Ch. 3 - Third Year and Planning for Fourth
The start of your third year marks the first major transition into regular clinical responsibilities. It is an exciting time! You are able to apply your basic science knowledge to clinical practice, participate as part of a health care team, and regularly spend time with patients. At the same time, your responsibility increases, and more of your time is spent at the bedside rather than in the classroom. Your schedule will be more rigorous. The way you learn may need to evolve. Your performance in core rotations is a critical part of your residency application, so performing well is important. You will also be simultaneously planning your fourth year, which can be both exciting and stressful. What is the key to success during your clinical years? Advanced planning.
Third Year
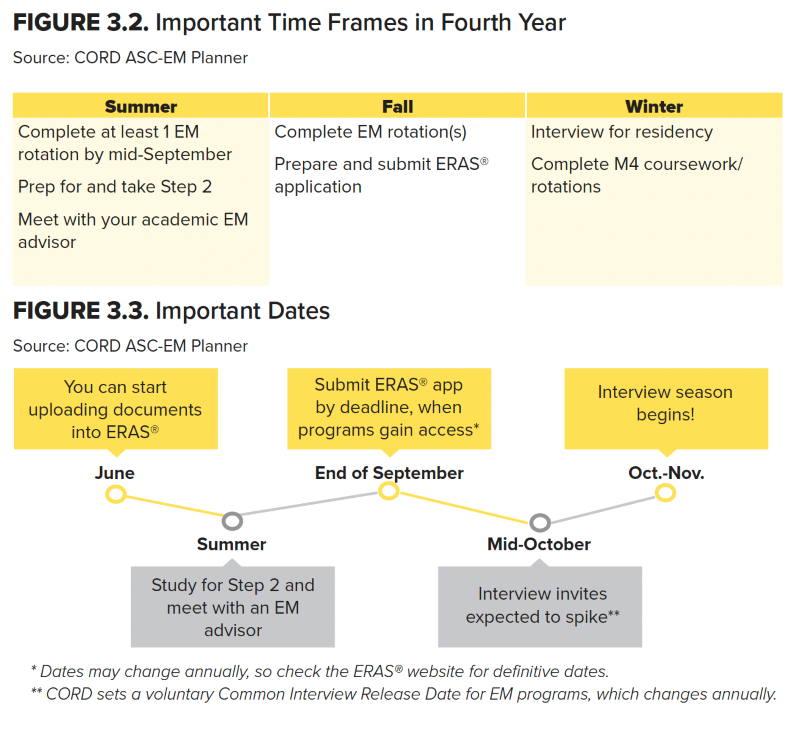
Figure 3.1 Important Time Frames in Third Year
Source: CORD ASC-EM Planner

Military Match: If you are a military match candidate, the timeline is accelerated. Applicants should research rotations early (summer of third year) and plan to rotate much earlier than non-military peers. You will be applying for and scheduling rotations in the winter!
IMG Candidates: Ensure paperwork is completed in time to allow for U.S. rotations. Consider researching away rotations as early as possible (summer of third year) so you can apply preferentially to institutions that accept your visa.
Couples Match: Meet with your advisor (individually and as a couple) to discuss career goals and how to increase your competitiveness as a couple. Consider these questions: What does couples matching mean to you? What compromises are you willing to make? What compromises are you not willing to make?
Latecomers: If you are undecided about your specialty but considering EM, meet with an EM advisor early in third year to discuss your options.
Academic Performance in Core Clerkships
Performing well in your core clerkships is critical for a number of reasons.
Making the most of your rotations and performing at a high level will:
- Accelerate your Step 2 preparation
- Allow you to apply your knowledge to patient care during your EM rotation(s)
- Make you a more competitive applicant
Narrative comments from your evaluations and information about your performance relative to your peers will be included in the MSPE, also known as the Dean’s letter. Per NRMP Match data from the 2021 Program Directors Survey, 70% of PDs cited “grades in required clerkships” as an important factor when selecting applicants to interview, with a mean importance rating of 3.9 out of 5.1 AOA and other honor society selection committees will also heavily consider your core clerkship performance. Lastly, your grades will impact your final class rank. One study found EM rotation performance and AOA designation were predictors of top performance in residency.2 Additionally, EM rotation grades have been shown to correlate with rank list position.3
What does all of this really mean?
It means preparation for Step 2 and your EM rotations begins now, with your core clerkships. With each rotation you are building your knowledge base and residency application.
At-Risk Candidates: Failing a clerkship is a major red flag. Nearly all programs reported “rarely or never” interviewing applicants with a clinical course failure, according to a recent CORD ASC-EM survey of EM educators.4 A clerkship failure should prompt consideration of a non-EM backup plan and a meeting with your academic EM advisor. Alternatively, performing at a high level on clerkships can help mitigate the effect of a failure on USMLE Step 1 or COMLEX Level 1.
Core Clerkship Pearls
Set yourself up for success on your core rotations — because all of them will ultimately help you be a better emergency physician. First, you can ask peers what worked well for them. What books did they read? Did they use any other resources? Next, make sure you review the syllabus and grading criteria. If a large part of your grade is exam performance, then creating a study plan for that rotation is important. And finally, be sure to ask for feedback from faculty and the clerkship director so you can identify areas for improvement early. Clerkship directors can help you come up with a plan to address these areas.
Table 3.1 Core Clerkship Pearls
Surgery — Success is all about dedication and preparation. Learning how to tie sutures before the start of your rotation is essential. Arrive early to pre-round, take time to “own” your patients, and absorb all you can about post-operative care. Don’t avoid the operating room; there you’ll learn valuable lessons on procedures (chest tubes, central lines, tracheostomies, etc.). Be sure to participate in clinic, too! Learning to evaluate wounds and manage postoperative complications is important. Examine any patient who is presenting for emergency surgery, as learning how to recognize an acute abdomen is a critical skill.
OB/GYN — You will deliver babies as an emergency physician! Make every effort to get hands-on practice while on your rotation. Pay particular attention to the techniques used in difficult deliveries (like shoulder dystocia). Also, practice reading fetal monitoring strips every day, as this is a skill commonly tested on your shelf exam. Ask if you can perform cervical checks during labor to get a sense of the degree of dilation and understand the various stages of labor. Being sensitive to gynecologic complaints and expertly and gently performing a pelvic exam is an essential skill in the ED. Lastly, participate in the care of patients with bleeding in pregnancy and pre-eclampsia, as well as postpartum patients with complications or breastfeeding concerns — these patients often present to the ED after-hours.
Psychiatry — EM physicians care for patients with a variety of mental health concerns, and many of these patients have limited access to care. Learning how to help patients find community resources is key. Also, learning how to identify those in acute psychosis or with a true psychiatric emergency is crucial. While rotating, try to become an expert in psychiatric medications, their dosing, interactions, and long-term and life-threatening side effects.
Pediatrics — Although there are many things to memorize during your pediatric rotation (such as developmental milestones and immunization schedules), there are also EM-specific pearls. Learn the basics such as normal and abnormal vitals for different age groups, how to properly perform nasal suction on infants or toddlers, and how to counsel families on safe-sleep habits. Take time to learn the basic treatment regimens for asthma, congenital abnormalities and their physiology, and changing physical exams at different ages.
Family Medicine/Internal Medicine — Understanding the hospital course and basic disease processes for the most common illnesses is crucial. During your IM rotation, it is important to take responsibility for your patients. Know their labs from three days ago, their vitals for the past 24–48 hours, and, most importantly, ask the nursing staff how they are doing. Your IM rotation hinges on collaboration between you and the entire health care team. Family medicine rotations vary at different institutions. While rotating, try to become an expert in antihypertensive and diabetes medications, including their indications, dosing, interactions, and side effects.
Dean’s Letter/Medical Student Performance Evaluation
The MSPE is an aggregation of all of your medical school accomplishments and is compiled by your home institution. This letter places a heavy emphasis on your core clerkship performance and feedback, as well as highlights your background, preclinical performance, and any service work or publications you may have. Core clerkship performance is critical, with many MSPEs providing summative rotation comments and a visual representation of your performance compared with your peers (typically a series of bar graphs or charts). According to the 2021 NRMP survey, 77% of PDs cited the MSPE as an important factor when selecting applicants to interview, with a mean importance rating of 3.8 out of 5.1 Most schools offer you the opportunity to review your MSPE before it is sent out. It is important to be aware of the content of your MSPE because below-average performance or potentially negative comments could be seen as a red flag and should be discussed early with your academic EM advisor. Additionally, interviewers might ask you about them. If you’re aware of any potentially problematic comments, you will have the opportunity to prepare how you might discuss them in an interview.
Planning for Your Emergency Medicine Clerkships
As an EM-bound student you should complete two EM rotations so you have two letters of recommendation (in EM we refer to these letters as eSLOEs, electronic Standardized Letters of Evaluation; see Chapter 6: Crush Your EM Clerkships, Secure Your SLOEs). While most required EM rotations are during fourth year, some EM rotations are offered during third year. Also, some schools with a required fourth-year EM rotation may allow students to rotate early (as an M3) if they have met the prerequisites. The experience gained on an EM rotation during the third year of medical school varies based on school, program, and timing. For example, if you rotate in the last month or block of M3, after all core rotations, that is much different than rotating in November of M3 before your surgery and pediatric rotations.
If your school offers or requires a third-year EM rotation, or permits you to schedule the M4 rotation as an M3, find out if they will write an eSLOE. Some institutions will not provide an eSLOE for M3s. If an eSLOE is an option, be sure to ask if the eSLOE will compare you to other M3s or to the M4 cohort — the added experience, confidence, and clinical competence of the M4 group may diminish your evaluation. An experienced EM advisor can help answer some of these nuanced questions, as each student’s circumstances are unique.
Ideally, you will complete your home institution (“home EM”) rotation first to get your feet wet before your away EM rotation. Unfortunately, EM is not a required rotation at all medical schools, so this isn’t always possible. If you do not have a home EM rotation with an ACGME-affiliated residency program, your only options will be away rotations. Late fall and early winter of your third year is the best time to start researching away EM rotations. EMRA Clerkship Match is a great place to start when researching programs.5 Alternately, use the EMRA Medical Student Advising Resources for Away Rotations to find even more specialized opportunities, such as international student rotations, diversity-oriented spots, and more.
There is more than one method for you to apply for away rotations. Some schools use the Visiting Student Learning Opportunities (VSLO), a centralized application service offered by the AAMC. Other schools have an “in-house” process that is unique to their school. “Participates in VSLO” is a filter on EMRA Clerkship Match, so you can easily find out which school uses which system. Clerkships that do not participate in VSLO will usually discuss how to apply for a rotation on their website.
The most critical thing is that you have at least one EM rotation completed in time to have an eSLOE from an ACGME-affiliated residency program in your file before ERAS applications are released to programs (usually in mid- to late September. (See Chapter 5 for more detailed information.)
Military Match: The timeline is accelerated. Applicants should research rotations early and plan to rotate as early as January of M3. Military rotations are set up by contacting the program directly via email.
Osteopathic and IMG Candidates: Be aware that your school may not have a home rotation so you must spend time researching academic programs with a history of accepting osteopathic and IMG applicants — EMRA Match can help with this. Start EARLY because you will need two away rotations in lieu of one that others are searching for.
Latecomers: Work with your EM advisor or clerkship director if you are having difficulty scheduling rotations. They can be an invaluable resource of experience and connections.
Fourth Year
IMG and At-Risk Candidates: Have two (instead of a minimum of one) rotations completed early so that both eSLOEs are in ERAS on the opening day for programs. Program leaders responsible for interviewing applicants recommend 2–3 eSLOEs for IMG applicants.
Military Match: The timeline is accelerated. The Match takes place in December of fourth year. Apply and be prepared to interview at civilian programs in late December/early January in case you don’t match into a military program.
Latecomers: Even if you do not have a completed eSLOE by opening day, do not delay in submitting your ERAS application. Only 15% of programs reported that it was “highly likely” that an application would be reviewed if it were completed after the ERAS opening date in September.6
USMLE Step 2
Preparing for USMLE Step 2 begins during pre-clinical courses and spans all of your core clinical clerkships. Your daily efforts to make the most of your rotations and master the learning objectives will save you time in the long run. In considering Step 2 preparation, take some time to reflect on your USMLE Step 1/ COMLEX Level 1 and clerkship exam performances: What worked well (or not)? What were your lessons learned? Residency programs are evaluated on the rate at which their graduates pass their board exams when they finish residency. It has been demonstrated for many specialties, including EM, that not passing a USMLE or COMLEX exam is a strong predictor of struggling to pass later exams.7 This correlation leads PDs to worry about applicants who struggle with these types of knowledge assessments. According to the 2021 NRMP PD survey, 77% of respondents listed USMLE Step 2 (and COMLEX Level 2 scores) as a factor in offering interviews.1 Further, USMLE Step 2 scores were given a mean importance rating of 3.8 out of 5 (compared to 3.5 for USMLE Step 1). Because of its clinical focus, USMLE Step 2 is often considered to be at least equally important as USMLE Step 1.1,4 The bottom line is USMLE Step 2 performance is very important — your work is not done after Step 1/Level 1! With USMLE Step 1 and COMLEX Level 1 moving to pass/fail, the importance of having a Step 2 score in your file when ERAS opens to programs is unknown at this time of publication. Per NRMP data from previous Match cycles, 23% of programs do not require Step 2 scores when deciding whom to interview.1 However, that means 77% do put some weight on this exam before granting an interview. Without a numerical score for Step 1/Level 1, many advisors think the importance of Step 2 will increase. As a result, we recommend you take Step 2 early enough that the scores will be in your file before late September when residency programs start to review applications. Also, keep in mind that as you progress through your fourth year, it may be more challenging to find time to study during away rotations, while preparing your application, or between interviews. If you failed Step 1 or Level 1, make sure you have met with an advisor and/or consulted with your office of student affairs and come up with a plan to take the exam again and pass. You might benefit from additional time in the form of a study month, or your school may offer other resources to help you prepare. Working with an EM advisor is crucial — a USMLE or COMLEX failure is a red flag and more likely than not warrants a backup plan. In addition, if you failed Step 1/ Level 1, it is recommended you attempt to bolster your application by taking Step 2 early (end of June or mid-July) so your scores are available to programs when ERAS applications are released. A good Step 2 score may help compensate for a Step 1/Level 1 failure. The mean Step 2 score for U.S. MDs matching into EM is 247 and 232 for those who went unmatched.8 Even if you passed Step 1/Level 1, most programs require a Step 2 score before the rank list deadline.2
Latecomers: Prioritize getting your first eSLOE over taking Step 2 early. Both are important, but studies show the eSLOE is more important in offering interviews.1,3,6,11-12
In general, it’s probably best to allow yourself time to focus on Step 2 and EM rotations independently. However, since there is significant overlap in the period for completion of each, this may not be possible. Your school may have deadlines that mandate a completion date during an eSLOE-granting EM rotation. For those who feel a dedicated study month (or two weeks) is needed, this should be done only if timing allows for scheduling at least one EM rotation over the summer months. Remember, your goal is to have at least one eSLOE, but preferably two, uploaded to ERAS by opening day.
Osteopathic Candidates: As there is no reliable score conversion from COMLEX to USMLE, there are still residency programs that prefer USMLE scores over COMLEX scores alone, although the gap is closing. To be compared apples-to-apples with your allopathic counterparts and open more opportunities for residency interviews, it is recommended that you take USMLE Step 2 early to have your score available when ERAS opens.9,10 As an osteopathic student, you do not need to take USMLE Step 1 in order to take USMLE Step 2.13
Fourth Year Coursework
EM rotations will take up at least two months of your year. Schedules don’t always align between schools, so you may find yourself with an odd week or two as you set up your away rotation(s). Work with your Dean’s office to see what options you may have if your away rotation schedule doesn’t align with your school’s schedule — some schools are flexible about this, but some are not. Your school may also have required coursework. Students are typically able to enroll in electives with flexible scheduling or take time off for interviews.
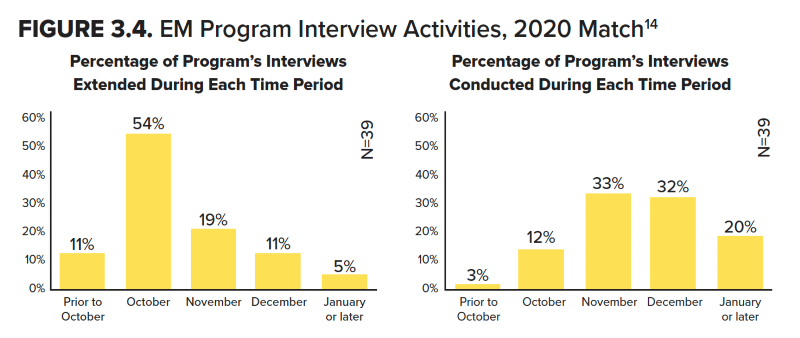
According to the 2020 PD survey for the 2019–2020 interview season, the majority of interview invites were sent in October (54%) and November (19%), and interviews were conducted in October (12%), November (33%), December (32%), and January (20%).14 Speak with your advisor or upper-year mentors who have gone through the specific coursework at your school to determine which electives are best for interview season in terms of flexibility for interviewing.
For any rotations during interview season, be sure to communicate with as much advance notice as possible regarding your interview schedule. Keep in mind that most courses or rotations have attendance requirements.
After you have completed your two EM rotations, consider broadening your coursework. As an EM physician, you will need to draw upon a broad skill set during your career. Both EM and non-EM electives can help you build important skills.
Figure 3.4 EM Program Interview Activities (n=84)
EM Subspecialty Electives
To further explore your interests in the field of EM, consider an elective in a related area. There are several clerkships in EM subspecialty areas including ultrasound, pediatric EM, toxicology, EMS, wilderness medicine, etc. Such rotations will help you expand your knowledge base and can also help you to get to know another program’s faculty and residents. They also open your eyes to the versatility of a career in EM and help build your excitement for residency and beyond. While subspecialty rotations often provide a letter of recommendation (known as an EM subspecialty SLOE), these letters are not given the same weight as a traditional eSLOE because they reflect your performance in a narrow area within EM. However, it is still important to request a SLOE from an EM subspecialty rotation to submit with your ERAS application.
IMG Candidates and Latecomers: For applicants struggling to get 1-2 (or any) rotations that can provide a traditional group eSLOE, a SLOE from a non-residency based EM rotation or an EM subspecialty elective in order to obtain an EM subspecialty SLOE will be the next best options.
Non-EM Electives
Ophthalmology
Eye complaints in the ED can be challenging for several reasons. Consider completing an ophthalmology rotation to become proficient at slit lamp examinations. Eye foreign bodies, ocular trauma, and vision loss complaints all warrant a good slit lamp exam. Additionally, learning how to use fluorescein and measure intraocular pressure will certainly put you a step ahead as an intern.
Orthopedics
Performing a complete musculoskeletal exam as well as recognizing and reducing fractures and dislocations are crucial skills for any emergency physician. A rotation in ortho can also help you communicate effectively with your consultants in the ED. Learning fracture types (Smith’s fracture vs. Colles’ fracture, Weber classification, etc.), the nomenclature of specific bony areas, and key information for your consultant will make your interactions with orthopedics colleagues much smoother. Absorb all you can about splinting and casting! Our orthopedic colleagues have a wealth of information on the best ways to immobilize fractures and are usually very willing to teach you.
Dermatology
Take this opportunity to learn how to recognize life-threatening rashes and lesions that may be indicative of serious diseases. Ask about the outpatient medical management of common rashes and skin complaints, and try to learn what needs emergent consultation vs. close follow-up.
Pulmonology
Working with a pulmonologist can provide a fascinating insight into what happens to our respiratory distress patients after they are admitted. Learning about how a ventilator works and how to set/adjust ventilator settings is a critical skill and cannot be overestimated. Be sure to observe a bronchoscopy whenever possible to gain a better understanding of the respiratory tree and the extensive sequelae of lung diseases. Pay particular attention to the medication and home care of patients so you can help counsel your patients who have frequent visits for COPD or asthma exacerbations.
Cardiology
Evaluating patients with chest pain is bread and butter emergency medicine. A cardiology rotation can help you learn more about evaluating for acute coronary syndrome, reading ECGs, performing and interpreting echocardiography, and learning more about how patients are evaluated for cardiac problems outside the ED (stress tests, catheterizations, etc.).
Critical Care
ICU experiences can provide opportunities to learn new procedural skills, such as placing arterial and central lines. Managing patients on ventilators and various medication drips is a key skill for EM physicians. You can learn about ICU admission criteria and the care and treatment of patients with conditions commonly encountered in the ED such as sepsis, multisystem trauma, stroke, etc. Different ICU experiences like trauma ICU, cardiovascular ICU, neuro ICU, or surgical ICU can diversify your education.
The Human Side of Medicine
The medical knowledge and clinical skills needed for EM are extensive, but communication, professionalism, and interpersonal skills will also be crucial in your career. They will likely contribute to your overall career satisfaction and even longevity. Take advantage of courses with a focus on palliative care, difficult discussions, or even how to be a better educator. This will make you a stronger EM physician, respected colleague, and patient advocate.
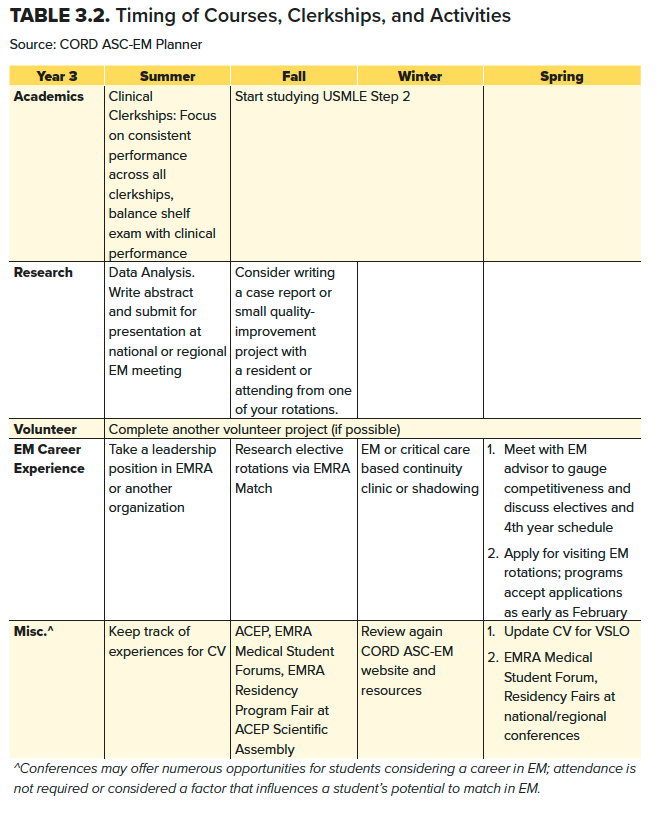
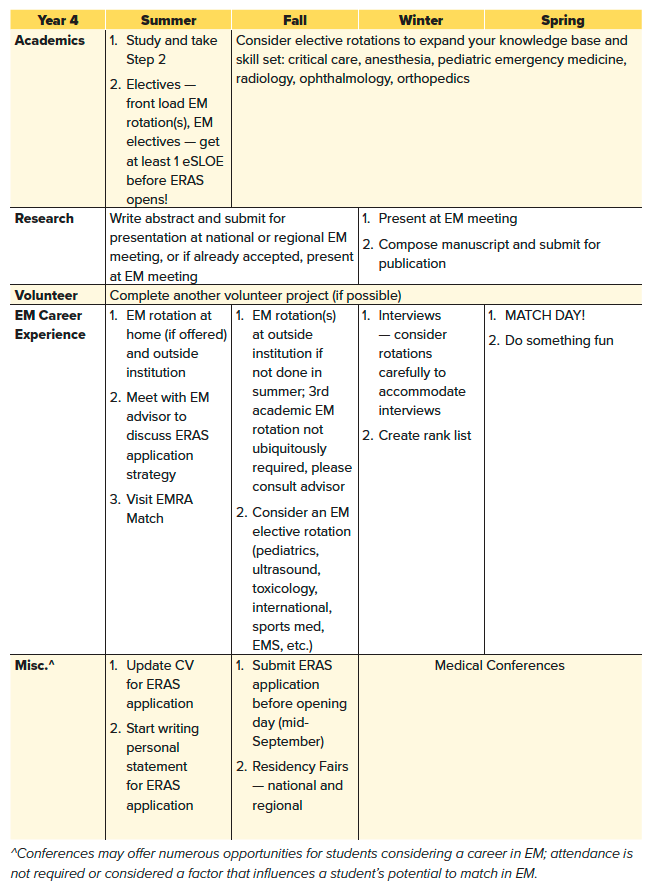
Table 3.2. Timing of Courses, Clerkships, and Activities
THE BOTTOM LINE
- Core clerkships are critical in helping you develop the knowledge and skills to succeed in EM and do well on Step 2. In addition, your performance will be highlighted in your MSPE and is important to EM PDs.
- Begin planning your fourth year early. This includes researching EM electives and brainstorming a strategy to prepare a complete ERAS application (When will you take Step 2? How many EM rotations do you need to complete before your ERAS application is due?).
- If you do not have an EM advisor now is the time to find one. An academic EM advisor can provide critical guidance on fourth-year planning. Students at schools without an EM residency or EM advising can email distanceadvising@cordjobboard.com.
References
- National Resident Matching Program Data Release and Research Committee. Results of the 2021 NRMP Program Director Survey.
https://www.nrmp.org/wp-content/uploads/2021/11/2021-PD-Survey-Report-for-WWW.pdf.
- Bhat R, Takenaka K, Levine B, et al. Predictors of a Top Performer During Emergency Medicine Residency. J Emerg Med. 2015;49(4):505-512.
- Breyer MJ, Sadosty A, Biros M. Factors Affecting Candidate Placement on an Emergency Medicine Residency Program’s Rank Order. West J Emerg Med. 2012;13(6):458-462.
- Pelletier-Bui AE, Schrepel C, Smith L, Zhang XC, Kellogg A, Edens MA, Jones CW, Hillman E. Advising special population emergency medicine residency applicants: a survey of emergency medicine advisors and residency program leadership. BMC Med Educ. 2020;20(1):495.
- Emergency Medicine Residents’ Association. EMRA Match. https://webapps.acep.org/utils/spa/match#/search/map. Accessed August 20, 2018.
- 8.National Resident Matching Program. Charting Outcomes in the Match: Senior Students of U.S. MD Medical Schools, 3rd ed. July 2022. https://www.nrmp.org/wp-content/uploads/2022/07/Charting-Outcomes-MD-Seniors-2022_Final.pdf
- 9.Lee AS, Chang L, Feng E, Helf S. Reliability and Validity of Conversion Formulas Between Comprehensive Osteopathic Medical Licensing Examination of the United States Level 1 and United States Medical Licensing Examination Step 1. J Grad Med Educ. 2014;6(2):280-283.
- 10.Sarko J, Svoren E, Katz E. COMLEX-1 and USMLE-1 Are Not Interchangeable Examinations. Acad Emerg Med. 2010;17(2):218-220.
- 11. Negaard M, Assimacopoulos E, Harland K, Van Heukelom J. Emergency Medicine Residency Selection Criteria: An Update and Comparison. AEM Educ Train. 2018;2(2):146-153.
- 12. Love JN, Smith J, Weizberg M, et al. Council of Emergency Medicine Residency Directors’ Standardized Letter of Recommendation: The Program Director’s Perspective. Acad Emerg Med. 2014;21(6):680-687.
- 6. King K, Kass K. What do they want from us? A survey of EM program directors on EM application criteria. West J Emerg Med. 2017;18(1):126-128.
- 7. Harmouche E, Goyal N, Pinawin A, Nagarwala J, Bhat R. USMLE Scores Predict Success in ABEM Initial Certification: A Multicenter Study. West J Emerg Med. 2017 Apr;18(3):544-549.
- United States Medical Licensing Examination. Who is Eligible to Take the USMLE Steps? . usmle.org. https://www.usmle.org/bulletin-information/eligibility. Accessed Sept 18, 2022.
- National Resident Matching Program Data Release and Research Committee. Results of the 2020 NRMP Program Director Survey. https://www.nrmp.org/wp-content/uploads/2022/01/2020-PD-Survey.pdf.





