Implications of Emergency Care post Roe v. Wade
EMRA Southeast Regional Medical Student Council Representatives
Shilpi Ganguly, MS-IV, University of Miami Miller School of Medicine, EMRA MSC Southeast Regional Coordinator 2022-2023
Matthew Lyons, OMS-IV, Lincoln Memorial University-DeBusk College of Osteopathic Medicine, EMRA MSC Southeast Regional Representative I 2022-2023
Daniel Aloise, MS-IV, Florida International University Herbert Wertheim College of Medicine, EMRA MSC Southeast Regional Representative II 2022-2023
On June 24th 2022, the United States Supreme Court in a 5-4 decision, overturned Roe v. Wade, the nearly 50-years-old landmark decision which established the constitutional right to abortion. This decision came on the grounds that the right to an abortion is not “deeply rooted in this nation’s history or tradition.” Many have expressed anger and anxiety over the recent ruling, while others have rejoiced. One thing holds certain, regardless of where one stands on the spectrum, as emergency medicine physicians, it is important to consider how this decision will impact patients, and how it may affect our ability to provide comprehensive care.
With the new ruling, the question of abortion rights now sits within the hands of each individual state, creating a wildly diverse climate with regards to reproductive healthcare access across America. Sixteen states and the District of Columbia have laws that protect the right to abortion. Thirteen states have initiated “trigger laws,” where abortions or nearly all abortions are subject to being banned in some shape or form. Other states sit somewhere in between. Extreme examples include states such as Kentucky, where a trigger law passed in 2019 bans abortion outright and makes it a class D felony to provide abortions within the state. Similarly in Wisconsin, although there is no trigger law, a state law written in 1849 banning abortions has essentially become the new law of the land post-Roe. Across the nation, there has been major pushback against some of these more extreme laws. Ultimately, given the legal implications associated with providing abortions and the dynamic movement of these legal proceedings, it is imperative that healthcare providers continue to educate themselves regularly to stay up to date on the practices of their individual states.
Emergency physicians in particular may be some of the first providers to experience the impact of these new laws on the healthcare system. Nearly one in four women in the United States undergo an abortion at some point in their lifetime. However, most emergency physicians have likely had little exposure to complications of abortions given patients in the United States have historically had access to safe abortions across the nation. An “unsafe abortion,” as it is termed by the World Health Organization, is something that has been studied in developing countries for some time and is defined as “the termination of a pregnancy by people lacking the necessary skills, or in an environment lacking minimal medical standards, or both.” Not surprisingly, unsafe abortions have been associated with higher rates of complications, including incomplete abortion, severe hemorrhage, infection, and uterine perforation. As the gateway to the hospital, especially for socioeconomically disadvantaged patients, the emergency department could begin to see a tremendous increase in conditions associated with unsafe abortions. This fear is well illustrated by the evolution of abortion laws in other countries, such as Romania. Prior to 1966, abortion was legal in Romania and the abortion mortality ratio was 20 per 100,000 live births. Legal restrictions were placed on abortion in 1966, and by 1989 the abortion mortality ratio had increased to 148 per 100,000 lives births.
As emergency physicians, we are our patients’ biggest advocates and often some of the most heavily impacted by social implications of new legislature and judicial rulings. Hospitals serve as a safe place for our patients, with many coming to the ED on their worst days and in their most vulnerable states, expecting us to provide them with both stabilization and reassurance. In this new era, it is our duty to be prepared to face the inevitable changes coming to our emergency rooms. For states with stringent restrictions, we must be prepared for the uptick of gynecologic emergencies secondary to unsafe abortions. For states with protected access, we must be prepared for the surge of patients who will inevitably be travelling across state lines in hopes of receiving the gynecologic care they need. Physicians across America are seeking legal counsel to assist in medical decision making, in fear of doing something that may cause them to lose their licenses or worse, end up in jail. These situations highlight just a few of the innumerable impacts this new ruling will surely bring on emergency care for women and their providers alike.
As it stands, this supreme court decision has received significant backlash from the medical community. This ruling not only places restrictions on the freedoms of American women, but directly impacts the physical health and mental well-being of countless across the country and limits the freedom of medical decision making. Doctors across the nation from all specialties have begun speaking for what they believe in. As emergency medicine providers and members of such a dynamic specialty that interfaces so closely with the public, it is our duty to use our voices to advocate for our patients well beyond the walls of the hospital. Together, we can enact change on a national level and continue to help our patients in their most intimate and vulnerable times.
References:
- https://www.guttmacher.org/article/2022/06/13-states-have-abortion-trigger-bans-heres-what-happens-when-roe-overturned
- https://www.acep.org/federal-advocacy/federal-advocacy-overview/regs--eggs/regs--eggs-articles/regs--eggs---june-28-2022/
- https://www.acep.org/federal-advocacy/federal-advocacy-overview/regs--eggs/regs--eggs-articles/regs--eggs---june-28-2022/
- https://www.healthline.com/health-news/roe-v-wade-the-mental-and-physical-health-effects-of-anti-abortion-laws#What-happens-when-abortion-access-is-denied?
- https://en.wikipedia.org/wiki/Roe_v._Wade#:~:text=Roe%20v.%20Wade%2C%20410%20U.S.,choose%20to%20have%20an%20abortion.
- https://www.annemergmed.com/article/S0196-0644(20)30747-2/pdf
- https://www.who.int/news-room/fact-sheets/detail/abortion
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2709326/
Related Content
Dec 12, 2021
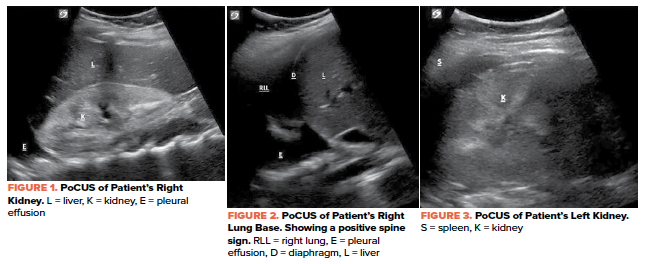
POCUS for the Win: Focal Segmental Glomerulosclerosis
Point of care ultrasound can be used to help evaluate patients with suspected kidney pathology and to diagnose causes of renal colic, renal failure, hematuria, and decreased urine output. Compared to computed tomography (CT), ultrasound can result in shorter lengths of stay, lower cost, and improved safety.
Dec 12, 2021
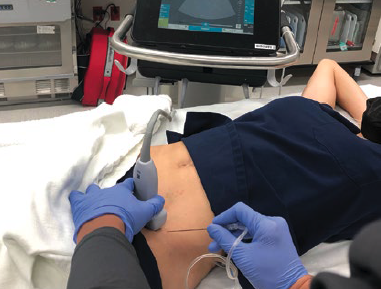
The Pericapsular Nerve Group (PENG) Block for Hip Pain
Hip fractures are common injuries evaluated in the ED. The majority of patients who suffer a hip fracture are over 80 years old, and as the population ages, the incidence of hip fractures is expected to increase. Do you have a strategy for managing this pain?
Dec 12, 2021
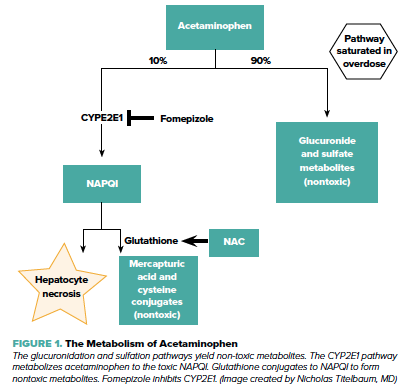
Fomepizole for Acetaminophen Toxicity: A Novel Use for a Classic Antidote
Acetaminophen toxicity is one of the most common causes of liver toxicity in the United States. New data reveals that fomepizole may be hepatoprotective in high dose acetaminophen toxicity when reviewed in animal models; will this affect management in humans?




