicians end up practicing in the same geographic location where they completed their residency training.4
FIGURE 4.2. Geographic Locations Historically Favorable to DO/IMG Applicants5
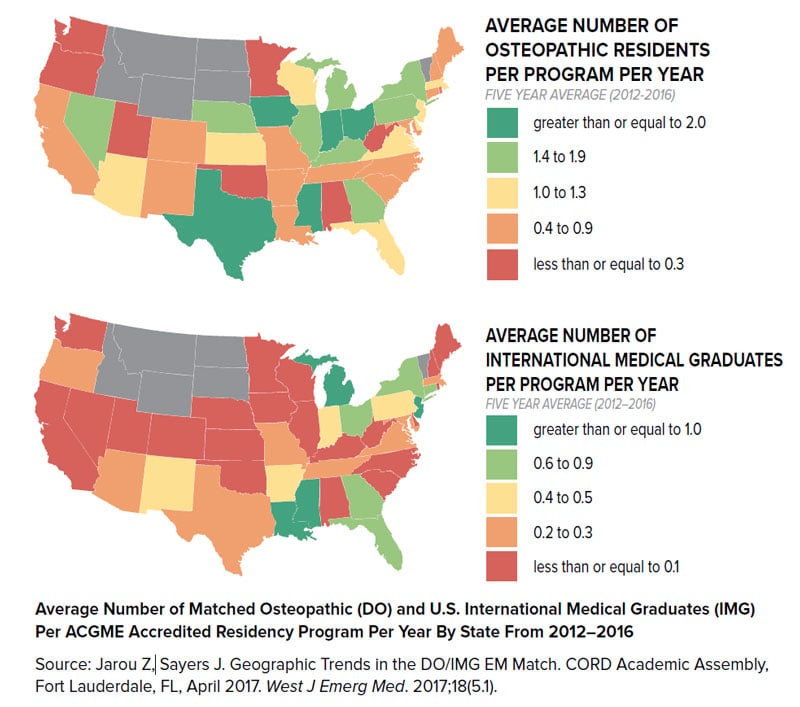
Couples Match: You don’t have to match at the same institution to be within a certain geographic distance of each other. Target cities and geographic locations that have multiple residency programs in each of your specialties.
Osteopathic and IMG Students: While osteopathic applicants will no longer have to make the decision to apply to AOA vs. ACGME programs due to the Single Accreditation System, certain states have traditionally matched a higher number of DO residents per program per year. The same holds true for IMG applicants.5
Comparing 3- and 4-Year Programs
One of the many things that makes EM unique is that applicants have the option of applying to both 3- and 4-year training programs. Approximately one-quarter of programs are 4 years in length. Applicants must weigh the opportunity cost of spending an additional year being paid as a resident, rather than an attending, with the benefits that can be gained by graduating from a 4-year training program.
Many applicants will apply to a mix of both 3- and 4-year programs, and must consider what makes an additional year of training at each program “worth it.” For example, an extra year of training may provide additional opportunities to teach students and interns, develop experience in maintaining the flow of patients throughout the entire ED, provide EMS medical direction, allow for unique clinical rotations outside of the ED or within an EM subspecialty area, allow for participation in a longitudinal specialty track during residency (see “Fellowships/Scholarly Tracks” section later in this chapter), or provide additional elective time to tailor their training experience to suit their individual needs. Elective time is an opportunity to explore other areas within EM, especially if you have special interests like international medicine, research, or ultrasound. This may help you decide about fellowship training, especially if you’re interested in a fellowship not available at your program.
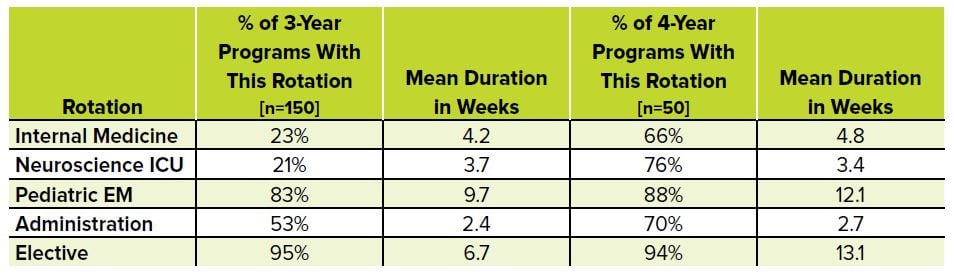
There is no difference in moonlighting opportunities, total critical care time, or percentage of time spent off-service during intern year between 3- and 4-year training programs; however, 4-year programs typically offer 14 weeks of elective time, compared to only 7 weeks of elective time at 3-year programs.2 Four-year programs are more likely to have Internal Medicine, Neuro ICU, and Administration rotations, and on average have an additional 2.4 weeks of time spent doing pediatric EM.6
TABLE 4.1. Similarities and Differences Between 3- and 4-Year Programs2
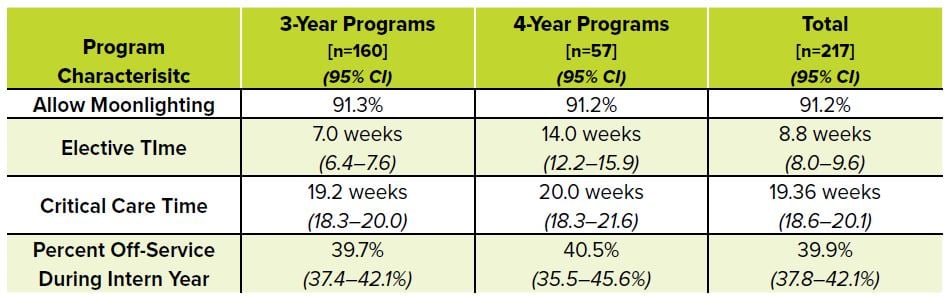
TABLE 4.2. Prevalence of Rotation Types at 3- vs. 4-Year Programs
Training Environment
Every residency program is housed at a sponsoring institution that assumes ultimate responsibility for ensuring the program receives the support necessary to successfully train residents. This sponsoring institution is typically the primary clinical site where residents complete their training, and may be a university, community, or county-based hospital (see Figure 4.3 for a breakdown of residencies by primary training environment). All EM residency programs must be affiliated with a medical school. Many residency programs have additional sites to provide exposure to experiences not offered at the primary clinical site. There are pros and cons to each type of training environment. You should consider which learning environment will best prepare you for your ultimate career goals.
FIGURE 4.3. Prevalence and Types of Primary Training Environments
Percentage of Residencies Self-Reporting Each Hospital Setting
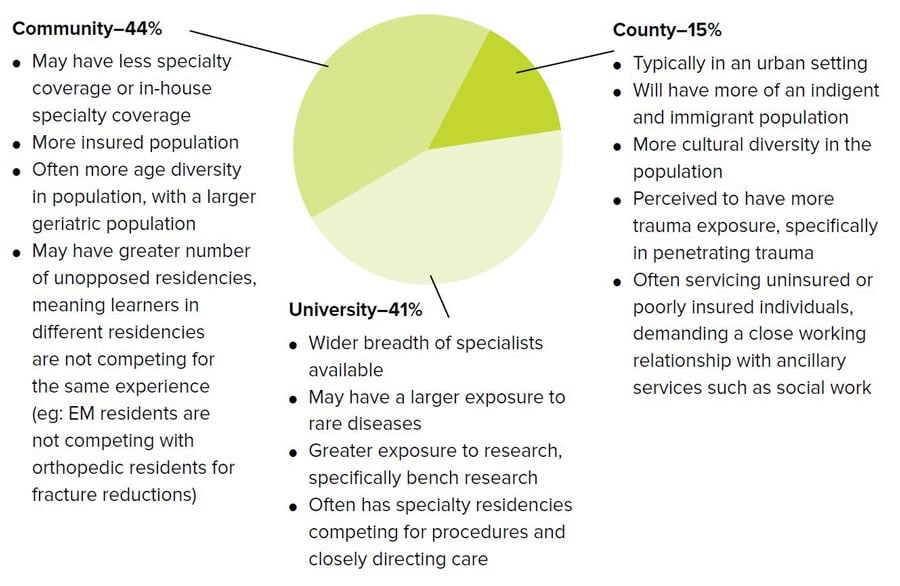
ED Patient Volume
While many applicants consider patient volume to be an important factor in choosing a residency program, this may or may not translate to increased learning opportunities. The ACGME requires that the primary clinical site and any ED where a resident spends more than 4 months to have a minimum of 30,000 annual visits. The primary site should also see a minimum of 3% or 1200 critically ill patients (whichever is greater). While some residency programs boast patient volumes in the hundreds of thousands, which may increase exposure to rare pathology, this may or may not hold true depending upon the staffing models used at each residency program. Some residency training programs will be located at institutions that also train or employ non-physician providers.
As EM is dedicated to the care of the critically ill, it can be important to explore the total number of critical care weeks during residency vs. the general nature of those critical care experiences to ensure a robust exposure to this field. In addition, many programs allow for additional critical care time to be used for electives if this is an interest of yours or you plan to pursue a fellowship.
Work-Life Balance: Length and Number of Shifts Per Month
Per ACGME rules, EM residents may not work longer than 12 hour shifts while in the ED. They must have a length of time off-duty that is equal to or longer than their scheduled shift length between each work period. Residents may not see patients for more than 60 scheduled hours per week in the ED (and no more than 72 total hours per week). EM residents must have at least 24 hours off every 7 days. Within these constraints, there is significant variability in the average shift length and number of shifts per month, though the majority of programs require interns to work 16–21 shifts per month that are each 9 hours or less. The number of shifts per month at a program may or may not decrease over the course of your training.
Many residents cite time for personal and professional needs as a crucial factor for burnout prevention. In one study, the authors conclude that “when baseline needs of adequate sleep and self-care are not met, the capacity for self-actualization is limited. The strained, moment-to-moment entality many residents experience does not permit introspection, processing of emotions, or learning from challenging patient encounters.”7 Applicants should try to find a program that will provide them with enough clinical exposure to become clinically excellent, while also considering their personal wellness and learning style. For example, those who learn best by seeing and doing may have a better educational experience at programs with more clinical duties, while those who learn best by reading and reflecting may be better suited to a program with more time for study.
TABLE 4.3. Average Length and Number of Shifts During PGY1
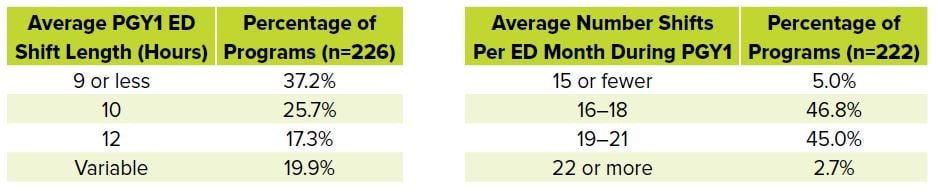
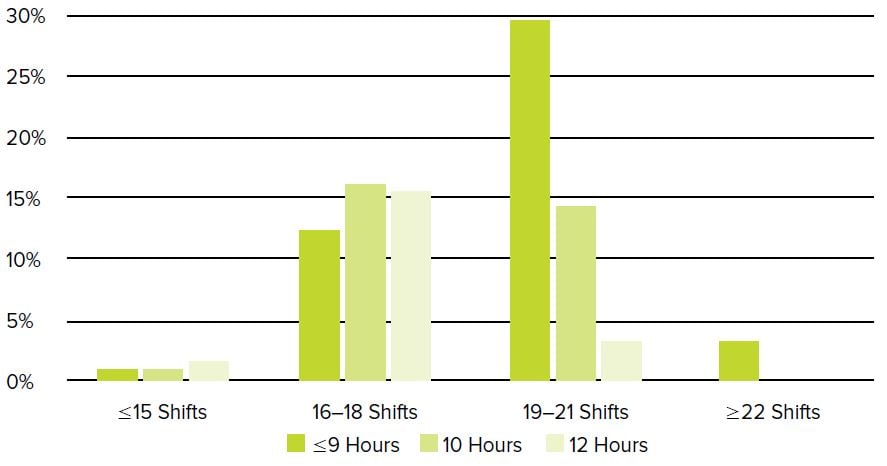
FIGURE 4.4. Percentage of Programs with Each Combination of Average PGY1 Shift Length and Frequency2
(n=177, programs with “variable” length of shifts excluded)
Program Size
The ACGME requires a minimum of 18 residents per EM residency program to foster a sense of community and to ensure there is a critical mass of learners to support educational activities. The largest EM residency is a four-year program that accepts 25 residents per year for a total of 100 residents. There is nothing inherently good or bad about a large or a small program. A smaller residency may have more dedicated one-on-one instruction and a closer-knit community, while a larger residency program may have greater resources, greater flexibility in scheduling, and more varied rotations. It is important to consider the number of clinical sites staffed by a program’s residents to understand how much actual opportunity for interaction you will have with your colleagues while on shift.
Residency Program Culture
Each residency program will have a relatively unique culture that results from the personalities who work there and the program’s priorities. Which factors are overall most important in determining if you will be happy at the program? Which training environment do you think you will work and learn best in? Do you need a family-friendly program? Are you looking for a program that will push you to your clinical limits, or one that will provide more time for pursuing research or other scholarly endeavors?
Program culture can be difficult to determine prior to visiting, though some sense of culture can be derived from social media profiles on Facebook or Twitter and their description of culture on EMRA Match. Lastly, spending time with current residents while on rotation or when visiting for an interview can give you a good “insider” perspective.
Moonlighting
The vast majority of EM residency programs (83%) allow residents to moonlight, either internally or externally.2 Moonlighting is permitted by the ACGME for non-PGY1 residents so long as it does not interfere with their education or cause a duty hours violation. Internal moonlighting allows residents to work additional shifts within their training program, which provides them an opportunity to assume the mindset of independent practice while still working in a department alongside their regular faculty. External moonlighting opportunities may allow residents to work at urgent care locations or in rural, critical access hospitals where they may be the only physician for miles, stabilizing patients for transport to facilities with more advanced capabilities.
Compensation & Benefits
Residents of all specialties training at each sponsoring institution are paid on the same PGY pay scale. Nationwide, the average starting salary for interns across specialties is $55,200, increasing to $60,700 for fourth-year residents.8 While there may be mild salary differences between programs given regional variation in cost of living, it is not recommended to make this a deciding factor in your rank list. Applicants may want to take note of additional benefits like meal plans, vacation time, parental leave policies, housing subsidies, and retirement plans.
Original Research vs. Scholarly Activity Requirement
The ACGME requires residents and faculty involvement in scholarly activity in order to maintain accreditation. The 2019 Common Program Requirements allow trainees and their program directors to use a wide variety of options to fulfill scholarly activity requirements, including discovery, integration, application, and teaching.9
Historically, 39% of EM residency programs have mandated resident scholarly activity requirements to be fulfilled by original research. Applicants seeking to fulfill their scholarly activity requirements by writing textbook chapters, presenting at national conferences, curriculum development, national leadership positions, or non-peer reviewed publications should pay attention to each program’s requirements.10
Fellowships/Scholarly Tracks
If you are already interested in a fellowship, then attending residency at a program that offers your hoped-for fellowship could be beneficial. You will likely have a better understanding of what the fellowship entails, plus the selection committee will already know you since they will have been your mentors during training. At the same time, it can also be nice to gain exposure to a different training environment by completing fellowship training in a new location.
Some programs offer scholarly tracks that can help establish a coordinated portfolio of work, increase scholarly output, and improve marketability.
For those who would like to begin developing a niche during residency, either in preparation for fellowship or to make themselves more marketable for a career in administration or academics, some programs offer scholarly tracks in areas such as medical education, administration, EMS, toxicology, ultrasound, and more. These tracks create mentorship communities within a residency program. Some programs require residents to participate in tracks, while others have optional tracks. During a 2009 working session at the CORD Academic Assembly, 8 residency programs shared their experiences with scholarly tracks, reporting that they helped residents create a coordinated portfolio of work in a single area of expertise, were associated with increased pursuit of academic careers by residency graduates, improved marketability for post-residency job search, and increased output of scholarly activity.11
Newer vs. Established Residency Programs
There is no data to suggest that an older vs. a newer program will give you a better residency experience. However, there are pros and cons to consider. A new residency will likely have more leeway to incorporate new ideas and innovations, allowing residents to make a lasting contribution to the program. A more established residency will have the advantage of being a known commodity with a larger alumni network to access when searching for jobs, fellowships, or niche types of mentorship. It is important to keep an open mind as either type of program may ideally serve your needs as a trainee.
Reputation
Picking a residency program based upon “reputation” should be avoided. There is no “best” residency program, only a set of programs that will be the best fit for you based upon your future goals, learning style, and lifestyle. In September of 2014, all major EM organizations wrote a co-signed letter to Doximity concerning the methodology behind the “Reputation” sort-by function in their Residency Navigator tool.12 Use of Doximity has been shown to cause one-quarter to one-half of applicants to change their rank lists, mostly by adding programs.13,14 Students are encouraged to consider objective data rather than unvalidated “reputation rankings” when comparing which program will best fit their needs.
Osteopathic Students: Historic/Ongoing Osteopathic Affiliation
Starting in 2020, all programs will be under a single GME accreditation system. If a student feels that maintaining an osteopathic-focused education is important, they will find a handful of historically AOA programs have applied for ACGME “Osteopathic Recognition,” which conveys their distinction in educational programming.
Use search filters (percent osteopathic residents currently at the program, acceptance of COMLEX in lieu of USMLE, etc.) in addition to reviewing data on the ACGME website to aid. Remember just because a program does not currently have an osteopathic resident, it does not eliminate your chances — but it should guide a realistic approach to applying.
The Bottom Line
- Start researching programs early to get a sense of what you find important in programs and which programs fit your needs.
- Multiple factors go into selecting a residency program. Only you can determine the program that is the best fit for you.
- Avoid relying on “reputation rankings” when considering which programs fit your needs.




