EM Match 2020 By the Numbers
Nico Ramsay, MSIV, FIU Herbert Wertheim College of Medicine
EMRA MSC Southeast Coordinator 2019-20
There has been a lot of chatter in recent years about emergency medicine (EM) becoming “more competitive.” But what do the numbers show? Although there are multiple ways to answer this question, one could argue that the best method is to compare the total number of applicants with the total number of available residency slots. Here we analyze some of the latest data from ERAS, which paint a more optimistic picture of this year’s application cycle.
How many people applied for EM this year?
As of October 15 (one month after ERAS opened) there were 3,640 applicants to EM residencies this cycle.[1] This number has been steadily rising over the last 10 years (Figure 1); in 2011 there were just 2,903 applicants. Interestingly, the number of International Medical Graduate (IMG) applicants has declined during that same time, before increasing slightly this cycle.
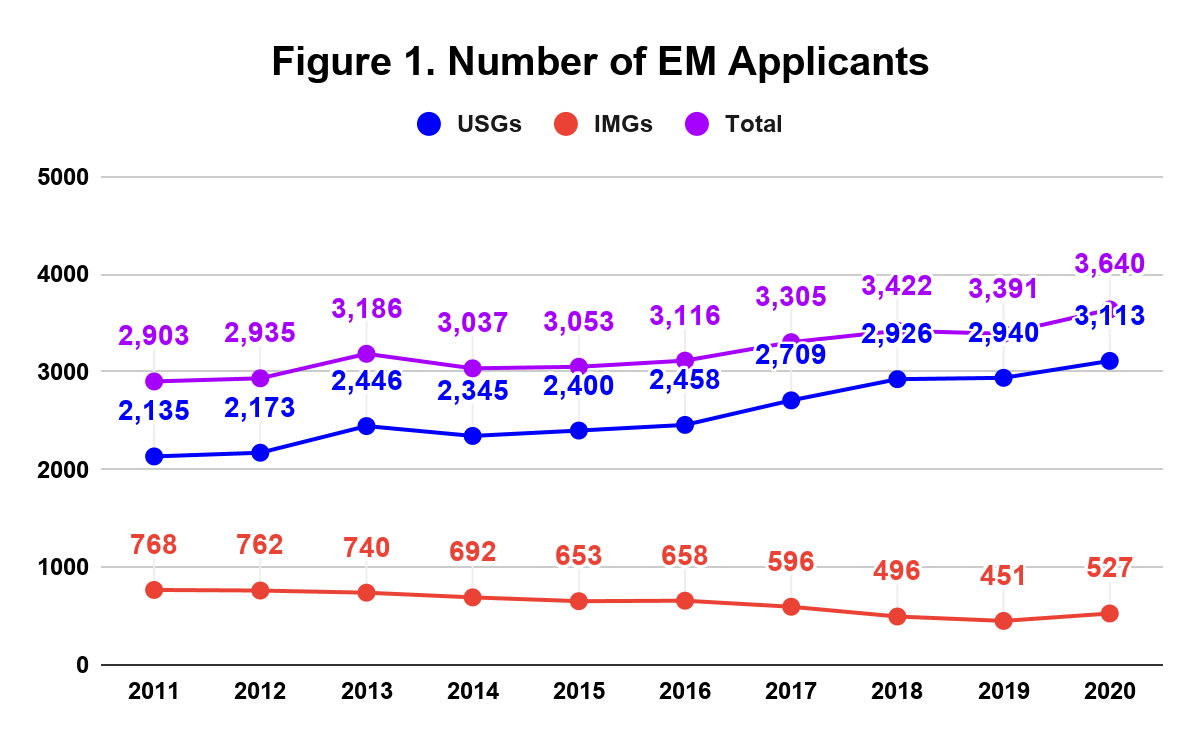
Is the specialty keeping up with the demand?
You may be thinking the natural follow-up question: “is the number of available EM residency positions also increasing to keep up with the increasing number of applicants?” The short answer is: yes. Figure 2 shows the total number of applicants each year compared to the available positions. In 2011, for example, there were only enough EM positions to accommodate 55 percent of applicants. This ratio has trended favorably for EM applicants each year. For the 2020 Match, there are 2,567 available positions for 3,640 applicants, a ratio of 71 percent.[1] Even more encouraging, the number of available positions this year does not include numerous programs that will likely be accredited by the end of this cycle, opening up even more spots. Furthermore, many applicants ultimately withdraw their applications or do not submit rank lists, further increasing the odds by the time March comes around.
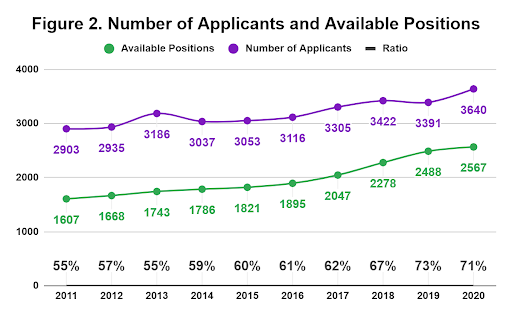
Did I apply to too many programs?
Although this question should be answered on a case by case basis, Figure 3 shows the average number of programs to which applicants applied. This number has steadily increased over the last ten years. This cycle, United State Graduates (USGs), which includes Canada, applied to an average of 58 programs, while the mean for IMGs was 75. Both figures are record highs. It is hard to know the reason for this steady increase. Perhaps applicants are being encouraged by their mentors to “apply more broadly,” but this has resulted in an increased burden on the programs receiving ever more applications.
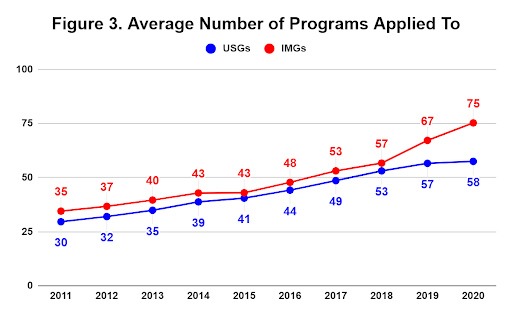
How many applications does each program receive?
If you’re applying this cycle, it is possible you have received a rejection email by now that includes a statement such as “we received a record number of applications this year.” But how many applications do these programs actually receive? Figure 4 shows the average number of applications per program and this cycle the number is a whopping 889. That’s right: on average, each program is sifting through almost 1,000 applications in order to decide who they should invite to interview. So if you have received an interview invitation that means you truly are among a select few for that program.
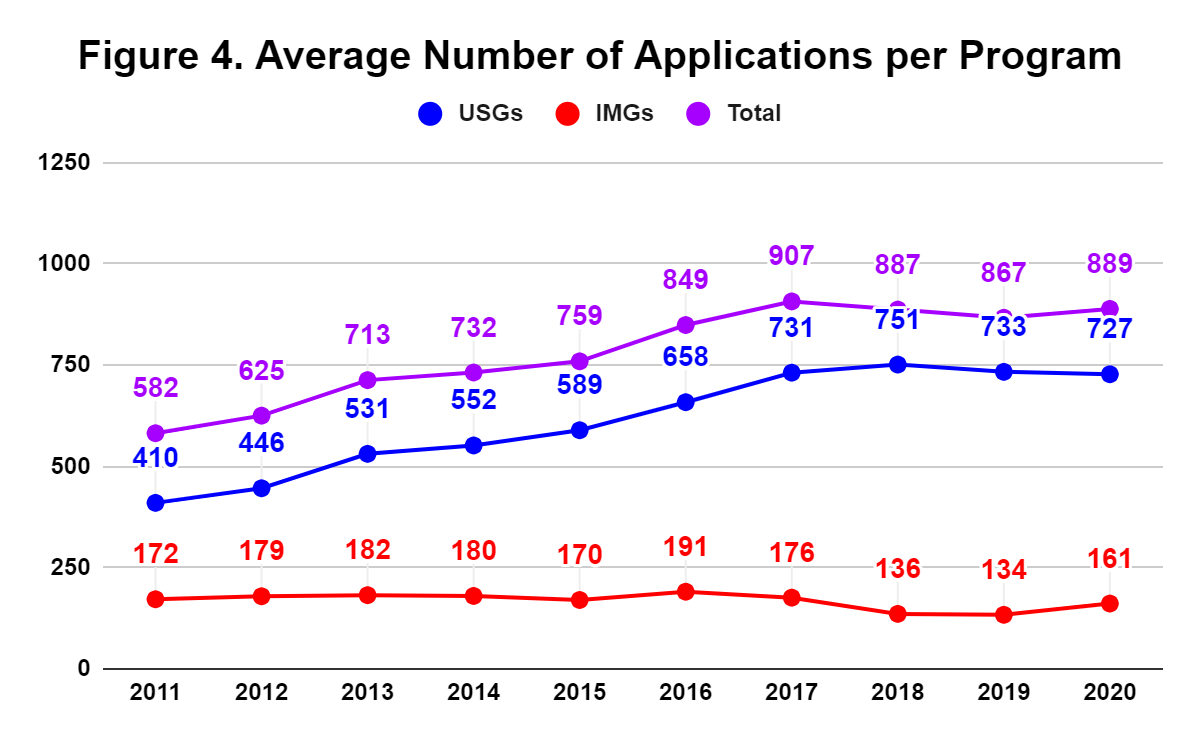
Although these data paint a picture of this year’s application cycle in broad strokes, the competitiveness of individual programs will inevitably vary a great deal. Hopefully, this review has given you a more accurate perspective of how this year compares to the last decade and where you stand compared to other applicants.
Stay tuned for next month’s newsletter, where I will dive into how competitive EM is compared to other specialties. The answer may surprise you. And, as always, good luck to all the fourth-years currently on the interview trail.
Reference:
Preliminary data published by AAMC available at: https://www.aamc.org/system/files/2019-10/services-eras-preliminary-data-counts-residency-applicants-specialty-year-10172019.xlsx [XLSX file]
Related Content

Apr 08, 2021
Near Death by Nasal Packing: A Rare Complication Due to the Fatal Trigeminocardiac Reflex
Epistaxis is a complaint that is frequently seen in the emergency department. As a physician, we took an oath to do no harm, but what if we end up doing more harm than good when managing epistaxis?
Apr 08, 2021
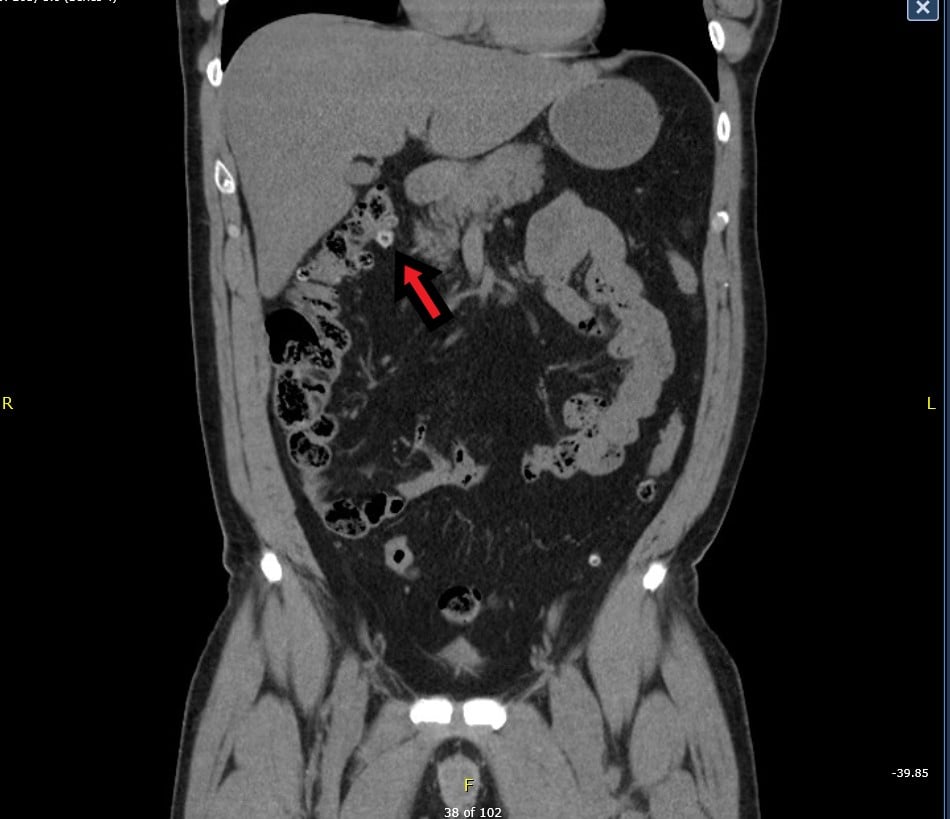
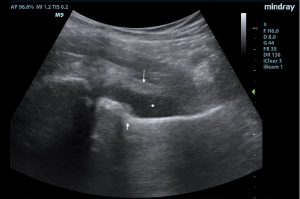
Pediatric Gonococcal Hip Arthritis Diagnosed by Emergency Point-of-Care Ultrasound-Guided Arthrocentesis
Point-of-care ultrasound-guided arthrocentesis performed in the emergency department can expedite the diagnosis and treatment of septic arthritis, potentially averting the need for surgery.




