Ch. 2 - The Preclinical Years
If you have decided that emergency medicine is for you, then you are probably wondering what you can do to increase your chances of successfully matching. During the preclinical years, your performance in preclinical courses and participation in extracurricular activities can impact your chances of matching at your top-choice residency program.1
Start by reviewing the Emergency Medicine Medical Student Planner2 created by the CORD Advising Students Committee in EM. Additional planners have been created and specifically tailored for applicant populations such as osteopathic students and military students.
Academics: Preclinical Basic Sciences
Perhaps the most obvious component of the preclinical years are the basic science courses. Many schools are opting to grade courses as pass/fail, but regardless of the grading structure, having a full grasp on the information is necessary. In EM, we are proud to see all types of patients, and therefore are expected to initially manage and stabilize a wide range of maladies. Building a solid foundation will ideally prepare you for the COMLEX Level 1 and/or the USMLE Step 1 examinations, which ultimately will be used to compare you against other applicants. Step 1 preparation begins Day 1.
At-Risk Candidates: Failing a course will be seen as a red flag, but failing one course does not automatically disqualify you from a residency in emergency medicine. What is most vital is identifying the reason for the failure and taking corrective action.
If you feel overwhelmed by the workload, reach out to the course director or someone in your school’s office of student affairs. Many students have been able to excel in undergraduate courses with mild learning disabilities, but under the pressure of medical school are unable to cope with the vast amount of work. Early recognition is important, and your school likely has resources to assist you. Furthermore, there are many time-management resources online, ranging from videos to customizable planners and calendars.
Failing multiple preclinical courses is a more difficult hurdle to overcome. Often when a student fails multiple courses, they fall behind their original class. Failing two courses in first year typically can be remediated in the summer. Failing two or more courses in second year may cause the clinical portion of school to be delayed. If you fail two or more courses in the preclinical years, then working with the office of student affairs will be necessary, as staying in phase with your class will be weighed against your chances of scholastic success.
If you are still considering applying to EM, find an EM advisor as soon as possible. Failing multiple courses puts you at a higher risk of failing to match in EM unless proactive measures are taken.
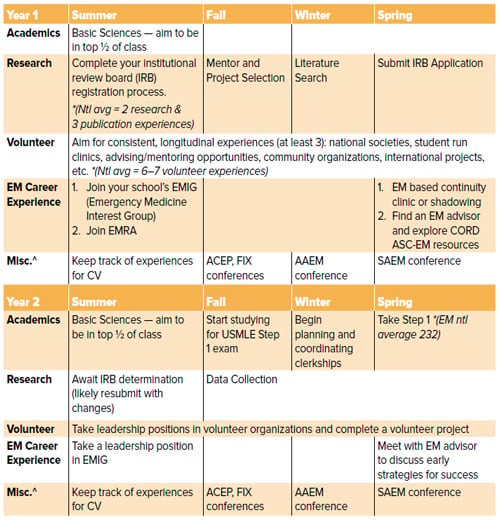
Table 2.1 CORD ASC-EM Medical Student Planner2
Source: CORD ASC-EM Planner
It is worth noting a few other ways that your pre-clinical performance will play a role in the residency application process. First, the Dean’s Letter, or Medical Student Performance Evaluation, includes information on your preclinical performance. The MSPE is a required component of the residency application and is reviewed by residency leaders when deciding which students to invite for interviews. Second, preclinical performance is considered by school committees responsible for selecting honor society or fraternity members for induction into Alpha Omega Alpha or Sigma Sigma Phi.
Finding Mentors and Advisors
Finding advisors and mentors can be as difficult as it is to agree upon a definition of the two terms. During the preclinical years, many medical schools will assign advisors. Your school may have a career development center, with faculty and staff assigned to advise students. While their advice is important and often accurate, their role is different from that of a mentor. The CORD ASC-EM defines advisors as emergency medicine academic faculty who provide specialty-specific, evidence-based advice.
In contrast, mentors will help coach you and often act as a role model. They are able to provide guidance and can offer intelligent direction on more generalized career advice. Mentors should be individuals whose professional and personal advice you seek and whose character you hope to emulate in your own life. Regardless of your academic performance during your preclinical years, finding quality advising and mentorship will be beneficial, and there are multiple people who can fill such roles. A mentor can be a peer who can offer their recent experiences to help guide you. If your school has an EM residency program, then shadowing a resident or faculty member can help establish a mentor/mentee relationship.
Ideally, you should obtain an advisor who is designated by your school or EM department and is affiliated with an ACGME-accredited residency program. If such a person is not available, then start by contacting physicians in the ED and let them know you are seeking an EM advisor. While anyone who is residency-trained in emergency medicine can provide career guidance, a faculty member with expertise and experience in advising students through their preclinical and clinical years in preparation for EM match is best.
If your school does not have an affiliation with a core teaching hospital or a residency program, review the CORD ASC-EM advising resources at https://www.cordem.org/communities/committees/advising-student-comm. You may also benefit from the EMRA Student-Resident Mentorship Program.3 This online service allows students to connect with residents who self-identify as mentors. Students can also join virtual advising sessions through EMRA Hangouts.
Lastly, faculty advisors are often available during your EM elective or out-of-town rotations; consider asking the clerkship director or one of their residency leaders for advising.
Osteopathic Students: Your institution may not offer EM-specific academic advising if not affiliated with a residency program.12 If this is the case, consider reaching out to recent grads and national mentoring programs through ACOEP-RSO, EMRA, or CORD.
Emergency Medicine Interest Groups (EMIGs)
A commitment to emergency medicine can be difficult to demonstrate during the preclinical years. One easy way is to join your school’s EMIG. By joining the group, you will gain insight into the world of emergency medicine. Skills workshops, ranging from suturing to advanced cardiac resuscitation, are often provided. Talks from local and regional experts are especially useful. In addition to being a member of the EMIG, you can potentially become a leader of the organization. As a leader, you are guaranteed to have a seat at the workshops, and you will also gain other valuable experience. Lastly, through your local EMIG you will often meet seasoned advisors and mentors, and you may find more opportunities for research or clinical experiences.
Preclinical Exposure to EM
At many schools EM is not a required rotation during your clinical years, so you may have limited exposure prior to the time you need to decide which specialty to apply to. Since it may be difficult to find extra time to shadow in the ED while on other clinical rotations as a third-year, spending time in the ED early on can play a crucial role in helping you decide if this is the environment where you can see yourself spending the rest of your career.
Service, Leadership, and Advocacy
The NRMP Match data shows the mean number of volunteer experiences as 7.3 for allopathic students, 6.0 for osteopathic students, 18.8 for U.S. IMG students, and 4.3 for non-U.S. IMGs.1,4,5 While sporadic volunteer opportunities such as a day in a soup kitchen or working a support tent at a 10K are important, long-term involvement with a program is viewed as more substantive.
PDs in emergency medicine were surveyed by the NRMP, and 69% reported that leadership qualities were an important factor in determining competitiveness for residency. This is noted to be more important than your personal statement and honor society membership.6
While EMIGs are a great way get your “feet wet” with leadership roles, additional options to get involved is through local, state, and national emergency medicine organizations such as EMRA and ACEP. By getting involved at the state or national level, you can advocate for the interests of your patients and colleagues and develop the skills to become a leader. These are also great opportunities to meet other students and physicians who are excited about emergency medicine. While leadership and extracurricular activities may help enhance your residency application, remember that mastering the basic sciences and building strong foundational knowledge should always come first.
Research as a Medical Student
Program directors use many criteria to help select their residency class. The number of research experiences by various applicant groups varies (Table 2.2). Though this amount of research involvement may seem intimidating during medical school, many medical students have performed research previously. The application for residency often includes all research performed, including research done during undergraduate and graduate education. Fortunately, the PD survey demonstrates that only 33% of PDs said research was important for offering interviews, and only 20% said it was important for ranking.6
Table 2.2 Average Research Experience of Successful EM Candidates in the 2018 NRMP Match1,4,5
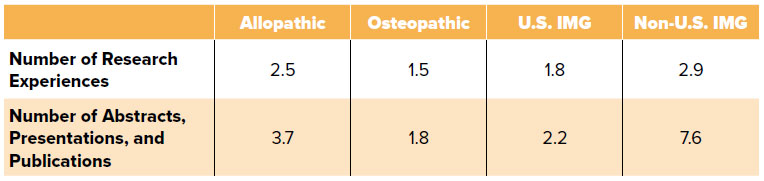
While performing research can be beneficial, finding the “perfect” research project during medical school can be difficult. Doing research just for the sake of doing research is often not advised, especially given the lower emphasis EM PDs place on this activity. Furthermore, doing research to pad your CV or to have another talking point during your residency interviews is also not advised. It is usually clear during the interview process how much involvement one had in the projects they list, and whether they were actually passionate about what they did.
If your school does not have a department or division of emergency medicine, then finding a project that interests you outside of EM is an option. Most medical schools have a contact for research opportunities. If your medical school does not, reach out to faculty in emergency medicine to see if there are any research projects for you to join. Lastly, your medical school may be in close proximity to another, and perhaps you can find a research project and possibly an advisor or a mentor at that location.
Initial Medical Licensing Exam
Finding leadership opportunities in medical school will provide valuable experiences, contribute to a robust EM application, and ultimately contribute to your effectiveness as an emergency physician. However, no amount of leadership, research, or volunteer activities can compensate for a medical licensing exam failure.
According to the NRMP 2018 PD survey, 97% reported that USMLE Step 1/COMLEX Level 1 score is important in deciding whom to interview.6 According to NRMP Match Data, the mean score for those students who successfully match in emergency medicine is 233 for USMLE Step 1, and 569 for COMLEX Level 1.1,4
Because Step 1 performance is highly important to EM PDs, you should start planning early how to best prepare for the exam. First, talk with your mentors, especially if they are residents or students more senior to you. You may find it beneficial to purchase commercially available review books, flashcards, and question banks as study aids during your preclinical years to maintain basic science knowledge through Step 1. Recent research suggests that retrieval practice in the form of practice questions and spaced repetition in the form of flash cards are two of the most effective ways to prepare for the USMLE.7 While passing your classes needs to be your top priority, studying the relevant board review material simultaneously is a great way to prepare for Step 1.
Osteopathic Students: Though osteopathic medical schools require COMLEX Level 1, Level 2CE/PE, and Level 3 for licensure, many residency programs require USMLE Step 1 and/or 2 for all applicants. While there are some residency programs that require either USMLE Step 1 or 2, there are some that specifically require Step 1. Use EMRA Match to filter programs based on licensing examination performance and if USMLE is a requirement. As noted in a recent survey conducted by CORD ASC-EM, only half of the programs who consider osteopathic students will offer an interview without either step of the USMLE, but 87% would offer an interview if the applicant had taken USMLE Step 1.8 Of the program directors surveyed, 27% did not weigh the COMLEX at all.8
Acceptance of COMLEX scores may change as the applicant pool expands, the move to a single accreditation system is complete, and programs become more comfortable with interpreting the COMLEX. In November 2018, the AMA House of Delegates created a policy calling for the AMA to promote equal acceptance of USMLE and COMLEX scores.9 However, at present, available data indicates if you are an osteopathic medical student, taking the USMLE Step 1 and 2 in addition to the COMLEX will open more opportunities for residency interviews. If you are unable to take both, prioritize USMLE Step 1. In addition, studying specifically for the USMLE will help maximize your chance of success.10
At-Risk Candidates: While most students take and pass USMLE Step 1, some do not. Not passing Step 1 of the licensing examination will significantly impact your application strategy. According to the 2018 NRMP PD survey, 98% of respondents would seldom or never interview a student with a Step 1 failure.6 However, an unpublished survey by CORD ASC-EM indicates there are programs willing to consider applicants who retake Step 1 and pass.8 Ifyou fail Step 1, contact your office of student affairs and your advisor so you can come up with a plan to retake the exam and perform well. Students often wonder if performing below-average will negatively affect their chances of matching. In a recent survey conducted by CORD ASC-EM, approximately half of programs will not consider an applicant who failed USMLE Step 1; however almost all interview applicants with below-average scores.8 While some programs filter applications in ERAS based on licensing exam scores, not all do.11 Further, you can take steps to compensate for a below-average score by taking Step 2 early and ensuring strong performance on clinical rotations. Students can use EMRA Match to filter which programs report having recently interviewed applicants who have previously failed Step 1.
As you look forward to the clinical years of medical school, remember that the best students and physicians built strong foundational medical knowledge during the preclinical years of medical school. The effort you put forth during your first 2 years will pay dividends for you and your patients as you move into your clinical rotations, residency, and beyond.
The Bottom Line
- The preclinical years provide a crucial foundation for the knowledge needed to succeed on medical licensing exams, during your clinical years, and on your emergency medicine rotations. Effort in the early years is a huge return on investment for the residency application process.
- Seek out opportunities to explore EM early; this will help you decide if EM is a good fit for you.
- If you have a red flag such as a low or failed Step 1 score or a failed preclinical course, seeking early guidance from an EM advisor is critical.
- When planning your research and volunteer activities, keep in mind that PDs value meaningful commitment over sporadic and superficial involvement (quality over quantity), and choose to dedicate your time to activities you truly care about.




