The Growth of Hyperbaric Medicine in Emergency Medicine
Collin Brooks, MSIII - Wayne State University School of Medicine
EMRA MSC Great Lakes Regional Representative, 2021-2022
Danielle Andrews, MSIII - Loyola University Chicago Stritch School of Medicine
EMRA MSC Great Plains Regional Representative, 2021-2022
What words come to mind when you hear hyperbaric medicine? “The bends”, “diving”, “bubbles”? If these did, you wouldn’t be too far off!
Hyperbaric oxygen therapy is a well-established treatment for decompression sickness, which is a common occurrence in scuba divers. But it’s also a phenomenal treatment option to treat a plethora of other conditions including gas emboli (air bubbles in the blood), carbon monoxide poisoning, crush injuries, protracted wound healing, osteomyelitis, post-radiation injuries, skin graft/flap healing, and many other conditions. A hyperbaric medicine physician will see patients with a wide array of pathophysiology.
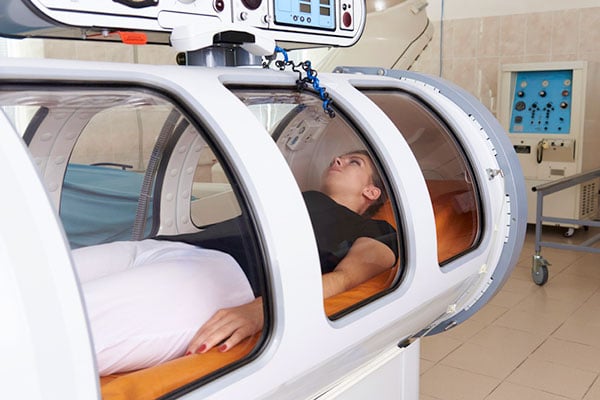
So how does it work? Patients who qualify for hyperbaric therapy are placed into a chamber to breathe 100% oxygen where the air pressure is 2-3 times greater than that of room air. Many physicians describe the sensation being similar to diving deeper underwater or when you come down from an airplane at about 10,000ft. Since room air consists of about 21% oxygen, the chamber significantly increases the amount of oxygen taken up by the lungs with each breath. The added gaseous pressure also forces more oxygen to be absorbed and dissolves into the plasma so that more oxygen circulates into the body and permeates through the organ tissues that may be hypoxic. Increased oxygen can stimulate angiogenesis, development of new blood vessels, which will then cause more blood, oxygen, and growth factors to enter hypoxic areas of the body to promote wound healing by making more scar tissue. For chronic wounds such as diabetic foot ulcers, wound healing is in part stunted by a lack of an oxygen gradient and chronic hypoxia around the tissue. By reintroducing oxygen to that area to reestablish an oxygen gradient, the body is signaled to start laying down new tissue layers to that area.
This in no way is an instantaneous process and generally patients need multiple sessions in the chamber to start seeing results and improvement in their condition. Typically, patients will lay flat in the chamber for anywhere between 90 minutes to 2 hours with nothing allowed but a water bottle to reduce contamination. Many places have a TV so patients can relax or take a nap during treatment. Commonly, patients must undergo anywhere from 20-40 sessions which breaks down to treatment Monday through Friday for about 6 to 8 weeks.
Undersea and hyperbaric medicine is defined as the therapeutic use of oxygen under pressure to treat disease. The history of hyperbaric medicine is rather unique. Caisson disease was first studied during the building of the Brooklyn Bridge in the 1800s. Physicians then began to create dive tables in order to increase the safety of divers in the era. Many years later, in the year 2000, the American Board of Emergency Medicine began to board-certify physicians in undersea and hyperbaric medicine.
In the modern day, hyperbaric medicine continues to be a field of innovation and growth. There are currently eight institutions that offer fellowship training in undersea and hyperbaric medicine, as well as three institutions in the process of starting new programs. Duke University School of Medicine, SUNY Upstate Medical University, UC San Diego, and University of Pennsylvania Medical Center are just some examples. Fellowships are one year and undersea and hyperbaric medicine has ACGME board certification requirements. Following training, physicians have many career options. You would be able to split time between various departments. Hyperbaric medicine physicians classically describe their career as a mix of emergency medicine, wound care, and hyperbaric medicine. Physicians also have the ability to work and research at an academic center or a community program.
Daily responsibilities of fellowship can include (1) determining the depth, duration, breathing gas mixture, and frequency of treatment for patients, (2) evaluating changes to pulmonary function following hyperbaric environment treatments, (3) wound care, (4) addressing patient care of chronic illness in a multidisciplinary approach, and (5) assessing for oxygen toxicity, and much more.
For more information be sure to check out the Undersea and Hyperbaric Medicine section of the EMRA Fellowship Guide!
Related Content

Jul 14, 2023
Surf Medicine: Perspectives, Potential Hazards, and the Importance of Preparedness
As the popularity of surfing grows, the incidence of surf injuries — both minor and traumatic — will increase accordingly. Knowledge and awareness about the breadth of potential injuries is essential to preparedness among care providers in surfing communities around the globe.

Feb 12, 2023
Emergent Diving Injuries: A Standardized Approach to Assessment
This article aims to provide a standardized approach to assessing diving-related injuries. We’ll first review the unique aspects of a history critical to diagnosing diving-related injuries. We’ll then present two very general chief complaints and work through a list of differentials to consider, each associated with a specific phase of a dive.